As how to get rid of gingivitis takes center stage, this opening passage beckons readers into a world where good oral hygiene habits and expert advice converge, ensuring a reading experience that is both absorbing and distinctly original.
From understanding the causes and risk factors of gingivitis to discovering the early warning signs and symptoms, this comprehensive guide will walk you through every step of the journey to a healthier smile.
Understanding the Causes and Risk Factors of Gingivitis
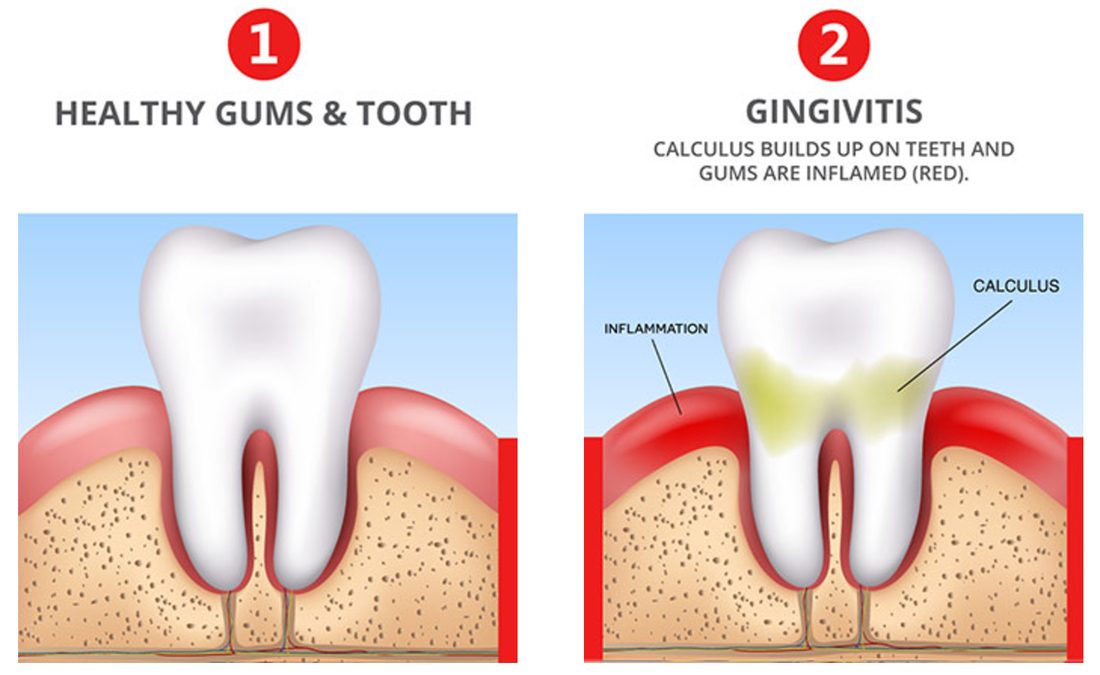
Gingivitis is a common and reversible condition where the gums become inflamed, red, and tender. Poor oral hygiene is often a contributing factor to the development of gingivitis. Regular brushing, flossing, and dental check-ups can help prevent gingivitis. Good oral hygiene practices involve removing plaque, a sticky film of bacteria that can cause gum inflammation. Brushing at least twice a day and replacing toothbrushes regularly can also help maintain healthy gums.
Poor oral hygiene habits, including infrequent brushing and flossing, are a major risk factor for gingivitis. This can lead to a buildup of plaque on the teeth and cause gum inflammation. Furthermore, if plaque is not removed, it can harden into tartar, which can make it difficult to clean the teeth properly. This can lead to gum recession, bleeding gums, and potentially even tooth loss.
Genetics and Hormonal Fluctuations
Research suggests that genetics can play a role in the development of gingivitis. Some studies have found that individuals with a family history of periodontal disease are more likely to develop gingivitis. Hormonal fluctuations during pregnancy, menstruation, or menopause can also increase the risk of developing gingivitis. Changes in hormone levels can cause an increase in blood flow to the gums, making them more susceptible to inflammation.
Additionally, the presence of certain medical conditions, such as diabetes, can also increase the risk of developing gingivitis. These conditions can cause changes in the body that make it more difficult for the immune system to fight off bacterial infections, which can lead to gum inflammation.
Medications and Gingivitis Risk
Certain medications can increase the risk of developing gingivitis. Antidepressants, for example, can cause dry mouth, which can lead to an increased risk of tooth decay and gum inflammation. Additionally, birth control pills contain hormones that can affect blood flow to the gums, making them more susceptible to inflammation.
Other medications, such as antihistamines and decongestants, can also cause dry mouth and increase the risk of gingivitis. Steroids can also cause changes in blood sugar levels, which can increase the risk of developing gingivitis.
Other Risk Factors, How to get rid of gingivitis
Tobacco use is another significant risk factor for gingivitis. Smoking and chewing tobacco can cause gum inflammation and increase the risk of gum recession. Furthermore, people with compromised immune systems, such as those with HIV/AIDS, are more susceptible to gum infections and gum disease.
Additionally, individuals who eat a diet high in sugar and acid can also increase their risk of developing gingivitis. Regular consumption of sugary and acidic foods can lead to tooth decay and gum inflammation.
Dietary Changes and Supplements for Gingivitis Prevention: How To Get Rid Of Gingivitis

Dietary changes and supplements play a significant role in the prevention and management of gingivitis. A well-balanced diet rich in essential nutrients and vitamins can help maintain oral health, reduce inflammation, and prevent the development of gingivitis. This section will discuss the importance of certain vitamins, omega-3 fatty acids, probiotics, and prebiotics in maintaining oral health and preventing gingivitis.
The Role of Vitamin Deficiency in Gingivitis Development
Vitamin deficiencies, particularly those of vitamins C and D, have been linked to an increased risk of gingivitis. Vitamin C, also known as ascorbic acid, plays a crucial role in the production of collagen, a protein that gives structure to the teeth, bones, and gums. Vitamin C is also essential for the synthesis of carnitine, a molecule that helps to transport fatty acids into the mitochondria, where they are burned for energy.
A minimum of 60 mg of vitamin C per day is recommended for adults to maintain optimal oral health.
Vitamin D, on the other hand, helps to regulate the body’s inflammatory response and has been shown to reduce the risk of gum disease.
The recommended daily intake of vitamin D is 600-800 IU for adults.
The Effects of Omega-3 Fatty Acids on Gum Inflammation
Omega-3 fatty acids, particularly EPA and DHA, have been shown to reduce inflammation and promote healing in the gums. These essential fatty acids work by reducing the production of pro-inflammatory molecules and promoting the production of anti-inflammatory molecules. Research has shown that consuming omega-3 fatty acids can significantly reduce gum inflammation and prevent the development of gingivitis.
- Sources of omega-3 fatty acids include fatty fish such as salmon, sardines, and mackerel, as well as plant-based sources such as flaxseeds and walnuts.
- Consuming omega-3 fatty acids in moderation, as part of a balanced diet, may help to reduce gum inflammation and prevent gingivitis.
- A study published in the Journal of Periodontology found that consuming 1 gram of omega-3 fatty acids per day reduced gum inflammation by 25%.
The Benefits of Probiotics and Prebiotics in Oral Health
Probiotics and prebiotics are live bacteria and yeast that are beneficial to the health of the mouth. Probiotics, such as Lactobacillus and Bifidobacterium, can help to maintain a healthy balance of the oral microbiome, reduce inflammation, and prevent the development of gingivitis. Prebiotics, such as inulin and fructooligosaccharides, work by feeding the good bacteria in the mouth, allowing them to flourish and maintain a healthy balance.
- Consuming probiotics and prebiotics may help to reduce gum inflammation and prevent gingivitis.
- Probiotics have been shown to reduce the levels of inflammatory markers in the mouth and promote the production of anti-inflammatory molecules.
- Prebiotics have been found to increase the levels of beneficial bacteria in the mouth and reduce the levels of pathogenic bacteria.
Ending Remarks
In conclusion, getting rid of gingivitis requires a multifaceted approach that combines good oral hygiene habits, dietary changes, and professional treatment options. By following the tips and advice Artikeld in this guide, you can effectively manage and prevent gingivitis, maintaining a healthy and beautiful smile for years to come.
Quick FAQs
Q: What are the main causes of gingivitis?
A: Poor oral hygiene habits, genetics, hormonal fluctuations, and certain medications such as antidepressants and birth control pills are all contributing factors to the development of gingivitis.
Q: Can gingivitis be prevented?
A: Yes, by practicing good oral hygiene habits, such as brushing and flossing regularly, and visiting your dentist for regular check-ups, you can significantly reduce your risk of developing gingivitis.
Q: What are the symptoms of gingivitis?
A: Common symptoms include swollen gums, redness, bleeding during brushing, sensitivity to hot and cold temperatures, and bad breath.
Q: What are the treatment options for gingivitis?
A: Treatment options may include scaling and root planing, laser treatments, and antimicrobial mouthwashes, depending on the severity of the condition.
Q: Can gingivitis be cured?
A: Yes, in most cases, gingivitis can be cured with proper treatment and care. However, recurrent cases may require ongoing maintenance and monitoring.