How to know if you have gingivitis sets the stage for this enthralling narrative, offering readers a glimpse into a story that is rich in detail, brimming with originality from the outset. As we delve into the world of dental health, it is essential to understand the warning signs of this condition, particularly in children, to prevent its progression into periodontal diseases.
Gingivitis, an inflammatory disease of the gums, affects not only adults but also children, often caused by poor oral hygiene, diet, or hormonal imbalances. Recognizing the symptoms early on is crucial in developing a personalized prevention plan. This article will guide you through the signs of gingivitis in children, differentiating it from other periodontal diseases, and understanding the impact of hormonal changes and genetics on its development.
Identifying Early Warning Signs of Gingivitis in Children
As a parent, it’s natural to be concerned about your child’s overall health, including their dental well-being. Gingivitis, an inflammatory condition characterized by red and swollen gums, can have a significant impact on a child’s quality of life, affecting their self-esteem, dietary preferences, and even their concentration in school. Early identification and treatment of gingivitis are crucial to preventing more severe complications such as periodontitis, tooth loss, and systemic infections.
Monitoring your child’s dental health habits and being aware of the early warning signs can help you address this issue before it worsens. Children, just like adults, can unknowingly contribute to gingivitis through poor oral hygiene, inadequate diet, and other factors. For example, sucking on hard objects like lollipops or pens can cause excessive pressure on the teeth and gums, while consuming sugary snacks and drinks repeatedly can lead to an increase in plaque formation.
Common Signs of Gingivitis in Children
Children’s dental health can be quite different from that of adults, making it important to understand the specific signs and symptoms of gingivitis in this age group.
Children with gingivitis may exhibit the following signs and symptoms, which can vary in severity and duration:
- Red or swollen gums that are tender to the touch, especially when smiling or biting down
- Difficulty swallowing food due to mouth pain or discomfort
- Sensitivity to hot or cold foods and drinks
- Bleeding gums, especially during brushing or flossing
- Receding gums, creating a “gum recession” around the teeth
- Bad breath or an unpleasant mouth odor
- A slight change in the color or texture of the gums
Avoiding Common Mistakes that can Contribute to Gingivitis
It’s essential to encourage good oral hygiene habits in your child, such as regular brushing and flossing, to reduce the risk of gingivitis. Additionally, teaching your child how to care for their teeth and gums properly can help prevent more severe dental problems. Some common mistakes to avoid include:
- Not establishing a regular brushing and flossing routine, especially after meals and snacks
- Using a toothbrush with hard bristles that can damage gums and tooth enamel
- Consuming excessive amounts of sugary snacks and drinks that contribute to plaque formation
- Not visiting the dentist regularly for check-ups and cleanings
- Not being aware of the importance of fluoride toothpaste for children’s dental health
As a parent, being proactive in monitoring your child’s dental health and teaching them good oral hygiene habits can significantly reduce the risk of gingivitis. Regular check-ups with a pediatric dentist and maintaining an open line of communication with your child about their dental health can help ensure a healthy and beautiful smile throughout their childhood and beyond.
Differentiation between Gingivitis and Other Periodontal Diseases
Gingivitis is a common oral health issue that affects millions of people worldwide. While it’s often associated with red, swollen, and bleeding gums, not all gum inflammation is gingivitis. In this article, we’ll delve into the world of periodontal diseases, exploring their characteristics, symptoms, causes, and treatments to help you accurately diagnose and address this oral health concern.
Periodontal diseases encompass a range of conditions that affect the gums and bone supporting the teeth. While gingivitis is the mildest form, it can progress to more severe conditions like periodontitis, perio-endo lesions, and other infections. To differentiate between these diseases, it’s essential to understand their distinct features.
Comparative Analysis of Gingivitis, Periodontitis, and Other Periodontal Diseases
Periodontal diseases share some common characteristics, but their symptoms, causes, and treatments differ significantly. Here’s a detailed table comparing the key features of each condition:
| Condition | Key Symptoms | Causes and Treatment Options |
|---|---|---|
| Gingivitis | Red, swollen, and bleeding gums; mild gum recession | Caused by poor oral hygiene, smoking, and hormonal changes. Treatments include improved oral hygiene practices, professional cleaning, and, in severe cases, medicated mouthwashes. |
| Periodontitis | Deep gum recession, exposed roots, and loose teeth; chronic bad breath and gum abscesses | Caused by a combination of poor oral hygiene, smoking, and genetic predisposition. Treatments include deep cleaning, antibiotics, and, in severe cases, surgery to repair damaged bone and gum tissue. |
| Perio-endo Lesions | Damage to the periodontal ligament, leading to root resorption and tooth loss | Caused by severe periodontitis, trauma, or orthodontic treatment. Treatments include root canal therapy, dental implants, or, in some cases, extracting the affected tooth. |
| Other Infections | Painful gums, swollen facial tissues, and fever; abscesses or pus discharge; bleeding gums and bad breath | Caused by bacterial or fungal infections, dental work, or other underlying conditions. Treatments include antibiotics, drainage of abscesses, or, in severe cases, hospitalization to manage life-threatening infections. |
Remember, early detection and treatment are crucial to preventing these conditions from progressing and causing irreversible damage. Regular dental check-ups, proper oral hygiene practices, and a balanced diet rich in essential nutrients can help maintain healthy gums and teeth throughout your life.
Conclusion
By understanding the characteristics, symptoms, causes, and treatments of gingivitis and other periodontal diseases, you can make informed decisions about your oral health. Remember that prevention is key, and regular dental care, combined with a healthy lifestyle, can help you maintain a beautiful, healthy smile for years to come.
Common Misconceptions about Gingivitis Prevention and Treatment
Gingivitis, a mild form of gum disease, can often be misunderstood, leading to incorrect assumptions about its causes and prevention. Unfortunately, many of these misconceptions can hinder efforts to prevent and treat the disease. In this section, we’ll address some of the most common misconceptions and separate fact from fiction.
The Importance of Misconception Correction, How to know if you have gingivitis
Correcting common misconceptions is crucial for effective gingivitis prevention and treatment. If we’re misinformed about the causes of gum disease, we may prioritize the wrong factors, leading to inadequate preventive measures or delayed treatment. By understanding the facts, individuals can take informed decisions to protect their oral health.
Misconceptions about Gingivitis Prevention
Misconceptions about gingivitis prevention can be misleading, leading to inadequate care routines. Here are some common misconceptions and the facts:
| Misconception | Fact |
|---|---|
| Regular toothbrushing is enough to prevent gingivitis. | While regular toothbrushing is essential, it’s not sufficient on its own to prevent gingivitis. Regular flossing, tongue scraping, and professional cleanings are also necessary. |
| Gingivitis is caused by poor oral hygiene alone. | Gingivitis is a bacterial infection caused by a combination of poor oral hygiene, diet, and systemic factors, such as smoking and hormonal changes. |
| Diet has no impact on gingivitis development. | A diet high in sugar, salt, and refined carbohydrates can contribute to gingivitis development, while a balanced diet rich in fruits, vegetables, and whole grains can help prevent it. |
Correcting these misconceptions can help individuals prioritize effective prevention and early treatment strategies, ultimately leading to better oral health outcomes.
Personalized Gingivitis Prevention Plans Based on Oral Health History
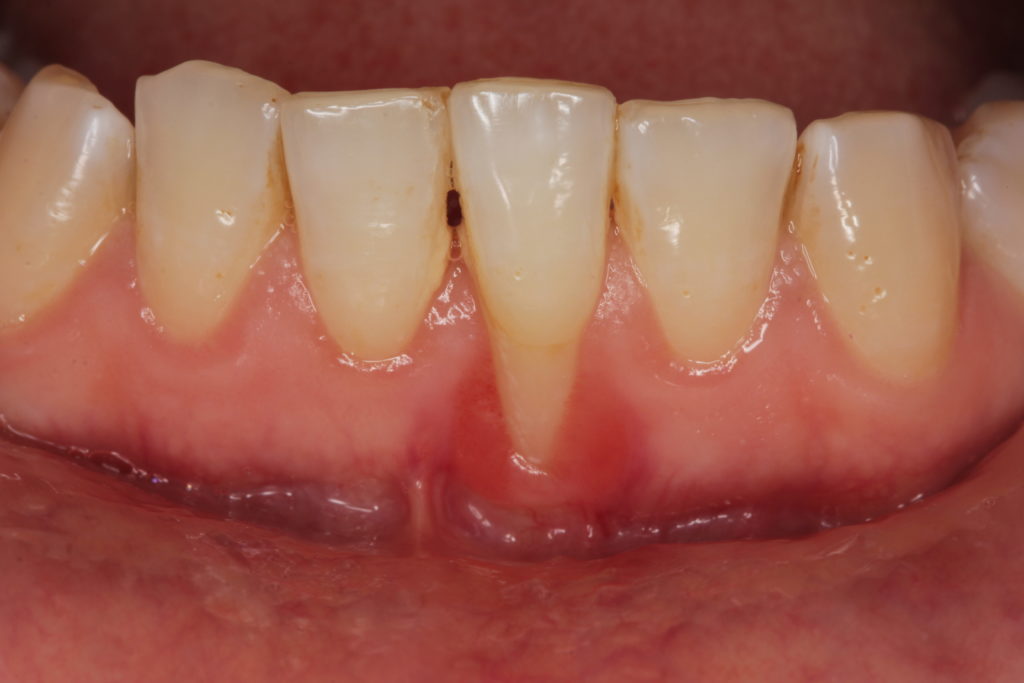
In the realm of oral health, one size does not fit all. Each individual’s oral health history is unique, shaped by a complex interplay of factors including genetics, lifestyle, diet, and previous dental experiences. As such, a tailored approach to preventing gingivitis is essential to ensure effective results. This approach not only helps to prevent the onset of this often-misunderstood condition but also helps to maintain optimal oral health for individuals across all age groups. By taking into account a patient’s individual oral health history and needs, dental professionals can create a personalized gingivitis prevention plan that addresses specific risk factors, promotes healthy habits, and fosters a deeper understanding of the dynamics at play in maintaining a healthy smile.
A comprehensive oral health assessment serves as the foundation upon which a personalized gingivitis prevention plan is built. This thorough evaluation of an individual’s oral health enables dental professionals to identify areas of strength and vulnerability, pinpoint potential risk factors, and develop targeted strategies for improvement. In other words, it is only when we have a clear understanding of our oral health landscape that we can tailor our approach to effectively prevent gingivitis and maintain optimal oral well-being.
Creating a Comprehensive Oral Health Assessment and Tailored Prevention Strategy
When it comes to creating a comprehensive oral health assessment, several key components must be considered.
-
Medical History Review
A thorough review of an individual’s medical history is crucial in identifying potential risk factors for gingivitis. This may include a history of respiratory or cardiovascular disease, pregnancy, or other conditions that could impact oral health. By factoring in medical history, dental professionals can better understand how individual health factors may influence oral health outcomes. -
Oral Examination
Conducting a thorough oral examination allows dental professionals to assess the health of an individual’s teeth, gums, and supporting tissues. This includes evaluating the presence of any signs of gum disease, tooth decay, or other oral health issues that could contribute to gingivitis. -
Diagnostic Tests
Diagnostic tests such as X-rays, dental CT scans, and other imaging modalities can help identify potential issues that may not be visible during a routine oral examination. These tests can provide crucial insights into an individual’s oral health and help identify potential risk factors for gingivitis. -
Patient History and Lifestyle Assessment
A comprehensive assessment of an individual’s lifestyle and habits is also essential in identifying potential risk factors for gingivitis. This includes evaluating diet, smoking habits, alcohol consumption, and other factors that could impact oral health. -
Risk Factor Analysis
Based on the findings of the oral health assessment, dental professionals can identify specific risk factors for gingivitis and develop targeted strategies to address these risks.
By systematically evaluating these key components, dental professionals can develop a comprehensive oral health assessment that provides a solid foundation for a personalized gingivitis prevention plan. This tailored approach allows individuals to take control of their oral health and work in partnership with their dental professionals to maintain optimal health and well-being.
To illustrate the importance of a comprehensive oral health assessment and tailored prevention strategy, let’s consider a few real-life examples.
For instance, imagine a patient who has a history of periodontal disease and is at high risk for developing gingivitis. By conducting a thorough oral examination and diagnostic tests, dental professionals can identify potential areas of concern and develop a personalized prevention plan that addresses specific risk factors and fosters a deeper understanding of the dynamics at play in maintaining a healthy smile.
Similarly, a patient who has been diagnosed with diabetes may require a customized prevention plan that takes into account the unique oral health challenges associated with this condition. In this case, dental professionals may recommend a more frequent oral health monitoring schedule, tailored diet and lifestyle recommendations, and personalized oral hygiene instructions to help manage oral health risks.
In each of these examples, a comprehensive oral health assessment and tailored prevention strategy play a critical role in preventing gingivitis and maintaining optimal oral health. By understanding an individual’s unique oral health history and needs, dental professionals can develop targeted strategies that address specific risk factors and foster a deeper understanding of the dynamics at play in maintaining a healthy smile.
Final Summary: How To Know If You Have Gingivitis

As we conclude our discussion on how to know if you have gingivitis, remember that prevention is key. By understanding the causes and signs of this condition, you can take the necessary steps to maintain good oral health. Develop a personalized prevention plan, practice good oral hygiene, and visit your dentist regularly to prevent the progression of gingivitis to more severe periodontal diseases.
Don’t wait until it’s too late; take control of your oral health today and discover the connection between a healthy smile and a healthier body.
FAQ Resource
Is gingivitis reversible?
Yes, gingivitis is reversible by maintaining good oral hygiene, reducing plaque and tartar buildup, and treating any underlying infections or conditions.
Can gingivitis cause heart disease?
Research suggests that there is a link between gingivitis and heart disease, as the bacteria causing gingivitis can enter the bloodstream, leading to inflammation and potentially causing cardiovascular issues.
How often should I visit my dentist for a check-up?
It is recommended to visit your dentist at least twice a year for a check-up to ensure early detection and prevention of oral health issues, including gingivitis.