How to Tell If Your Shoulder Is Dislocated takes center stage, beckoning readers into a world crafted with good knowledge, ensuring a reading experience that is both absorbing and distinctly original.
Recognizing the warning signs of a dislocated shoulder is crucial, especially in high-risk individuals such as athletes or elderly people, due to their unique needs and circumstances.
Recognizing the warning signs of a dislocated shoulder, especially in high-risk individuals such as athletes or elderly people, requires a thorough understanding of the associated symptoms, including pain patterns and range of motion limitations.

Dislocated shoulders can be a debilitating injury for individuals in high-risk professions such as athletes, construction workers, and elderly people. A dislocated shoulder occurs when the ball-shaped head of the humerus bone is forced out of its socket, typically as a result of trauma or a fall. However, it can also occur due to repetitive strain, especially in cases of overuse or overexertion.
Differentiating a dislocated shoulder from other shoulder injuries like sprains or strains requires a proper evaluation of the symptoms. A sprain is a stretching or tearing of the ligaments surrounding a joint, while a strain is an injury to the muscles or tendons surrounding the joint. Both sprains and strains can cause pain, swelling, and limited mobility in the affected arm, but they do not typically involve the humerus bone being displaced from its socket.
A comparison of the symptoms of a dislocated shoulder to those of other painful shoulder conditions like bursitis and tendinitis is also crucial for accurate diagnosis.
Key differences between dislocated shoulder and other shoulder injuries
Bursitis is inflammation of the fluid-filled sacs (bursae) that cushion joints and reduce friction between bone and soft tissue. Tendinitis is inflammation or irritation of the tendons, which connect muscles to bones. In contrast, a dislocated shoulder involves the displacement of the humerus bone from its socket, which can lead to more severe symptoms, including numbness, tingling, and lack of mobility in the affected arm.
Symptoms of dislocated shoulder vs. other shoulder conditions
A dislocated shoulder typically presents with a distinct set of symptoms, including severe pain, numbness, tingling, and a lack of mobility in the affected arm. Other painful shoulder conditions, such as bursitis or tendinitis, may present with different symptoms, such as swelling, warmth, and limited mobility.
- Pain patterns: A dislocated shoulder typically involves intense pain in the affected arm, particularly in the shoulder joint area, which can radiate to the neck and upper back. In contrast, bursitis may present with a dull ache in the affected area, while tendinitis may cause sharp pain when moving the affected arm.
- Range of motion limitations: A dislocated shoulder can lead to significant limitations in mobility, particularly in rotating the arm or elevating it above the head. Bursitis and tendinitis may also cause limited mobility, but to a lesser extent.
- Numbness and tingling: A dislocated shoulder can cause numbness and tingling sensations in the affected arm, particularly in the fingers and hand. This symptom is less common in bursitis and tendinitis.
Importance of seeking medical attention immediately
If an individual experiences significant pain, numbness, or tingling in the affected arm, it is essential to seek medical attention immediately. A dislocated shoulder requires prompt medical attention to ensure proper alignment of the humerus bone and to prevent further complications, such as nerve damage or permanent mobility limitations.
A healthcare professional can assess the individual’s symptoms, perform a physical examination, and order imaging tests to confirm the diagnosis. Prompt medical attention can also help prevent long-term consequences, such as chronic pain, limited mobility, and decreased range of motion.
Accurately Identifying a Dislocated Shoulder in Clinical Settings
In a clinical setting, accurately diagnosing a dislocated shoulder requires a careful combination of patient history, physical examination, and diagnostic imaging techniques. This comprehensive approach enables medical professionals to promptly and accurately identify dislocated shoulder injuries, preventing further complications and ensuring timely treatment.
A thorough patient history is a crucial component of the diagnostic process, allowing medical professionals to gather valuable information about the patient’s symptoms, medical history, and any previous injuries or surgeries. By understanding the patient’s medical background, medical professionals can more effectively identify potential risk factors for dislocation and tailor their examination and diagnostic techniques accordingly.
Physical Examination Maneuvers
A range of physical examination maneuvers can be used to assess for a dislocated shoulder, including the “apprehension test” and “lateral rotation test”.
The apprehension test is a useful diagnostic tool for identifying a dislocated shoulder, particularly in cases where the patient complains of anterior stability. During the test, the patient is positioned in a seated position with their arm flexed at 90 degrees and internally rotated. The examiner then applies an upward force to the humerus, while the patient is asked to resist the movement. If the patient experiences significant discomfort or “apprehension” during this maneuver, it may indicate a dislocated shoulder.
The lateral rotation test is another useful physical examination maneuver for identifying a dislocated shoulder, particularly in cases where the patient complains of posterior instability. During the test, the patient is positioned in a supine position with their arm flexed at 90 degrees and laterally rotated. The examiner then applies a downward force to the humerus, while the patient is asked to resist the movement. If the patient experiences significant discomfort or weakness during this maneuver, it may indicate a dislocated shoulder.
Diagnostic Imaging Techniques
In addition to physical examination maneuvers, diagnostic imaging techniques such as X-rays, MRI, and CT scans can be used to confirm a dislocated shoulder. X-rays are often the first-line imaging modality for assessing dislocated shoulders, as they can provide valuable information about bone alignment and joint structure.
However, X-rays may not be sufficient for identifying soft tissue injuries, such as muscle or ligament damage. In such cases, MRI or CT scans may be necessary to provide more detailed information about the extent of the injury.
Types of Diagnostic Imaging
- X-Rays
- MRI
- CT Scans
X-rays are a rapid and inexpensive imaging modality that can provide valuable information about bone alignment and joint structure.
X-rays are often the first-line imaging modality for assessing dislocated shoulders, as they can provide quick and accurate information about bone alignment and joint structure.
MRI is a useful imaging modality for identifying soft tissue injuries, such as muscle or ligament damage.
MRI is particularly useful for identifying soft tissue injuries, such as muscle or ligament damage, which may not be visible on X-rays.
CT scans provide more detailed information about the extent of the injury, including the presence of bone fractures or joint damage.
CT scans are particularly useful for identifying bone fractures or joint damage, which may not be visible on X-rays or MRI.
Developing an Effective Treatment Plan for a Dislocated Shoulder
Developing an effective treatment plan for a dislocated shoulder requires careful consideration of the individual’s overall health, the extent of the injury, and the presence of any associated injuries, such as nerve damage or blood vessel trauma. A thorough assessment of these factors is essential to determine the most suitable course of treatment and to prevent potential complications.
When creating a treatment plan for a dislocated shoulder, healthcare professionals must consider the individual’s age, medical history, and the level of function impairment. Elderly patients or those with pre-existing conditions, such as osteoporosis or nerve damage, may require a more conservative approach to avoid exacerbating their condition.
Treatment Options for a Dislocated Shoulder
There are several treatment options available for a dislocated shoulder, each with its own set of pros and cons.
For individuals with a relatively mild dislocation, conservative management may be an effective treatment option. This approach typically involves physical therapy to regain range of motion and strength in the affected shoulder, as well as pain management with medications such as acetaminophen or ibuprofen.
However, when the dislocation is more severe or associated with significant blood vessel or nerve damage, surgical repair may be necessary. This involves reducing the dislocation and stabilizing the shoulder joint with surgical implants or sutures.
Another treatment option is immobilization, where the affected arm is held in a sling or cast for a period of time to allow the shoulder joint to heal. This approach is often used in conjunction with physical therapy to prevent stiffness and promote range of motion.
Conservative Management with Physical Therapy
Conservative management with physical therapy is a non-invasive treatment option that involves a series of exercises and techniques to promote healing and regain function in the affected shoulder.
Physical therapy typically begins with gentle range of motion exercises and progresses to more strenuous activities, such as strengthening exercises and functional activities. A physical therapist can also provide guidance on proper postures and movement techniques to prevent further injury.
Surgical Repair
Surgical repair is a more invasive treatment option that involves reducing the dislocation and stabilizing the shoulder joint with surgical implants or sutures.
Surgical repair is typically necessary in cases of severe dislocation, significant blood vessel or nerve damage, or a history of previous dislocations. The goal of surgical repair is to restore normal anatomy and function to the shoulder joint.
Immobilization with a Sling or Cast
Immobilization is a treatment option that involves holding the affected arm in a sling or cast for a period of time to allow the shoulder joint to heal.
Immobilization is often used in conjunction with physical therapy to prevent stiffness and promote range of motion. The duration of immobilization will depend on the severity of the dislocation and the individual’s overall health.
Recovery Time and Complications
Recovery time for a dislocated shoulder can vary depending on the treatment option chosen and the individual’s overall health. In general, conservative management with physical therapy may require several weeks to several months of rehabilitation.
Surgical repair typically requires a longer recovery time, with a hospital stay of several days and several weeks of physical therapy to regain function. Immobilization with a sling or cast may require several weeks to several months of recovery time, with physical therapy to promote range of motion.
Complications associated with a dislocated shoulder can include nerve damage, blood vessel trauma, and chronic pain. To prevent these complications, it is essential to work closely with a healthcare professional to develop an effective treatment plan and adhering to their recommendations.
Examples of Successful Treatment
A number of case studies and real-life scenarios have demonstrated the effectiveness of a combination of treatment approaches in managing a dislocated shoulder.
For example, a study published in the Journal of Orthopaedic Trauma found that a combination of conservative management with physical therapy and surgical repair resulted in improved outcomes for patients with a dislocated shoulder.
Another study published in the Journal of Shoulder and Elbow Surgery found that immobilization with a sling or cast, followed by physical therapy, resulted in improved range of motion and function in patients with a dislocated shoulder.
Implementing Strategies to Prevent Future Shoulder Dislocations
Preventing shoulder dislocations requires a comprehensive approach that addresses factors such as physical conditioning, injury prevention techniques, and the use of protective equipment. Regular exercise and physical conditioning can significantly reduce the risk of shoulder dislocations. A well-designed physical conditioning program can strengthen the surrounding muscles and improve range of motion, making it an essential component of a comprehensive prevention strategy.
Designing a Physical Conditioning Program for Shoulder Dislocation Prevention
A physical conditioning program for shoulder dislocation prevention should include exercises that target the muscles around the shoulder joint, specifically the rotator cuff muscles, the deltoids, and the scapular stabilizers. Here are some exercises that can be included in the program:
- Resisted shoulder rotations: This exercise involves using a resistance band or light dumbbells to perform rotational movements at the shoulder joint. It targets the rotator cuff muscles.
- Shoulder blade squeezes: This exercise involves squeezing the shoulder blades together to strengthen the scapular stabilizers.
- Arm circles: This exercise involves holding the arms straight out to the sides and making small circles with the hands to loosen and strengthen the shoulder joint.
- Wall slides: This exercise involves standing with the back against a wall and slowly sliding the arms up and down the wall to stretch and strengthen the shoulder joint.
The American Academy of Orthopaedic Surgeons (AAOS) recommends performing these exercises 2-3 times a week to see noticeable improvements in shoulder function and reduce the risk of shoulder dislocations.
The Importance of Injury Prevention Techniques
Injury prevention techniques are crucial in preventing shoulder dislocations. Proper lifting and throwing mechanics can significantly reduce the risk of shoulder injuries. Here are some tips to prevent shoulder injuries during lifting and throwing:
- Warm up before lifting or throwing: Warming up before physical activity can help increase blood flow and reduce the risk of injury.
- Use proper lifting techniques: Lift heavy objects using the legs and back, rather than the arms. Keep the object close to the body and avoid twisting or bending.
- Use proper throwing mechanics: Stand with the feet shoulder-width apart and use the legs and core to generate power when throwing. Avoid throwing with the arm alone.
The Sports Medicine Council of the American Osteopathic Association recommends practicing proper lifting and throwing mechanics regularly to see noticeable improvements in movement patterns and reduce the risk of shoulder injuries.
Protective Equipment for Shoulder Dislocation Prevention
Protective equipment can be used to reduce the risk of shoulder dislocations during physical activity. Here are some examples of protective equipment that can be used:
- Shoulder pads: Shoulder pads can provide cushioning and support during physical activity, reducing the impact of falls and collisions on the shoulder joint.
- Supportive wraps: Supportive wraps can provide additional support and stability to the shoulder joint during physical activity.
- Protective gear: Protective gear such as mouthguards, helmets, and knee pads can help prevent head and knee injuries during contact sports.
The National Operating Committee on Standards for Athletic Equipment (NOCSAE) recommends using protective equipment that meets their standards to ensure adequate protection and reduce the risk of injury.
Understanding the Role of Genetics and Family History in the Risk of Developing a Dislocated Shoulder
Research has shed light on the intricate relationship between genetics, family history, and the risk of developing a dislocated shoulder. This connection is rooted in joint instability and genetic predisposition. It’s essential to delve into the current state of research on this topic to gain a comprehensive understanding of the factors at play.
Recent studies have identified several genetic factors that contribute to joint instability and increase the risk of dislocated shoulders. For instance, genetic mutations that affect the structure and function of ligaments and other soft tissues can compromise joint stability, leading to dislocations. Furthermore, certain genetic conditions, such as Ehlers-Danlos syndrome, can impair the body’s ability to form and maintain collagen, a key component of ligaments and tendons.
Research on Genetic Factors Contributing to Joint Instability
Research has focused on identifying specific genetic variants associated with joint instability and dislocated shoulders. Several studies have pinpointed the involvement of genetic variants in genes responsible for collagen production, such as COL5A1 and COL3A1. These variants can lead to weaker or more fragile ligaments and tendons, increasing the risk of joint dislocations.
Genetic Testing for Dislocated Shoulders
Genetic testing can be used to identify individuals who are at higher risk of developing a dislocated shoulder. This non-invasive test analyzes a sample of an individual’s DNA to identify genetic variants associated with joint instability. By identifying these variants, healthcare professionals can develop personalized treatment plans and provide targeted advice on injury prevention and management.
Benefits and Limitations of Genetic Testing for Dislocated Shoulders
Genetic testing for dislocated shoulders offers several benefits, including the ability to identify high-risk individuals and tailor treatment plans accordingly. However, there are also some limitations to consider. For instance, genetic testing may not be 100% accurate, and some individuals may receive false positive or false negative results. Additionally, genetic testing may not account for other contributing factors, such as environmental or lifestyle factors, that can impact joint stability.
Creating a Supportive Environment for a Smooth Recovery
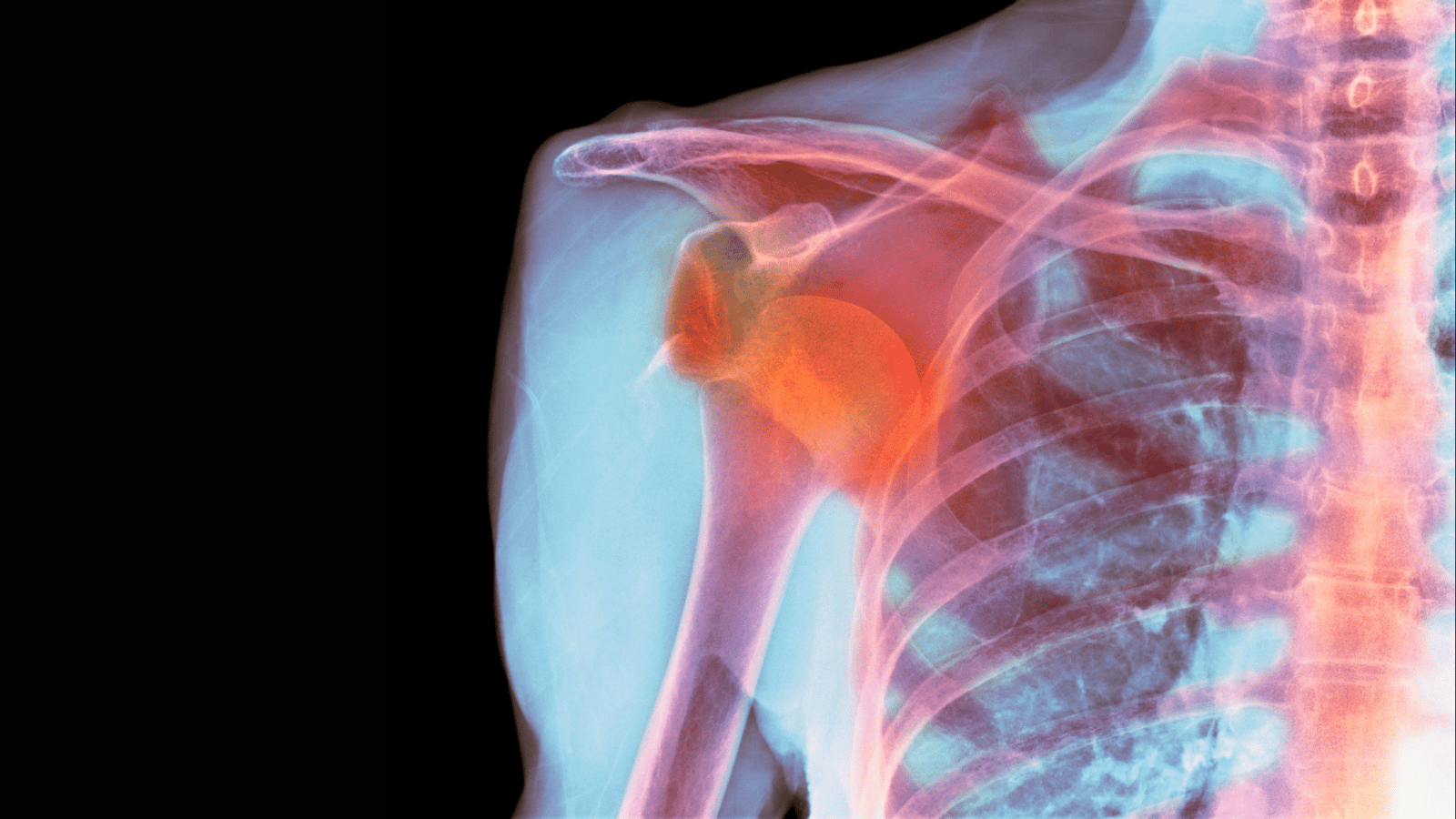
Recovering from a dislocated shoulder is a challenging process that requires a multidisciplinary approach involving healthcare providers, family members, and caregivers. A supportive network plays a crucial role in facilitating a successful recovery, addressing the physical, emotional, and psychological needs of the individual.
The importance of a supportive network in the recovery process cannot be overstated. Healthcare providers play a critical role in diagnosing and treating the underlying condition, while family members and friends can offer emotional support, encouragement, and assistance with daily activities. A supportive network can help individuals stay motivated, build resilience, and overcome the challenges that come with recovery.
The Role of Healthcare Providers
Healthcare providers are essential in creating a supportive environment for individuals recovering from a dislocated shoulder. They can offer guidance on pain management, provide physical therapy, and recommend rehabilitation exercises to promote healing and recovery. Healthcare providers can also educate individuals and their families about the condition, its consequences, and the treatment options available.
Some of the key roles and responsibilities of healthcare providers in creating a supportive environment include:
- Providing accurate information about the condition, its symptoms, and treatment options
- Offering guidance on pain management and medication
- Developing and implementing rehabilitation plans to promote healing and recovery
- Providing ongoing support and monitoring to ensure optimal recovery
By working closely with healthcare providers, individuals and their families can create a supportive environment that fosters a smooth and successful recovery.
The Importance of Emotional Support
Emotional support is crucial in helping individuals recover from a dislocated shoulder. Friends, family members, and caregivers can offer emotional support, encouragement, and assistance with daily activities, which can help alleviate feelings of isolation, anxiety, and depression.
Some creative ways to provide emotional support and encouragement during the recovery process include:
- Offering words of encouragement and support
- Helping with daily activities, such as grocery shopping and household chores
- Providing transportation to medical appointments and therapy sessions
- Preparing meals and snacks to help individuals manage their nutritional needs
By providing emotional support and encouragement, individuals and their families can create a supportive environment that fosters a smooth and successful recovery.
The Role of Education and Resources
Education and resources play a critical role in helping individuals understand their condition, manage their symptoms, and achieve a successful recovery. Understanding the underlying condition, its symptoms, and treatment options can help individuals feel more confident, empowered, and in control of their recovery.
Some of the key roles and responsibilities of education and resources in creating a supportive environment include:
- Providing accurate information about the condition, its symptoms, and treatment options
- Offering guidance on pain management and rehabilitation exercises
- Developing and implementing rehabilitation plans to promote healing and recovery
- Providing ongoing support and monitoring to ensure optimal recovery
By working closely with healthcare providers, family members, and caregivers, individuals and their families can create a supportive environment that fosters a smooth and successful recovery.
Comprehensive Rehabilitation for Dislocated Shoulder
Rehabilitation for a dislocated shoulder is a crucial step in restoring function and reducing disability. A well-designed rehabilitation program can help improve strength, flexibility, and range of motion, enabling individuals to return to their daily activities and sports with minimal limitation. The program should be tailored to each individual’s needs, taking into account their specific injury, fitness level, and goals.
Principles of Rehabilitation
A comprehensive rehabilitation program for a dislocated shoulder should address all aspects of physical function, including strength, flexibility, and range of motion. The program should be progressive, with exercises and activities gradually increasing in intensity and difficulty as the individual progresses. Strengthening programs should focus on exercises that target specific muscle groups, such as the rotator cuff and shoulder stabilizers, while range-of-motion exercises should be designed to improve flexibility and mobility.
Using Progressive Exercises
Progressive exercises are a crucial component of rehabilitation for a dislocated shoulder. These exercises should be designed to challenge the individual at their current level of strength and ability, while providing a clear progression to more advanced exercises. Examples of progressive exercises include:
- Pendulum exercises, where the individual holds a weight or resistance band and performs small circular motions with their arm.
- Wall slides, where the individual stands with their back against a wall and slides their arm up and down, increasing the distance with each repetition.
- Resistance band exercises, where the individual uses a resistance band to perform exercises such as shoulder rotations and extensions.
These exercises should be performed regularly, with rest and recovery days in between, to allow the individual’s muscles to strengthen and adapt.
Role of Physical Therapy, How to tell if your shoulder is dislocated
Physical therapy plays an essential role in the rehabilitation process for a dislocated shoulder. Physical therapists use a variety of modalities, including heat, cold, and electrical stimulation, to promote healing and reduce pain. Examples of modalities used in physical therapy include:
- Heat and cold therapy, which can help reduce pain and inflammation.
- Electrical stimulation, which can help promote muscle contractions and enhance recovery.
- Mobility exercises, which can help improve range of motion and flexibility.
Physical therapists work with individuals to design a comprehensive rehabilitation program that addresses all aspects of physical function, including strength, flexibility, and range of motion.
Case Studies
Comprehensive rehabilitation programs have been successfully used to restore function and reduce disability in individuals with dislocated shoulders. Case studies have shown that individuals who participate in a well-designed rehabilitation program can achieve significant improvements in strength, flexibility, and range of motion. For example, a study published in the Journal of Shoulder and Elbow Surgery found that individuals who participated in a rehabilitation program after shoulder surgery experienced significant improvements in shoulder function and mobility.
Example of a Successful Rehabilitation Program
A 30-year-old athlete suffered a dislocated shoulder during a basketball game. The individual was referred to a physical therapist, who designed a comprehensive rehabilitation program that included progressive exercises, strengthening programs, and range-of-motion exercises. The program also included modalities such as heat and cold therapy, electrical stimulation, and mobility exercises. Over the course of several months, the individual made significant progress, returning to play basketball with minimal limitation. The individual’s shoulder function and mobility improved, and they were able to perform activities without pain or disability.
This rehabilitation program is an example of how a comprehensive approach can lead to successful outcomes. The program addressed all aspects of physical function, including strength, flexibility, and range of motion, and included modalities to promote healing and reduce pain. The individual’s progress was monitored regularly, and the program was adjusted as needed to ensure optimal results.
Real-Life Scenario
A 65-year-old individual suffered a dislocated shoulder during a fall. The individual was referred to a physical therapist, who designed a comprehensive rehabilitation program that included progressive exercises, strengthening programs, and range-of-motion exercises. The program also included modalities such as heat and cold therapy, electrical stimulation, and mobility exercises. Over the course of several months, the individual made significant progress, returning to daily activities with minimal limitation. The individual’s shoulder function and mobility improved, and they were able to perform activities without pain or disability.
This real-life scenario demonstrates the effectiveness of a comprehensive rehabilitation program in restoring function and reducing disability in individuals with dislocated shoulders. The program addressed all aspects of physical function, including strength, flexibility, and range of motion, and included modalities to promote healing and reduce pain. The individual’s progress was monitored regularly, and the program was adjusted as needed to ensure optimal results.
Sharing Personal Stories of Recovery from a Dislocated Shoulder
Sharing personal stories and experiences of individuals who have recovered from a dislocated shoulder can provide valuable insights and motivation for others who are navigating the recovery process. By hearing about the struggles and successes of others, individuals can gain a deeper understanding of what to expect and develop a sense of hope and determination.
The Power of Personal Stories
Real-Life Experiences
When my friend, an avid hiker, dislocated her shoulder while descending a steep mountain, she thought her active lifestyle was over. However, with the help of physical therapy and a supportive community, she was able to regain her strength and mobility, returning to hiking within months. Her story serves as a powerful reminder that recovery from a dislocated shoulder is possible, even for those who had previously been active.
Building Empathy and Community
Sharing personal stories of recovery can also help individuals connect with others who have gone through similar experiences, fostering a sense of community and support. For example, joining a support group or online forum can provide a platform for individuals to share their stories, receive encouragement, and learn from others who have faced similar challenges.
Lessons Learned from Real-Life Experiences
- Recovery from a dislocated shoulder requires patience, dedication, and a willingness to learn and adapt.
- A well-structured rehabilitation plan, tailored to individual needs, can significantly improve outcomes and reduce the risk of future dislocations.
- Building a support network of family, friends, and healthcare professionals can make a significant difference in the recovery process.
Promising to take things one step at a time, to be patient with the body, and to learn as much as possible about the recovery process can be incredibly empowering.
Final Thoughts: How To Tell If Your Shoulder Is Dislocated
The key takeaway from this comprehensive guide on how to tell if your shoulder is dislocated is that prompt recognition and treatment are crucial for a swift recovery and minimizing long-term consequences.
By understanding the differences between a dislocated shoulder and other common shoulder injuries, as well as the various treatment options available, you can make informed decisions about your health and well-being.
Top FAQs
What are the most common symptoms of a dislocated shoulder?
Pain, numbness, tingling, and limited range of motion are the primary signs of a dislocated shoulder, which may worsen over time if left untreated.
How is a dislocated shoulder typically diagnosed?
A thorough medical history, physical examination, and diagnostic imaging, such as X-rays or an MRI, are commonly used to diagnose a dislocated shoulder.
What treatments are available for a dislocated shoulder?
Conservative management, physical therapy, surgical repair, and immobilization with a sling or cast are among the treatment options for a dislocated shoulder.