With how to know if you need a root canal at the forefront, this article opens a window to a crucial dental emergency where timely intervention can mean all the difference between saving or losing a precious tooth. At the heart of every dental emergency lies a painful question: how to know if you need a root canal? The answer lies not just in the pain but in the underlying causes of that pain, which could be a deep decay, infected gums, or a cracked tooth.
This article aims to demystify the process of root canal treatment, exploring the causes of tooth pain, identifying warning signs, the role of X-rays, treatment options, and the costs associated with it. By understanding the importance of a root canal, you can make informed decisions to save your tooth, preventing the need for more complex and costly treatments in the future.
Understanding the Causes of Tooth Pain
Tooth pain can be a debilitating and worrying experience, and it’s essential to understand the underlying causes to determine the best course of action. In many cases, tooth pain is a sign that a root canal may be necessary.
Deep Decay and Tooth Infections
Deep decay refers to the progression of tooth decay into the pulp and dentin layers of the tooth. This can lead to tooth infections, which can be incredibly painful and may require a root canal to alleviate symptoms. The pulp contains nerves, blood vessels, and connective tissue, and when it becomes infected, it can cause severe pain and inflammation. If left untreated, a tooth infection can spread to other parts of the face and even the bloodstream.
- Infected Pulp: When the pulp becomes infected, it can cause severe pain, and the tooth may become discolored. In severe cases, the infection can spread to the surrounding bone and tissues, leading to swelling and abscesses.
- Swollen Gums: Infected teeth can cause the gums to become swollen and inflamed, leading to discomfort and pain. In some cases, the gums may bleed easily or become discolored.
Cracked Teeth and Tooth Fractures
Cracked teeth can be incredibly painful, as the crack can expose the pulp and cause it to become infected. Tooth fractures can also lead to the need for a root canal, especially if the fracture extends into the pulp. Cracked teeth can be caused by a range of factors, including biting or chewing on hard objects, trauma to the mouth, or even grinding and clenching of the teeth.
- Cracked Cusps: Cracks in the cusps of the teeth can cause pain and sensitivity, and may require a root canal to alleviate symptoms.
- Fractured Roots: In cases where the roots of the tooth become fractured, a root canal may be necessary to remove the infected pulp and prevent further damage.
The Importance of Oral Hygiene
Oral hygiene plays a crucial role in maintaining healthy teeth and gums. Good oral hygiene can help prevent tooth decay, reduce the risk of infections, and promote overall dental health.
- Regular Brushing: Brushing teeth at least twice a day can help remove bacteria and plaque from the surfaces of the teeth, reducing the risk of decay and infections.
- Flossing: Flossing can help remove food particles and bacteria from between the teeth, where a toothbrush may not reach. This can help prevent the buildup of plaque and reduce the risk of gum disease.
Remember, regular oral hygiene is key to maintaining healthy teeth and gums. By taking the time to brush and floss your teeth regularly, you can reduce the risk of tooth decay, infections, and other oral health issues.
Preventing Tooth Pain and Infections
Preventing tooth pain and infections can be achieved through regular oral hygiene, avoiding sugary or acidic foods and drinks, and visiting your dentist regularly for check-ups and cleanings.
- Avoid Sugary and Acidic Foods: Consuming sugary or acidic foods and drinks can lead to tooth decay and increase the risk of infections.
- Visit Your Dentist Regularly: Visiting your dentist regularly can help identify potential problems early on, reducing the risk of tooth pain and infections.
Identifying Warning Signs for Root Canals
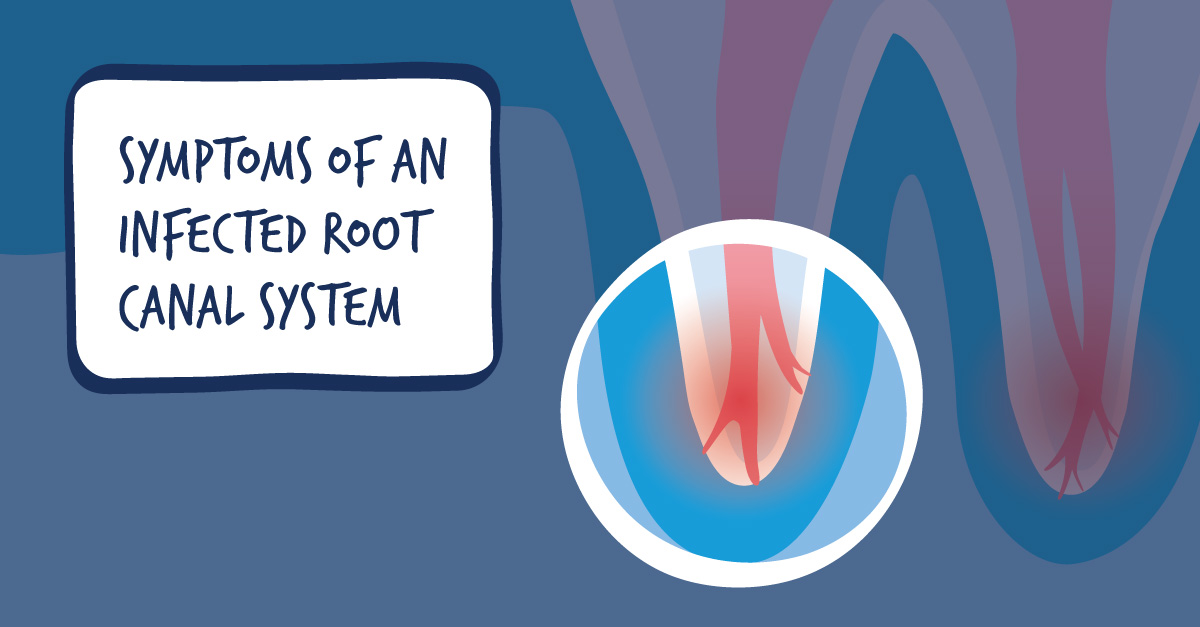
Root canals are a crucial dental procedure that saves natural teeth from extraction. However, identifying the warning signs of a potential root canal is essential to prevent further damage and complications. Delayed treatment can lead to severe consequences, including tooth loss, abscesses, and even systemic infections.
### The Difference Between a Toothache and a Root Canal
A toothache and a root canal have distinct symptoms, but often, they are confused with each other. A toothache is a sharp or dull pain that can be caused by decay, cracks, or gum disease. On the other hand, a root canal is a more severe infection that requires immediate attention. Here are some key differences:
####
Similar Symptoms and Their Significance
The symptoms of a toothache and a root canal can be alarming, but understanding their differences is crucial.
– Sensitivity: Both conditions can cause sensitivity to hot and cold temperatures. However, sensitivity during a root canal indicates a deeper infection that may require a root canal.
– Swelling: Swelling in the gums or face can occur in both a toothache and a root canal. But root canal swelling is often accompanied by other symptoms like pus and fever.
– Pain when biting: Pain when biting is a symptom of both conditions. However, in a root canal, the pain can be more severe and persistent, even after a night of rest.
### Case Studies: The Consequences of Delayed Root Canals
Delaying a root canal can lead to severe consequences. Here are some case studies that highlight the importance of early treatment:
* In one study, a patient with a root canal delay developed an abscess that led to a systemic infection. The patient required antibiotics and hospitalization.
* Another study found that delayed root canals increased the risk of tooth loss by up to 50%.
* A patient who delayed a root canal for several months suffered from persistent pain and swelling, which ultimately led to tooth extraction.
### Your Medical History: A Key to Recognizing Root Canal Symptoms
Your medical history plays a significant role in recognizing the warning signs of a root canal. A dentist can review your medical history to identify potential risk factors, including:
####
Risk Factors and Their Significance
Understanding your risk factors can help you recognize the warning signs of a root canal.
– Previous root canals: If you’ve had a root canal before, you’re more likely to experience complications.
– Diabetes: People with diabetes are more susceptible to oral infections, including root canals.
– Gum disease: Gum disease can increase the risk of root canal complications.
– Hormonal changes: Hormonal fluctuations during pregnancy or menstruation can increase the risk of root canal complications.
Recognizing these warning signs and risk factors can help you take proactive steps to prevent complications and ensure a healthier smile.
The Role of X-rays in Root Canal Determination
Determining the need for a root canal can be a complex process, and while visual inspections and symptoms play a significant role, X-rays are also crucial in identifying internal tooth damage that may not be apparent visually. X-rays allow dentists to evaluate the extent of tooth decay, cracks, or infections that may have caused the symptoms leading to the need for a root canal.
In many cases, X-rays will be taken as part of a routine checkup or emergency examination. Dentists will use these X-rays to identify internal tooth damage, such as cracks or infections, that may not be visible to the naked eye. A dentist may also use X-rays to evaluate the condition of the surrounding bone and tissue, which can help determine if a root canal is the best course of treatment.
X-ray Indicators of Internal Tooth Damage
A dentist may consider taking X-rays in several situations, including:
- A tooth that has been subjected to trauma or injury
- A tooth that has shown significant decay or cavities
- A tooth that is causing pain or discomfort, especially if the pain is related to biting or chewing
When evaluating X-rays, a dentist may look for several indicators of internal tooth damage, including:
- A dark or hazy appearance in the pulp chamber or canals, indicating a possible infection
- A widening or expansion of the pulp chamber or canals, indicating a possible crack or fracture
- A loss of definition or Artikel of the tooth structure, indicating a possible infection or decay
Interpreting X-rays for Root Canal Determination, How to know if you need a root canal
When interpreting X-rays for root canal determination, a dentist will consider several factors, including:
- The extent of tooth decay or cavities
- The presence or absence of cracks or fractures
- The condition of the surrounding bone and tissue
The dentist will use this information to make a diagnosis and determine the best course of treatment. In some cases, a root canal may be recommended to remove the infected or damaged tissue and prevent further damage or infection.
A typical X-ray that would indicate a root canal is necessary may show:
– Dark or hazy areas in the pulp chamber or canals, indicating a possible infection.
– A widening or expansion of the pulp chamber or canals, indicating a possible crack or fracture.
– A loss of definition or Artikel of the tooth structure, indicating a possible infection or decay.
The X-ray may also show a black or dark area inside the tooth where the pulp has died, this area is typically referred to as a ‘periapical cyst,’ these cysts are usually painless and can go unnoticed, but when detected, they can indicate the presence of an infected root canal.
In summary, X-rays play a vital role in determining the need for a root canal, by helping dentists identify internal tooth damage that may not be apparent visually. By evaluating X-rays, dentists can make an informed diagnosis and recommend the best course of treatment to prevent further damage or infection.
Exploring Root Canal Treatment Options
Root canal treatment is a complex procedure that requires careful planning and execution to ensure the best possible outcome. There are various types of root canal treatments available, each with its own set of advantages and disadvantages. Choosing the right treatment option depends on the individual case and the specific needs of the patient.
Types of Root Canal Treatments
There are three primary types of root canal treatments: single-visit, multiple-visits, and pulpectomy.
- Single-Visit Root Canal
- A single-visit root canal is a procedure where the dentist completes the treatment in a single appointment.
- This type of treatment is ideal for patients with a straightforward root canal anatomy.
- It is generally less expensive than multiple-visits treatment, but may require additional procedures if complications arise.
- Multiple-Visits Root Canal
- A multiple-visits root canal is a procedure where the dentist completes the treatment over several appointments.
- Each visit typically involves accessing the infected tooth, cleaning and shaping the root canal, and filling the canal with a medicated paste.
- This type of treatment is ideal for patients with complex root canal anatomy or infected teeth.
- Pulpectomy
- Pulpectomy is a procedure where the dentist removes the entire pulp from the tooth.
- This type of treatment is typically reserved for patients with severely infected teeth or those who have suffered pulp damage.
- Pulpectomy is often used in conjunction with a full-coverage crown or other restorative treatments.
The Importance of a Root Canal Specialist
A root canal specialist, also known as an endodontist, has received extensive training in root canal procedures and is equipped to handle complex cases. They have the skills to identify potential complications and take necessary measures to prevent them from arising.
The American Association of Endodontists recommends consulting an endodontist for root canal procedures, as they can ensure a higher success rate and provide personalized care.
A Patient’s Experience Undergoing a Root Canal
A root canal procedure typically begins with an initial consultation, where the dentist examines the tooth and creates a treatment plan. On the day of the procedure, the patient is given local anesthesia to numb the area, and the dentist accesses the infected tooth.
The dentist then cleans and shapes the root canal using specialized instruments, followed by filling the canal with a medicated paste. The dentist may use x-rays or other imaging techniques to confirm the success of the procedure.
After the treatment, the dentist will provide guidance on postoperative care, which may include taking pain medication, using a topical anesthetic, and maintaining good oral hygiene. In most cases, patients can resume their normal activities immediately following the procedure.
The recovery process is usually quick and straightforward, with most patients experiencing minimal discomfort. However, some patients may experience sensitivity or pain in the treated tooth, which can be managed with over-the-counter pain medication.
In rare cases, complications may arise, such as pain or swelling, which can be resolved with additional procedures or antibiotics. It is essential for patients to follow their dentist’s instructions carefully to ensure a smooth and successful recovery.
Preparing for and Recovering from Root Canal Surgery
Root canal surgery can be a daunting experience for many individuals. However, with proper preparation and care during the recovery process, patients can minimize discomfort and achieve optimal results. Many patients who have undergone root canal surgery have reported minimal discomfort during recovery. For instance, a patient who had a root canal on a molar reported feeling only a mild soreness on the day of the procedure, which subsided by the next day.
Preparing for root canal surgery involves a few key steps. Patients should schedule the procedure at the end of the day, as the anesthesia used during the procedure will leave them feeling numb for several hours. Additionally, patients should arrange for someone to drive them home after the procedure and stay with them for the remainder of the day. Eating a light meal or snack before the procedure can also help alleviate discomfort during recovery.
Alleviating Post-Operative Soreness
There are several ways to alleviate post-operative soreness after a root canal. Three effective methods include:
- Biting on gauze: Biting on gauze for 30-60 minutes after the procedure can help control bleeding and alleviate soreness.
- Over-the-counter pain medication: Taking over-the-counter pain medication such as ibuprofen or acetaminophen as directed by the dentist can help manage pain and discomfort.
- Applying ice packs: Applying ice packs to the affected area can help reduce swelling and alleviate soreness.
Post-Operative Care from Dentists
Dentists typically provide patients with a list of post-operative care instructions to ensure a smooth and comfortable recovery. These instructions often include:
- Avoiding strenuous activities for the remainder of the day
- Avoiding biting or chewing on the affected tooth
- Bruising the area with a salt water rinse for 24-48 hours after the procedure
- Returning for a follow-up appointment to ensure the tooth is healing properly
The Cost and Insurance Considerations of Root Canals
When considering a root canal procedure, the financial implications can be a major concern for individuals. Understanding the costs and insurance coverage can help make the process smoother and more manageable. In this section, we will discuss the costs associated with root canals, potential insurance coverage, and how to navigate copays and payment plans.
Cost Estimates for Root Canals
The cost of a root canal can vary depending on several factors, including the location, dentist’s experience, and the complexity of the procedure. On average, the cost of a root canal can range from $500 to $1,500 per tooth, with some procedures costing upwards of $3,000. It’s essential to note that costs can vary significantly depending on your location, with urban areas typically having higher costs compared to rural areas.
Insurance Coverage for Root Canals
Most dental insurance plans cover a significant portion of the costs associated with root canals. However, the extent of coverage can vary depending on your insurance provider and plan. Typically, insurance plans will cover around 50-80% of the cost, with the remaining amount paid out-of-pocket by the patient. It’s crucial to review your insurance plan’s details to understand what is covered and what is not.
Negotiating a Payment Plan
For individuals who cannot afford the upfront cost of a root canal, negotiating a payment plan with your dentist is possible. Many dentists and clinics offer financing options or payment plans that can help spread the cost over several months or years. It’s essential to discuss your financial situation with your dentist and explore options that work for you.
- Ask your dentist about available financing options or payment plans.
- Be open and honest about your financial situation, including income and expenses.
- Request a detailed breakdown of costs and what is covered by your insurance plan.
By understanding the costs and insurance considerations associated with root canals, individuals can better prepare themselves for the financial aspect of the procedure and make informed decisions about their dental care. Regular check-ups and preventative care can also help identify potential issues before they become more complex and costly.
A root canal procedure can range from $500 to $1,500 per tooth, depending on the location, dentist’s experience, and complexity of the procedure. Keep in mind that costs can vary significantly depending on your location, with urban areas typically having higher costs compared to rural areas.
Your dental insurance plan may cover a significant portion of the costs associated with root canals, typically around 50-80%. Be sure to review your plan’s details to understand what is covered and what is not.
By understanding your options and being open with your dentist, you can work together to find a payment plan that suits your financial situation and get the care you need.
Final Review: How To Know If You Need A Root Canal
In conclusion, a root canal is a lifesaver for a damaged or infected tooth. By knowing the warning signs and taking immediate action, you can save your tooth and prevent more severe problems down the line. Don’t hesitate to seek professional help from a dentist to determine if a root canal is necessary. Remember, a healthy tooth is a happy tooth!
FAQ Resource
Q: When should I go to the dentist for a root canal?
A: If you experience severe tooth pain, sensitivity to hot or cold foods, or swelling around the affected tooth, you should visit a dentist as soon as possible.
Q: What are the different types of root canal treatments?
A: The most common types of root canal treatments are single-visit root canals, multiple-visit root canals, and pulpectomies. Dentists will recommend the best type of treatment for you based on the extent of the infection.
Q: Can I get a root canal if I have a cracked tooth?
A: Yes, if your tooth is cracked, but the crack is not severe, a root canal might be possible. However, if the crack is extensive, a crown or extraction might be more suitable.
Q: Will my insurance cover a root canal?
A: Many insurance plans cover a significant portion of the cost of a root canal. However, the extent of coverage depends on your policy, so it’s best to check with your insurance provider before undergoing treatment.
Q: How long does it take to recover from a root canal?
A: Recovery time varies from person to person, but you can expect to feel better within a few days. You may experience some discomfort, swelling, or bleeding after the procedure, but these symptoms are usually temporary.