How long does it take for dry socket to heal sets the stage for this enthralling narrative, offering readers a glimpse into a story that is rich in detail and brimming with originality from the outset. The journey of healing from dry socket is a complex process that involves multiple stages, each with its unique set of challenges and opportunities for growth.
The symptoms of dry socket can be easily overlooked, especially during the initial stages, leading to misdiagnosis and prolonged healing times. The correct diagnosis of dry socket requires a combination of visual examination and X-ray visualization to determine the underlying factors that contribute to its formation.
Dry socket, also known as alveolar osteitis, is a painful condition that can develop after tooth extraction, particularly if proper oral care is not followed. It is characterized by the exposure of bone and nerve endings in the extraction site, leading to severe pain. Historical context indicates that dry socket has been a well-documented complication of tooth extraction since the late 19th century.
The underlying factors that lead to the formation of dry socket include:
The extraction site’s anatomy plays a crucial role in the development of dry socket. The presence of thin bone, incomplete clotting, and a higher concentration of nerve endings in the lower mandible increase the risk of dry socket.
The anatomy of the extraction site makes it more susceptible to complications, particularly if proper oral care is not followed.
- The thin bone in the lower jaw makes it easier for the clot to dislodge.
- Incomplete clotting can expose the nerve endings, leading to pain.
- A higher concentration of nerve endings in the lower mandible increases the risk of dry socket.
Smoking has been identified as a significant risk factor for dry socket. Tobacco smoke contains chemicals that can interfere with blood clotting, making it more likely for dry socket to develop.
Smoking is a contributing factor to dry socket, and its effects are often underestimated.
The risk of dry socket is increased threefold in smokers compared to non-smokers.
Certain medications, including anticoagulants, antiplatelet drugs, and steroids, can increase the risk of dry socket.
Medications can contribute to dry socket, especially when taken in conjunction with other risk factors.
| Medication | Risk Increase |
|---|---|
| Anticoagulants | 5-fold increase in risk |
| Antiplatelet drugs | 3-fold increase in risk |
| Steroids | 2-fold increase in risk |
Acute dry socket typically develops within 24 hours after extraction, while chronic dry socket can occur weeks or even months later.
The difference between acute and chronic dry socket lies in the timing and severity of symptoms.
- Acute dry socket develops within 24 hours after extraction.
- Chronic dry socket can occur weeks or even months later.
Symptoms of Dry Socket
Dry socket, also known as alveolar osteitis, is a painful and potentially debilitating condition that can occur after a tooth extraction. It’s essential to identify the symptoms accurately to seek medical attention promptly. Accurate identification of symptoms can help distinguish them from the normal healing process, reducing the risk of complications.
Dry socket symptoms can be categorized into several key areas, including pain, swelling, bad taste, and foul odor. These symptoms can vary in duration and severity, impacting the overall healing process and daily life.
Symptoms of Dry Socket
Recognizing the symptoms of dry socket can be challenging, especially during the initial stages. A comprehensive understanding of these symptoms is crucial for timely intervention and effective management.
| Symptom | Description | Duration | Severity |
|---|---|---|---|
| Pain | Intense, throbbing, or aching sensation in the extraction site or surrounding areas | Several days to weeks | High |
| Swelling | Visible increase in gum size or swelling around the extraction site | Several days | Moderate |
| Bad Taste | Unpleasant sensation or metallic taste in the mouth, often near the extraction site | Several days | Moderate |
| Foul Odor | Noticeable bad smell from the wound site, which can be a sign of bacterial infection | Several days | Moderate |
Each symptom can manifest differently, and their duration and severity can vary depending on the individual and the severity of the dry socket. Recognizing these symptoms and understanding their characteristics can help you identify potential dry socket cases and take prompt action to alleviate symptoms and promote healing.
Stages of Dry Socket Healing and Timeline
The recovery process from a dry socket can be a long and challenging journey, but understanding the different stages involved can help patients and healthcare providers manage expectations and tailor treatment plans accordingly. A healthy bone healing process typically takes around 3-6 months, with each stage marked by distinct milestones in the healing process.
Stage 1: Initial Pain and Swelling (1-3 days)
During the initial stages of dry socket recovery, patients may experience severe pain and swelling in the affected area. This pain can be so intense that it radiates to other parts of the face and head, making it difficult to manage daily activities. In most cases, the pain peaks within the first 48 hours after surgery and gradually subsides as the healing process progresses.
Stage 2: Dry Socket Formation (4-7 days)
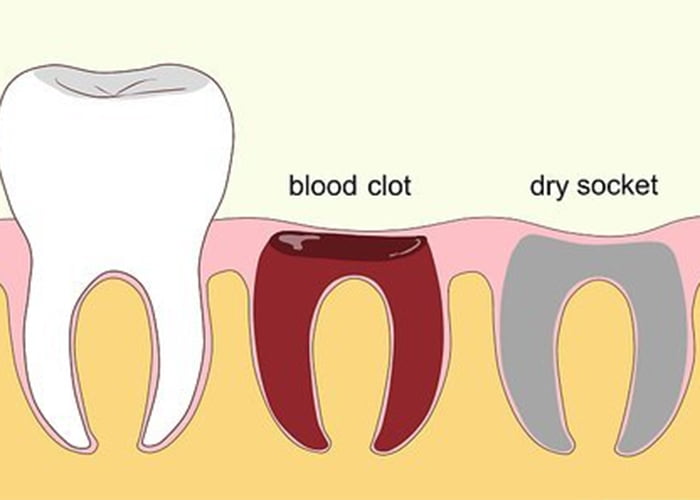
Dry socket formation is a crucial stage in the healing process, where the bone and soft tissue surrounding the affected area start to disintegrate. During this time, the bone becomes exposed, leading to increased pain and discomfort. The dry socket area may appear dry and grayish, and the surrounding tissues may be red and inflamed.
Stage 3: Wound Debridement (8-14 days)
As the dry socket starts to heal, the body begins to clean out the dead tissue and debris from the affected area. This process, known as wound debridement, can be painful and may require additional medication to manage the discomfort. Patients may also be advised to maintain good oral hygiene by rinsing with saline solution to prevent further complications.
Stage 4: Granulation Tissue Formation (15-28 days)
During this stage, the body starts to form new tissue and blood vessels in the affected area, replacing the dead tissue and promoting healthy bone growth. Granulation tissue is a critical part of the healing process, as it provides a foundation for further tissue repair and regeneration. Patients may experience increased bleeding or spotting during this stage as the new tissue forms.
Stage 5: New Tissue Formation (29-42 days)
As the granulation tissue continues to mature, new tissue begins to form, gradually covering the exposed bone. This new tissue is essential for restoring the normal anatomy of the affected area and enabling patients to experience relief from pain and discomfort.
Stage 6: Soft Tissue Closure (43-56 days)
The soft tissue closure stage is a critical milestone in the healing process, where the body completes the formation of new tissue and blood vessels, allowing the affected area to heal completely. Patients may still experience some mild pain or discomfort during this stage, but it is generally much more manageable than during the initial stages of recovery.
Stage 7: Wound Contraction (57-70 days), How long does it take for dry socket to heal
Wound contraction is the final stage of the healing process, where the affected area begins to shrink and tighten, promoting further tissue repair and regeneration. This stage is essential for restoring the normal function and appearance of the affected area.
Stage 8: Complete Healing (71-90 days)
The final stage of dry socket recovery is complete healing, where the affected area has fully recovered and patients can resume their normal daily activities without any significant discomfort or pain. This stage typically occurs between 3-4 months after surgery and is characterized by complete bone and tissue regeneration, as well as the restoration of normal oral function.
- The entire recovery process can take up to 3-6 months or longer, depending on the complexity of the surgery and individual patient factors.
- During the initial stages of recovery, patients may experience severe pain, swelling, and discomfort, but this gradually subsides as the healing process progresses.
- Good oral hygiene practices, such as rinsing with saline solution and maintaining a healthy diet, are essential for promoting recovery and preventing further complications.
- Patients may require additional medication to manage pain and discomfort during the recovery process, but they should always follow the recommended dosage and consult their healthcare provider before making any changes to their treatment plan.
In summary, the recovery process from a dry socket involves several distinct stages, each with its unique milestones and challenges. By understanding the different stages involved, patients and healthcare providers can work together to tailor treatment plans and manage expectations, ultimately promoting a smoother and more successful recovery outcome.
Risk Factors and Contraindications for Dry Socket Formation: How Long Does It Take For Dry Socket To Heal
Dry socket is a complication that can arise after tooth extraction, affecting millions of people worldwide. However, the exact causes and risk factors associated with dry socket formation are still not fully understood. Researchers have identified several factors that increase the likelihood of developing dry socket. Maintaining proper oral hygiene and avoiding certain habits and medications can significantly reduce the risk.
Impact of Oral Hygiene Practices
Proper oral hygiene practices are crucial in preventing dry socket. A study published in the Journal of Oral and Maxillofacial Surgery found that poor oral hygiene was a significant risk factor for dry socket development.
Regular brushing, flossing, and rinsing with antibacterial mouthwash can help reduce the risk of dry socket by removing bacteria and debris from the extraction site.
Failure to follow a standard oral hygiene routine can lead to the accumulation of bacteria and food particles in the extraction site, increasing the likelihood of dry socket development.
Smoking and Dry Socket
Smoking is another significant risk factor for dry socket development. The chemicals present in tobacco smoke can damage the blood vessels and reduce blood flow to the extraction site, making it more susceptible to dry socket. According to the American Dental Association, smokers are 10 times more likely to develop dry socket compared to non-smokers. The exact mechanism of how smoking causes dry socket is not fully understood, but researchers believe that the chemicals present in tobacco smoke interfere with the healing process. Quitting smoking significantly reduces the risk of developing dry socket, making it an essential step in preventing complications after tooth extraction.
Medications and Dry Socket
Certain medications, such as steroids and nonsteroidal anti-inflammatory drugs (NSAIDs), can increase the risk of dry socket development. Steroids can suppress the immune system, making it more difficult for the body to heal after tooth extraction. NSAIDs, on the other hand, can reduce blood flow to the extraction site, making it more susceptible to dry socket. Research has shown that patients who use NSAIDs after tooth extraction are more likely to develop dry socket compared to those who do not use these medications. Patients taking steroids or NSAIDs should inform their dentist before undergoing tooth extraction and follow their instructions to minimize the risk of dry socket.
Prevention and Treatment Options for Dry Socket

Preventing dry socket is a crucial aspect of ensuring a smooth recovery after dental extractions. Effective pain management plays a significant role in reducing the risk of dry socket. By implementing proper post-extraction care and choosing the right medications, patients can significantly minimize their risk of developing dry socket.
Medications for Pain Management
Pain management is an essential aspect of preventing dry socket. Non-steroidal anti-inflammatory drugs (NSAIDs) and prescription painkillers are commonly used medications to control post-extraction pain. These medications help reduce swelling and discomfort around the extraction site, which can lower the risk of dry socket.
NSAIDs, such as ibuprofen and naproxen, are effective in reducing pain and inflammation. They work by blocking the production of prostaglandins, which are chemicals responsible for pain and inflammation. For patients who experience severe pain or discomfort, prescription painkillers may be prescribed. These medications, such as narcotic analgesics, provide quick relief from pain and discomfort but should be used with caution, as they can have side effects.
Platelet-Rich Plasma (PRP) Therapy
Platelet-rich plasma (PRP) therapy has gained popularity in dental care for its ability to promote wound healing and reduce the risk of dry socket. This non-surgical treatment involves injecting platelet-rich plasma into the extraction site. PRP is obtained from the patient’s own blood and is rich in growth factors that stimulate healing.
PRP therapy helps to accelerate the healing process by increasing blood flow to the affected area. This leads to faster granulation tissue formation and faster re-epithelialization, which can reduce the risk of dry socket. Additionally, PRP therapy has anti-inflammatory properties that can help reduce swelling and pain around the extraction site.
Emerging Treatments for Dry Socket
Several emerging treatments have shown promise in promoting wound healing and reducing the risk of dry socket. One such treatment is the use of growth factors, such as platelet-derived growth factor-BB (PDGF-BB) and fibroblast growth factor-2 (FGF-2). These growth factors have been shown to promote wound healing by stimulating cell proliferation and differentiation.
Another emerging treatment is the use of nanofibers, which are ultra-fine fibers that can be used to create a scaffold for tissue regeneration. Nanofibers can be used to deliver growth factors and antibiotics to the extraction site, promoting wound healing and reducing the risk of dry socket.
End of Discussion
Healing from dry socket is a journey that requires patience, persistence, and the right approach. By understanding the stages of dry socket healing and timeline, patients can develop a clear plan of action to manage their symptoms and promote quick recovery. With proper care and attention, dry socket can be effectively managed, allowing patients to return to their normal oral health in a relatively short period.
Clarifying Questions
Can dry socket be prevented?
Yes, dry socket can be prevented by following proper oral hygiene practices, avoiding smoking, and using medications as directed. Effective post-extraction pain management is also crucial in preventing dry socket from developing.
How long does it take for dry socket to heal completely?
The complete healing of dry socket can take anywhere from 71 to 90 days, with the average healing time being around 3-6 months. However, this timeframe can vary depending on individual factors and the effectiveness of treatment.
Can dry socket recur after treatment?
Yes, dry socket can recur after treatment if underlying factors such as smoking, poor oral hygiene, and medication use are not addressed. Recurrence can also occur if treatment is not effective in addressing the root cause of dry socket.