With how long does it take for dental implants to heal at the forefront, this journey opens a window to an in-depth exploration of the complexities involved in the process. From the initial healing process to osseointegration duration and bone regeneration, every step plays a crucial role in the successful integration of dental implants.
The speed of recovery time varies depending on several factors, including age, health status, and smoking habits. The role of blood flow and oxygenation in the initial healing process cannot be overstated, with proper placement and angulation of dental implants being equally important. Osseointegration duration and its importance in dental implant integration cannot be ignored, with different bone types and their osseointegration durations varying significantly.
Dental Implants Healing Process and Factors Influencing Recovery Time
The initial healing process of dental implants involves several complex biological and biochemical events. This process is crucial for the successful integration of dental implants into the human body. The healing process can be influenced by various factors, including age, overall health status, smoking habits, and proper placement and angulation of dental implants.
Role of Blood Flow and Oxygenation in Initial Healing Process
Blood flow and oxygenation play a vital role in the initial healing process of dental implants. The presence of oxygen is essential for the formation of new bone tissue, which is necessary for the integration of dental implants. During the healing process, the body relies on blood flow to deliver oxygen and nutrients to the implant site. Blood flow also helps to remove waste products and dead cells from the implant site, promoting a healthy environment for healing. Without adequate blood flow and oxygenation, the healing process may be delayed or compromised, leading to implant failure.
Factors Affecting Healing Time
Several factors can influence the healing time of dental implants, including age, overall health status, and smoking habits. Older patients may experience a slower healing process due to decreased bone density and reduced blood flow. Patients with certain medical conditions, such as diabetes or cardiovascular disease, may also experience delayed healing due to compromised blood flow and oxygenation. Smoking habits can also negatively impact healing time by reducing blood flow and oxygenation to the implant site.
Age-related factors can significantly influence the healing time of dental implants. Older patients may experience a slower healing process due to:
- Decreased bone density, which can affect the stability of dental implants
- Reduced blood flow, which can compromise oxygenation and nutrient delivery to the implant site
- Increased risk of infections and other complications, which can delay healing
Smoking habits can also negatively impact healing time by reducing blood flow and oxygenation to the implant site:
- Smoking can lead to a decrease in blood flow to the implant site, compromising oxygenation and nutrient delivery
- Smoking can also lead to a decrease in the production of collagen, a protein essential for wound healing
- Smoking can increase the risk of infections and other complications, which can delay healing
Proper placement and angulation of dental implants are also crucial for the healing process. Dental implants that are placed too shallow or too deep can experience reduced stability and increased risk of failure. Dental implants that are angled incorrectly can also compromise the surrounding bone tissue, affecting the healing process.
Importance of Proper Placement and Angulation of Dental Implants, How long does it take for dental implants to heal
Proper placement and angulation of dental implants are critical for the successful integration of dental implants into the human body. Dental implants that are placed too shallow or too deep can experience reduced stability and increased risk of failure. Dental implants that are angled incorrectly can also compromise the surrounding bone tissue, affecting the healing process.
The importance of proper placement and angulation can be seen in the following:
- Poor placement can lead to reduced stability, which can affect the healing process and increase the risk of implant failure
- Poor angulation can compromise the surrounding bone tissue, affecting the healing process and increasing the risk of implant failure
- Proper placement and angulation can ensure that dental implants are integrated into the surrounding bone tissue, promoting a healthy environment for healing
Osseointegration Duration and its Importance: How Long Does It Take For Dental Implants To Heal
Osseointegration is the process by which dental implants integrate with the surrounding bone, enabling secure attachment and stability of the implant. This biological and mechanical bond between the bone and the implant is crucial for the long-term success of dental implants. The osseointegration duration, typically ranging from several weeks to several months, varies depending on individual factors, including bone type, implant design, and patient health.
Different Bone Types and Their Osseointegration Durations
Bone type plays a significant role in determining the osseointegration duration. Different bone types have varying levels of osteoconductivity, osteoinductivity, and bone density, which influence the rate of integration.
- Dense Cortical Bone: Osseointegration occurs rapidly in dense cortical bone, typically within 2-4 months. Cortical bone is known for its high density and structural integrity, providing a stable foundation for implant placement.
- cancellous Bone: Osseointegration in cancellous bone, characterized by its porous and spongy structure, is slower than in cortical bone, typically taking 4-6 months. However, cancellous bone’s high surface area and potential for osteogenesis compensate for its slower integration rate.
- Poorly Mineralized Bone: Bone with low mineral content, often due to osteoporosis or other metabolic disorders, exhibits delayed osseointegration, typically requiring 6-9 months or more. In such cases, additional measures like bone grafting may be necessary to enhance bone density.
Proper osseointegration can be achieved through optimal implant placement, loading protocols, and bone grafting, ensuring a stable and successful integration process.
- Loading Protocols: The force applied to the implant during functional loading can significantly impact osseointegration. Proper loading protocols, such as controlled mastication and avoidance of excessive forces, help maintain the bone-implant interface without compromising integration.
- Bone Grafting: Bone grafting involves using graft materials to enhance the bone density and promote osteogenesis. This can be particularly useful in cases of insufficient bone density, poorly mineralized bone, or when implants are positioned in areas with limited bone availability.
CONSEQUENCES OF DELAYED OR INSUFFICIENT OSSEOINTEGRATION
Delayed or insufficient osseointegration can lead to implant instability, affecting the entire restorative process and reducing the lifespan of the implant.
- Implant Instability: Insufficient osseointegration may result in implant movement, which can lead to micromotion and bone resorption around the implant site. This instability jeopardizes the success of the implant, necessitating corrective measures or even implant removal.
- Peri-Implantitis: Prolonged implant instability can lead to peri-implantitis, characterized by inflammation and bone loss. This can compromise the implant’s longevity and necessitate costly and time-consuming treatments.
Osseointegration is a dynamic process, influenced by a combination of biological, mechanical, and physiological factors. Understanding these factors is crucial for optimizing osseointegration and ensuring the long-term success of dental implants.
Bone Regeneration and Dental Implant Healing Describe the process of bone regeneration and its role in dental implant healing
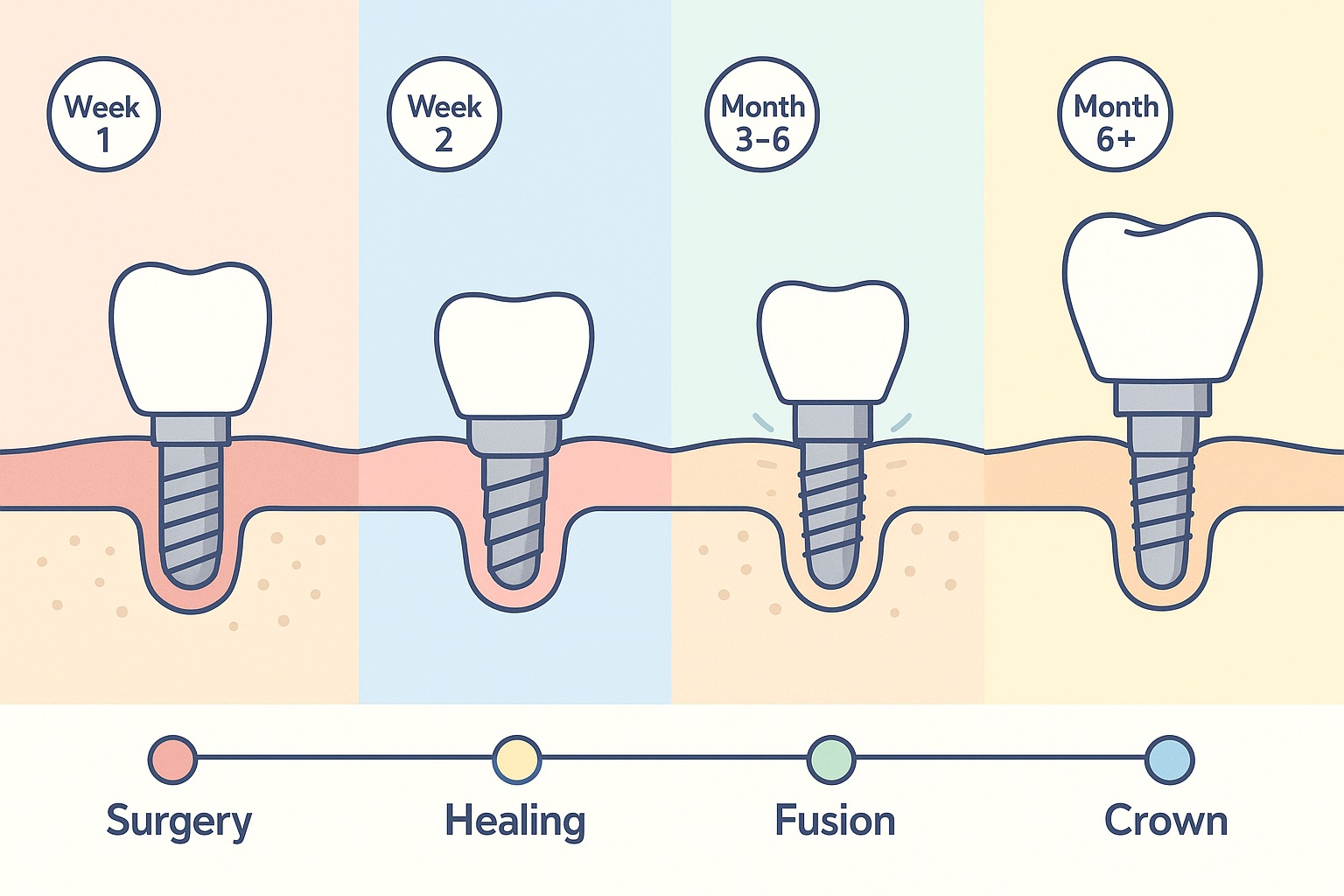
Bone regeneration plays a crucial role in dental implant healing, ensuring a stable and secure foundation for the implant. This process is essential for the success of dental implants, as it enables the growth of new bone tissue around the implant, promoting integration and stability. In this section, we will delve into the process of bone regeneration, its role in dental implant healing, and explore the role of stem cells and growth factors in this process.
Bone regeneration involves the activation of various cellular processes that lead to the formation of new bone tissue. This process can be influenced by several factors, including the presence of stem cells, growth factors, and the overall health of the individual. In the context of dental implants, bone regeneration is critical for ensuring a stable and durable implant.
The Role of Stem Cells in Bone Regeneration
Stem cells are undifferentiated cells that have the ability to differentiate into various cell types, including those needed for bone regeneration. In the context of dental implant healing, stem cells play a crucial role in the activation of bone regeneration processes. These cells can be derived from various sources, including bone marrow, adipose tissue, and peripheral blood. Research has shown that the use of stem cells can enhance bone regeneration, promoting faster and more stable implant integration.
The Role of Growth Factors in Bone Regeneration
Growth factors are signaling molecules that play a crucial role in the regulation of cellular processes, including bone regeneration. In the context of dental implant healing, growth factors can stimulate the growth and differentiation of osteoblasts, leading to the formation of new bone tissue. Growth factors such as BMP-2 (Bone Morphogenetic Protein-2) and VEGF (Vascular Endothelial Growth Factor) have been shown to promote bone regeneration, enhancing implant integration and stability.
Case Studies: Bone Regeneration for Improved Denture Stability
Bone regeneration has been used to improve denture stability in individuals with severe bone loss. In one study, researchers used a combination of stem cells and growth factors to promote bone regeneration in individuals with severe mandibular bone loss. The results showed significant improvements in denture stability, quality of life, and overall satisfaction.
Comparison of Different Bone Regeneration Techniques
Several techniques have been developed to promote bone regeneration in dental implant healing. These include the use of stem cells, growth factors, and bone grafting materials. While each technique has its own advantages and disadvantages, research has shown that a combination of these techniques can enhance implant integration and stability.
Table: Comparison of Different Bone Regeneration Techniques
| Technique | Advantages | Disadvantages |
|---|---|---|
| Stem Cell-Based Bone Regeneration | Enhanced implant integration and stability | High cost, limited availability |
| Growth Factor-Based Bone Regeneration | Increased bone density and quality | Potential for overstimulation and excessive bone growth |
| Bone Grafting Material-Based Bone Regeneration | Cost-effective, widely available | Potential for graft rejection, limited long-term stability |
End of Discussion

Throughout this narrative, we’ve delved into the intricacies of dental implant healing, highlighting the importance of each stage in the process. From initial healing to osseointegration and bone regeneration, every step is critical in ensuring the success of dental implant integration. With proper care and understanding of the recovery process, patients can enjoy a healthier, happier smile.
Quick FAQs
Q: What is the average recovery time for dental implant surgery?
A: The average recovery time for dental implant surgery can vary from person to person, but typically ranges from 3-6 months.
Q: Can smoking habits affect the healing time of dental implants?
A: Yes, smoking can significantly impact the healing time of dental implants, as it reduces blood flow and oxygenation to the affected area.
Q: What are some common complications associated with dental implant healing?
A: Some common complications associated with dental implant healing include implant failure, infection, and nerve damage.
Q: Can dental implant failure be prevented?
A: Yes, dental implant failure can be minimized through proper placement and angulation of the implant, as well as regular follow-up appointments with your dentist.
Q: How long does it take for dental implants to fully integrate with the surrounding bone?
A: The full integration of dental implants with the surrounding bone typically takes several months to a year after the initial placement.