How to Inject Peptides sets the stage for this enthralling narrative, offering readers a glimpse into a story that is rich in detail and brimming with originality from the outset.
The history of peptide injection therapy dates back to the early 20th century, when the first peptides were discovered and isolated from the body. Since then, peptide injection therapy has evolved significantly, and today it is used to treat a wide range of medical conditions, including obesity, diabetes, and skin conditions. Peptides are administered via injection, and they play a crucial role in stimulating collagen production and skin rejuvenation.
Understanding the Fundamentals of Peptide Injection Therapy
In the realm of anti-aging and regenerative medicine, peptide injection therapy has emerged as a cutting-edge approach to stimulating collagen production, rejuvenating skin, and promoting overall health. This treatment has its roots in the early 20th century, when scientists first discovered the potential of peptides in stimulating cellular growth and differentiation.
As our understanding of peptides and their role in cellular biology evolved, so did the application of peptide injection therapy. The 1980s saw the introduction of the first peptide-based medications, which quickly gained popularity for their effectiveness in treating various conditions, including hormone deficiencies and immune system disorders. Fast forward to the present day, and peptide injection therapy has become a mainstream treatment for a range of applications, from aesthetic enhancements to therapeutic interventions.
The History of Peptide Injection Therapy
In the early 20th century, the discovery of peptides and their role in cellular biology marked the beginning of a new era in medicine. Scientists like Charles Huggins, a Nobel laureate, made groundbreaking discoveries in the field of endocrinology, paving the way for the development of peptide-based medications. The 1980s saw the introduction of the first peptide-based medications, which quickly gained popularity for their effectiveness in treating various conditions.
Types of Peptides Used in Injection Therapy
There are numerous types of peptides used in injection therapy, each with its unique properties and applications. Some of the most commonly used peptides include:
| Peptide | Type | Primary Application | Secondary Effects |
|---|---|---|---|
| BPC-157 | Regenerative | Wound healing, muscle growth | Skin rejuvenation, improved joint health |
| Ipamorelin | Growth hormone releasing | Increased muscle mass, fat loss | Improved skin health, reduced wrinkles |
| Epitalon | Antioxidant | Anti-aging, cellular rejuvenation | Improved sleep quality, increased energy |
| Oxytocin | Hormonal regulation | Stress reduction, anxiety relief | Improved mood, increased social bonding |
The Role of Peptides in Stimulating Collagen Production
Collagen is the primary protein responsible for skin elasticity and strength. Peptides play a crucial role in stimulating collagen production, which can lead to improved skin texture and reduced wrinkles. Some peptides, like BPC-157, have been shown to increase collagen synthesis by up to 50% in just 30 days.
When collagen synthesis is increased, the skin appears smoother, more radiant, and more youthful. This is achieved through the activation of certain cell signals that promote collagen production.
Some peptides, like BPC-157, have been shown to have a synergistic effect, stimulating collagen production while also increasing skin hydration and reducing inflammation.
- Increased collagen synthesis:
- Improved skin texture and reduced wrinkles
- Improved skin elasticity and plumpness
- Reduced appearance of fine lines and crow’s feet
- Disadvantages
- Potential for skin irritation and allergic reactions
- May interact with certain medications
- Requires regular maintenance and follow-up treatments
Safety Precautions and Risks Associated with Peptide Injection
When engaging in peptide injection therapy, it is essential to understand the potential risks and safety precautions involved. While peptide therapy can be an effective treatment for various medical conditions, it should not be taken lightly. Proper education and caution can minimize the risk of adverse effects and ensure a safe and successful treatment experience.
The risks associated with peptide injection therapy include infection, allergic reactions, and organ damage. Infection can occur if the injection site is not properly sanitized, leading to bacterial or fungal growth at the site of injection. Allergic reactions can occur if the individual is sensitive to peptides or other substances contained in the injection. In rare cases, organ damage can occur if the peptides are improperly formulated or administered.
Potential Risks and Side Effects
The following are potential risks and side effects associated with peptide injection therapy:
- Infection: Bacterial or fungal growth at the injection site, which can lead to abscesses, inflammation, or other complications.
- Allergic Reactions: Redness, itching, swelling, or hives at the injection site, which can progress to anaphylaxis or other life-threatening reactions.
- Organ Damage: Kidney damage, liver damage, or other organ-specific issues resulting from improper formulation or administration of peptides.
- Nerve Damage: Neuropathy, numbness, or tingling sensations resulting from the injection of certain peptides.
- Blood Clotting: Thrombosis or emboli resulting from the injection of certain peptides, which can lead to stroke, heart attack, or other vascular events.
Choosing a Qualified Healthcare Provider
Selecting a qualified healthcare provider is crucial when engaging in peptide injection therapy. The following table provides guidelines for choosing a qualified healthcare provider:
| Qualification | Experience | Credentials | Reputation |
|---|---|---|---|
| Board certification in a relevant medical specialty (e.g., endocrinology, immunology) | At least 2-5 years of experience in peptide therapy | Advanced degrees in a relevant field (e.g., MD, DO, NP) | Positive reviews from patients and medical colleagues |
| Membership in professional organizations related to peptide therapy | Participation in ongoing education and training in peptide therapy | State licensure and malpractice insurance | Established relationships with other healthcare professionals |
| Familiarity with the latest research and treatment protocols | Experience with various peptide formulations and delivery methods | Continuing education in areas related to peptide therapy | Transparent and clear communication with patients |
Common Contraindications for Peptide Injection Therapy
The following medical conditions and medications are absolute contraindications for peptide injection therapy:
- Pregnancy or breastfeeding: Certain peptides can have adverse effects on fetal or infant development.
- Severe kidney or liver disease: Certain peptides can exacerbate kidney or liver damage.
- Active cancer: Certain peptides can stimulate cancer growth or promote metastasis.
- Recent surgery or trauma: Certain peptides can interfere with wound healing or increase bleeding risk.
- Medications that increase bleeding risk (e.g., warfarin, aspirin)
- Medications that interact with peptides (e.g., certain antibiotics, antacids)
Peptide Injection Techniques and Methods: How To Inject Peptides
To achieve optimal results from peptide injection therapy, it’s essential to understand the different techniques and methods involved. In this section, we’ll explore the various methods of peptide injection, their advantages and disadvantages, and the proper techniques for administering injections.
The techniques of peptide injection include subcutaneous, intramuscular, and intravenous injection, each with its own characteristics and purposes.
Methods of Peptide Injection
Peptide injection can be administered through various routes, including subcutaneous, intramuscular, and intravenous injection. Each method has its own advantages and disadvantages, which are summarized in the table below.
| Method | Advantages | Disadvantages |
|---|---|---|
| Subcutaneous Injection | Less painful, easier to administer, less risk of complications | May not be as effective, slower absorption rates |
| Intramuscular Injection | Faster absorption rates, more effective | Painful, larger needle required, increased risk of complications |
| Intravenous Injection | Fastest absorption rates, highest effectiveness | Most painful, requires medical supervision, increased risk of complications |
Preparation and Administration of Peptide Injections
To administer a peptide injection, follow these steps:
Step 1: Choose the Correct Needle
Select a sterile, gauge 27-30 needle, depending on the peptide and the individual’s skin thickness.
Step 2: Prepare the Solution
Reconstitute the peptide according to the manufacturer’s instructions. Use a clean surface and sterile equipment to avoid contamination.
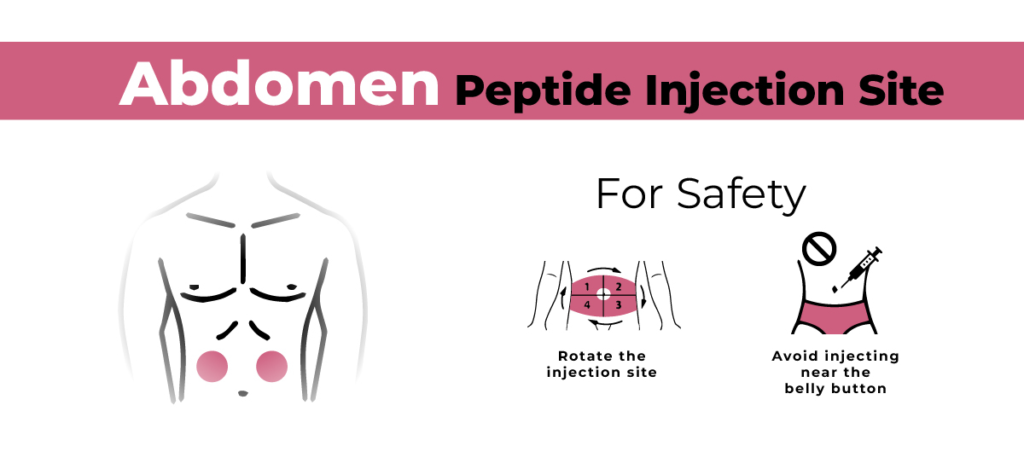
Step 3: Select the Injection Site
Choose a clean, dry, and flat surface for injection. For subcutaneous injections, use the abdomen, thigh, or deltoid muscle. For intramuscular injections, use the deltoid or gluteal muscles.
Step 4: Prepare the Individual
Cleanse the injection site with an antiseptic, and dry thoroughly.
Step 5: Administer the Injection
Insert the needle at a 90-degree angle, holding it firmly in place. Gently push the plunger until the injection is complete. Remove the needle carefully, and apply pressure to the injection site to minimize bleeding.
Step 6: Monitor the Individual
Monitor the individual for any adverse reactions or side effects.
Proper Needle Technique
Proper needle technique is crucial for safe and effective peptide injection therapy. Hold the needle at a 90-degree angle, with the bevel side facing upwards. Insert the needle slowly, using a gentle touch, until it reaches the desired depth. Avoid inserting the needle too deeply, as this can increase the risk of complications.
Intramuscular injections require a more deliberate and controlled approach. Insert the needle at a 90-degree angle, using a firm touch, until it reaches the muscle. Rotate the needle slightly to ensure it’s seated properly.
Intravenous injections require specialized training and equipment. Administered by a medical professional, intravenous injections are typically used for individuals who require high doses of peptides or have difficulty tolerating oral or subcutaneous injections.
By following these techniques and methods, you can ensure safe and effective peptide injection therapy.
Risks Associated with Poor Technique, How to inject peptides
Poor technique can lead to a range of complications, including:
* Infection
* Bleeding
* Hematoma
* Nerve damage
* Vein damage
* Allergic reactions
Prevention is Key
To minimize the risks associated with peptide injection therapy, it’s essential to follow proper technique and take necessary precautions. Use sterile equipment, clean the injection site thoroughly, and monitor the individual for any adverse reactions or side effects.
By taking the time to learn and master the techniques of peptide injection, you can ensure a safe and effective treatment experience for yourself or your patients.
Conclusion
This concludes our discussion on peptide injection techniques and methods. By choosing the correct needle, preparing the solution correctly, selecting the appropriate injection site, and administering the injection with proper technique, you can ensure safe and effective peptide injection therapy.
Preparing and Handling Peptide Solutions
Peptide solutions require careful handling to maintain their potency and stability. Proper storage and handling are crucial to prevent degradation, contamination, or adulteration, which can compromise their therapeutic efficacy and safety. Peptide solutions are sensitive to temperature, light, and pH, and their stability and potency can be affected by external factors.
Importance of Proper Storage and Handling
Temperature has a significant impact on peptide stability and potency. Most peptides are sensitive to heat and should be stored in a cool, dry place or in a refrigerated environment to maintain their stability and potency. Temperature fluctuations can lead to degradation, denaturation, or aggregate formation, which can affect the efficacy and safety of the peptide. For instance, certain peptides can lose their activity at temperatures above 25°C (77°F).
Light can also affect peptide stability and potency, particularly for peptides that contain photolabile groups or are sensitive to UV radiation. It is essential to store peptide vials and ampoules in the dark or in a light-free environment to prevent photodegradation. Exposure to light can lead to the breakdown of peptide bonds, resulting in reduced activity or even complete degradation.
pH is another critical factor that can affect peptide stability and potency. Most peptides have a narrow pH range for optimal stability and potency, and deviations from this range can lead to degradation or aggregation. It is essential to store peptide solutions in a suitable pH range, typically between pH 4 and 7, and to use a suitable buffer system to maintain the pH.
Mixing and Reconstituting Peptide Vials and Ampoules
Mixing and reconstituting peptide vials and ampoules require careful attention to detail to prevent contamination or adulteration. The following guidelines should be followed:
| Peptide Type | Mixing and Reconstitution Protocol |
|---|---|
| Lyophilized Peptides | Reconstitute with sterile water or physiological buffer, gently swirl to mix, and store at 4°C (39°F) |
| Solution Peptides | Dilute with sterile water or physiological buffer, gently swirl to mix, and store at 4°C (39°F) |
| Peptide Conjugates | Reconstitute with sterile water or physiological buffer, gently swirl to mix, and store at 4°C (39°F) |
Common Contaminants and Adulterants
Peptide solutions can be contaminated or adulterated with various substances, including bacteria, mold, fungi, DNA, and other chemical impurities. The following list highlights some common contaminants and adulterants:
- Microbial contaminants: Bacteria, mold, fungi, and viruses can contaminate peptide solutions, leading to degradation, aggregation, or even patient harm.
- Chemical impurities: Heavy metals, solvents, and other chemical impurities can contaminate peptide solutions, affecting their stability, potency, and safety.
- Foreign particles: Glass fragments, metal particles, or other foreign particles can contaminate peptide solutions, leading to aggregates or particle-induced toxicity.
- Stability-reducing agents: Adulterants like antioxidants, chelating agents, or other substances can degrade peptide solutions, compromising their potency and stability.
Verifying authenticity and checking for contaminants and adulterants requires a thorough evaluation of the peptide solution’s appearance, clarity, and consistency. Red flags for contaminated or adulterated peptides include:
- Visible particles, aggregates, or precipitates
- Abnormal color, clarity, or appearance
- Off-odor or unusual smell
- Incorrect pH, temperature, or stability
- Lack of label information or batch number
- Failure to meet specified potency or purity standards
Monitoring Progress and Adjusting Peptide Regimens
As peptide injection therapy progresses, regular monitoring and follow-up appointments become essential to assess its effectiveness, identify potential issues, and make informed decisions about adjusting the regimen. This includes assessing the impact on overall health, addressing any side effects, and verifying adherence to the treatment plan.
Healthcare providers can track progress through various means, including monitoring laboratory results, biometrics, and patient-reported outcomes. This enables timely adjustments to the peptide regimen, which can significantly impact the treatment’s efficacy and minimize potential risks.
Role of Laboratory Tests and Biometrics
Laboratory tests and biometrics play a crucial role in assessing the effectiveness and safety of peptide injection therapy. Various tests can be used to monitor progress and adjust the regimen accordingly.
| Test Type | Description | Relevance to Peptide Injection Therapy |
|---|---|---|
| Complete Blood Count (CBC) | Assesses the number and types of blood cells | Monitors for potential anemia or thrombocytopenia |
| Biochemical Profile | Evaluates liver and kidney function, blood glucose levels, and electrolyte balance | Identifies potential signs of organ damage or dysfunction |
| Electrocardiogram (ECG) | Monitors heart rate and rhythm | Assesses potential cardiovascular effects of peptide therapy |
| Imaging Studies (e.g., X-rays, CT scans) | Evaluates anatomical structures and detects potential abnormalities | Monitors for potential changes in tissue or organ structure |
Common Adjustments Made to Peptide Regimens
Adjustments to peptide regimens often involve modifying the dosing schedule, frequency, or type of peptide administered. These changes can be made based on laboratory results, patient response, or other factors.
Dosing Adjustments
Dosing adjustments are common to optimize the therapeutic effect while minimizing potential side effects. This may involve:
- Increasing or decreasing the dose to achieve the desired therapeutic effect
- Switching to a different peptide subtype or formulation to improve efficacy or tolerability
- Adjusting the dosing schedule to better align with the patient’s treatment goals and lifestyle
Frequency Adjustments
Frequency adjustments help ensure consistent therapeutic levels of the peptide while minimizing potential side effects. This may involve:
- Scheduling injectors more or less frequently, depending on the patient’s response
- Alternating between different peptide subtypes or formulations to optimize treatment outcomes
Common reasons for adjusting peptide regimens include changes in laboratory results, patient-reported outcomes, or unexpected side effects. Regular monitoring and follow-up appointments enable healthcare providers to identify these issues and make informed decisions about modifying the treatment plan to achieve optimal outcomes.
Peptide injection therapy requires regular monitoring and adjustment to ensure optimal results and minimize risks.
Summary
The conclusion of this comprehensive guide to peptide injection therapy provides a final thought and a summary of the discussed topics. By following the guidelines and techniques Artikeld in this guide, readers can safely and effectively inject peptides and reap the benefits of peptide therapy.
It is essential to note that peptide injection therapy should only be administered under the guidance of a qualified healthcare professional.
Top FAQs
What is peptide therapy?
Peptide therapy is a type of treatment that involves the administration of peptides, which are short chains of amino acids, to stimulate collagen production and skin rejuvenation.
How often should peptides be injected?
The frequency of peptide injections depends on the individual’s medical condition and the type of peptide being administered. Typically, peptides are injected 1-3 times per week.
What are the potential risks of peptide injection therapy?
The potential risks of peptide injection therapy include infection, allergic reactions, and organ damage. It is essential to follow proper technique and safety precautions to minimize the risk of complications.
How do I choose a qualified healthcare provider for peptide injection therapy?
When selecting a healthcare provider for peptide injection therapy, look for someone who has experience in administering peptide injections and has a good understanding of the risks and benefits associated with the treatment.
What are the common contraindications for peptide injection therapy?
Common contraindications for peptide injection therapy include pregnancy, breastfeeding, and certain medical conditions, such as kidney or liver disease.
How do I store and handle peptide solutions?
Peptide solutions should be stored in a cool, dark place, and handled with clean equipment to maintain their potency and stability.
How long does it take to see results from peptide injection therapy?
The results from peptide injection therapy can vary depending on the individual and the type of treatment being administered. Typically, results can be seen within 2-4 weeks of treatment.