Dry socket how long does it take to heal is a crucial inquiry you should make after experiencing tooth extraction pain that refuses to subside. The narrative of dry socket healing is rich in detail, with a clear timeline that Artikels the progression from initial infection to complete recovery. As we delve into the story, you’ll uncover essential insights into the causes of dry socket, the factors that contribute to its formation, and the effective strategies for managing pain and discomfort.
The healing process of dry socket involves several stages, and understanding these stages can help you navigate this complex journey. In this narrative, you’ll discover the importance of dental hygiene, the role of bacteria in dry socket formation, and the significance of pain management in the healing process. Our aim is to provide you with a comprehensive understanding of dry socket, enabling you to take control of your recovery and make informed decisions about your oral health.
Managing Dry Socket Pain and Discomfort: Dry Socket How Long Does It Take To Heal
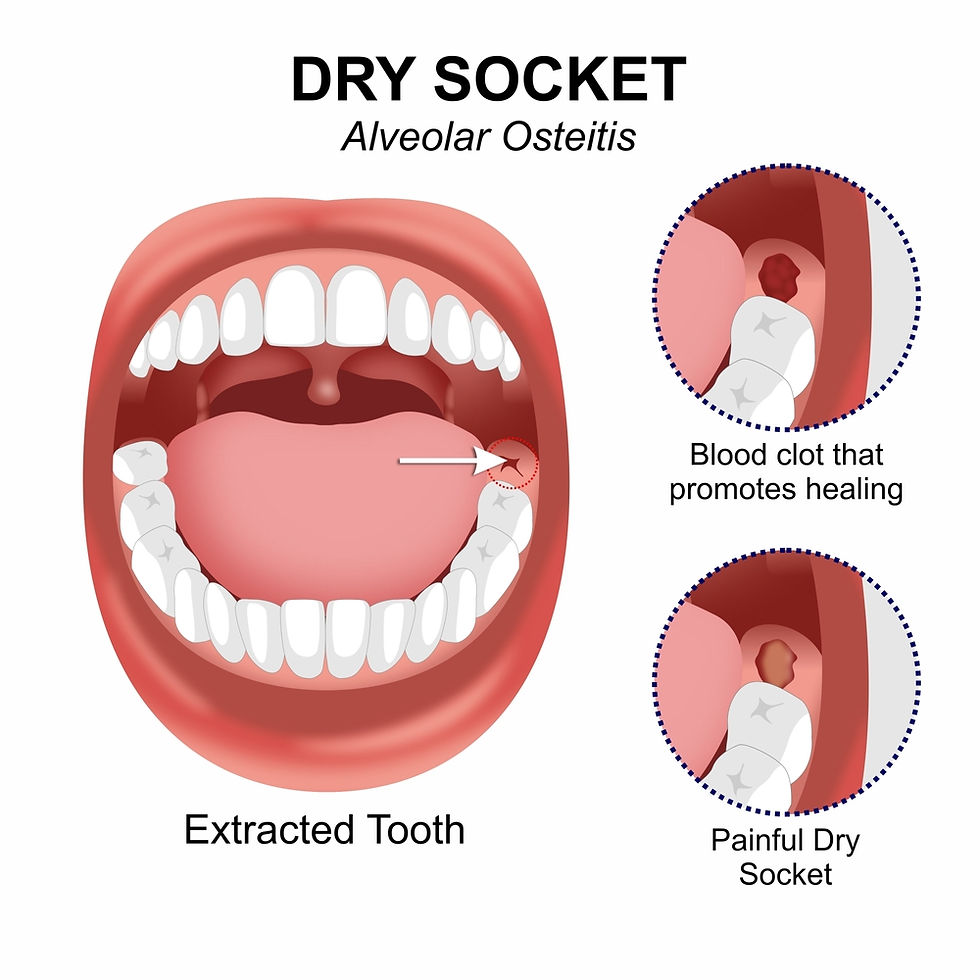
Dry socket, also known as alveolar osteitis, is a painful complication that can occur after tooth extraction. The prolonged healing process can lead to various symptoms, including pain, swelling, and difficulty eating or speaking. In this section, we will discuss the various symptoms associated with dry socket and explore effective strategies for managing pain and discomfort.
Prolonged bleeding, sharp pain, and difficulty managing daily activities are the common symptoms of dry socket. The condition arises when the blood clot that forms over the extraction site is dislodged or fails to develop properly. This can cause the bone and nerves to become exposed, leading to extreme pain and discomfort.
Pain management is a crucial aspect of dry socket treatment. Various over-the-counter and prescription medications can help alleviate symptoms.
Benefits of Saltwater Rinses
Saltwater rinses have been found to promote healing and reduce dry socket symptoms. The antibacterial properties of salt help maintain a clean extraction site, reducing the risk of infection. Additionally, saltwater rinses can help reduce pain by promoting the formation of a new blood clot.
For example, a study published in the Journal of Oral and Maxillofacial Surgery found that participants who used saltwater rinses after tooth extraction experienced fewer dry socket complications compared to those who did not use the rinse.
To prepare a saltwater rinse, dissolve 1 teaspoon of salt in 8 ounces of warm water. Swish the solution around your mouth for 30 seconds and spit it out. Repeat this process several times a day to promote healing and reduce symptoms.
Pain Management Strategies
Over-the-counter pain medications, such as ibuprofen or acetaminophen, can help alleviate dry socket symptoms. These medications work by blocking the production of pain-causing chemicals in the body. However, it is essential to follow the recommended dosage and consult with your dentist or healthcare professional before taking any medication.
Prescription pain medications may be necessary for more severe cases of dry socket. These medications can be more effective in managing pain, but they also come with a higher risk of side effects.
In some cases, dry socket pain can be managed with a pain-relieving gel or patch. These products contain ingredients that block pain receptors and provide sustained relief.
Dental Care Strategies, Dry socket how long does it take to heal
Proper dental care is essential for managing dry socket symptoms. Avoid rinsing with hot water, as this can dislodge the blood clot and worsen symptoms. Instead, rinse with cold water or a saltwater solution.
To reduce swelling and promote healing, apply an ice pack or a cold compress to the affected area for 15-20 minutes. Elevate your head while sleeping to reduce swelling and promote draining of the blood clot.
Follow a healthy diet that is rich in nutrients and avoids spicy or hard-to-chew foods, which can worsen symptoms. Quit smoking and limit alcohol consumption, as these habits can slow down the healing process.
Reducing the Risk of Dry Socket Formation
Reducing the risk of dry socket formation after tooth extraction involves taking essential steps to prevent complications. A dry socket occurs when the blood clot that forms in the socket is dislodged, exposing the underlying bone and nerve endings. This can be a painful and potentially serious condition that can prolong recovery and increase the risk of infection. Therefore, it is crucial to follow proper post-extraction care and take preventive measures to minimize the risk of dry socket formation.
Post-Extraction Care Instructions
To prevent dry socket formation, it is essential to follow the post-extraction care instructions provided by a dentist or oral surgeon. These instructions may include:
- Do not smoke or use tobacco products for at least 24 hours after tooth extraction, as smoking can delay healing and increase the risk of dry socket.
- Do not drink through a straw, as this can dislodge the blood clot and increase the risk of dry socket.
- Avoid eating hard, hot, or spicy foods for the first 24 hours after tooth extraction, as these can irritate the socket and increase the risk of dry socket.
- Take over-the-counter pain medication as directed by your dentist or oral surgeon to manage pain and discomfort.
- Do not touch or manipulate the socket area, as this can dislodge the blood clot and increase the risk of dry socket.
- Follow a gentle oral hygiene routine, including brushing and flossing around the extraction site, to prevent infection and promote healing.
These post-extraction care instructions are crucial in preventing dry socket formation and promoting a smooth and speedy recovery.
The Importance of Good Oral Hygiene
Good oral hygiene plays a vital role in minimizing the risk of dry socket and other post-extraction complications. After tooth extraction, it is essential to maintain good oral hygiene by:
- Brushing the teeth gently around the extraction site to prevent infection and promote healing.
- Flossing to remove food particles and debris from around the extraction site.
- Rinsing the mouth with saltwater or a antibacterial mouthwash to reduce the risk of infection.
- Using a soft-bristled toothbrush to clean the teeth and prevent irritation to the extraction site.
By maintaining good oral hygiene, you can reduce the risk of dry socket and other post-extraction complications, promote a smooth and speedy recovery, and ensure the best possible outcome for your dental health.
Reducing the Risk of Dry Socket with Antibiotics
In some cases, a dentist or oral surgeon may prescribe antibiotics to reduce the risk of dry socket and other post-extraction complications. Antibiotics can help prevent infection by killing bacteria that can accumulate at the extraction site. However, it is essential to follow the instructions provided by your dentist or oral surgeon and complete the full course of antibiotics to ensure effective prevention of dry socket and other complications.
Reducing the Risk of Dry Socket with Pain Management
Pain management is a critical aspect of preventing dry socket formation. After tooth extraction, it is essential to manage pain and discomfort effectively to prevent the formation of a dry socket. This can be done by:
- Following a pain management plan provided by your dentist or oral surgeon.
- Taking over-the-counter pain medication as directed.
- Using a cold compress or ice pack to reduce swelling and alleviate pain.
- Practicing relaxation techniques, such as deep breathing or meditation, to manage stress and anxiety.
By managing pain and discomfort effectively, you can reduce the risk of dry socket formation and promote a smooth and speedy recovery.
Reducing the Risk of Dry Socket with Follow-Up Care
Follow-up care is critical in preventing dry socket formation and promoting a smooth and speedy recovery. Regular follow-up appointments with your dentist or oral surgeon can help monitor healing progress, identify potential complications, and provide guidance on post-extraction care and pain management. By following up with your dentist or oral surgeon as recommended, you can reduce the risk of dry socket formation and ensure the best possible outcome for your dental health.
Treatment Options for Dry Socket
Dry socket, a painful sequela of tooth extraction, necessitates effective treatment to promote healing and alleviate discomfort. A comprehensive understanding of available treatment options is crucial for healthcare providers to manage this complication.
Debridement
Debridement is a common treatment approach for dry socket, involving the gentle removal of fibrinous tissue and blood clots from the extraction socket. This procedure helps to eliminate bacteria and debris, promoting a clean environment for healing. Debridement can be performed using saline rinse, hydrocortisone gel, or hydrogen peroxide.
Debridement can be achieved through various methods:
-
–
Saline rinse: A gentle flushing of the socket with saline solution to remove debris and promote drainage.
-
–
Hydrocortisone gel: Application of hydrocortisone gel to reduce inflammation and promote tissue healing.
-
–
Hydrogen peroxide: Use of hydrogen peroxide to eliminate bacteria and reduce infection risk.
Antibiotics
In cases where infection is suspected, antibiotics may be prescribed to manage bacterial growth and promote healing. However, antibiotics should be used judiciously, as overuse can lead to bacterial resistance.
The following are examples of antibiotics commonly used:
-
–
Metronidazole: An effective antibiotic in managing anaerobic bacterial infections.
-
–
Cephalexin: A broad-spectrum antibiotic useful in treating dry socket associated with bacterial infections.
Pain Management
Pain management plays a crucial role in treating dry socket. Various pain relief strategies can be employed, including the use of analgesics, anesthetics, and topical agents.
For example:
-
–
Analgesics: Over-the-counter pain relievers such as ibuprofen or acetaminophen can help manage mild pain.
-
–
Anesthetics: Local anesthetics, such as lidocaine or benzocaine, can provide temporary pain relief.
-
–
Topical agents: The use of topical capsaicin cream or benzocaine gel can help reduce pain and inflammation.
Palliative Care
Palliative care focuses on alleviating the symptoms and stress of a serious illness, such as dry socket. By addressing the patient’s physical, emotional, and social needs, palliative care can improve the quality of life.
For instance:
–
Palliative care can involve psychological support to help manage anxiety and depression associated with dry socket.
–
Pain management strategies are integrated with palliative care to ensure effective pain relief.
Real-life examples of successful treatment for dry socket include patients who have undergone debridement and received antibiotics to manage infection, leading to complete recovery. Additionally, patients who have received palliative care have reported significant improvements in their overall well-being.
Coping with Dry Socket
Coping with dry socket can be a challenging and emotionally taxing experience. The pain and discomfort associated with dry socket can be severe, leading to anxiety and stress. It’s essential to address the emotional and mental aspects of dry socket to ensure a smooth recovery.
The Emotional Toll of Dry Socket
The emotional impact of dry socket can be significant, affecting not only the individual but also their loved ones. Dry socket can lead to feelings of frustration, anger, and despair, particularly if the pain and discomfort persist for an extended period. The emotional toll of dry socket can manifest in various ways, including:
- Anxiety and stress: The constant pain and discomfort associated with dry socket can create a sense of unease and anxiety, making it challenging to perform daily activities.
- Frustration and anger: The prolonged period of discomfort and pain can lead to feelings of frustration and anger, particularly if the individual believes that the dry socket could have been prevented.
- Depression: The emotional toll of dry socket can also contribute to feelings of depression, particularly if the individual feels overwhelmed and helpless in managing their pain and discomfort.
Cognitive-Behavioral Therapy (CBT) for Dry Socket
Cognitive-behavioral therapy (CBT) is a type of therapy that can be beneficial in managing anxiety and stress related to dry socket. CBT focuses on identifying and challenging negative thought patterns and behaviors that contribute to the individual’s emotional distress. By addressing these underlying issues, CBT can help individuals develop more adaptive coping mechanisms and improve their overall mental well-being. Some of the benefits of CBT for dry socket include:
- Reducing anxiety and stress: CBT can help individuals develop coping strategies to manage their anxiety and stress related to dry socket.
- Improving mood: By addressing underlying thought patterns and behaviors, CBT can help individuals improve their mood and reduce symptoms of depression.
- Enhancing self-efficacy: CBT can help individuals develop a sense of control and confidence in managing their pain and discomfort, which can enhance their overall quality of life.
The Importance of Social Support
Social support is crucial in coping with dry socket and promoting overall well-being. Social support can come in various forms, including:
- Family and friends: Having a strong support system of family and friends can provide emotional support, practical help, and reassurance during the recovery period.
- Support groups: Joining a support group can provide individuals with a sense of community and connection with others who are experiencing similar challenges.
- Healthcare professionals: Healthcare professionals, including dentists and dental hygienists, can provide essential emotional support and guidance throughout the recovery process.
Concluding Remarks
Dry socket how long does it take to heal is a query that many individuals pose after experiencing this painful complication. As we’ve navigated this enthralling narrative, we’ve uncovered the complexities of dry socket, its causes, and the effective strategies for managing pain and discomfort. Remember, a comprehensive understanding of dry socket can empower you to take proactive steps towards healing and ensuring that you don’t experience this complication in the future.
Essential Questionnaire
Q: Is dry socket a common complication of tooth extraction?
A: Yes, dry socket is a common complication of tooth extraction, affecting approximately 2-5% of patients. Its occurrence is often linked to poor oral hygiene, smoking, and certain medications.
Q: Can dry socket be prevented?
A: Yes, dry socket can be prevented by following proper post-extraction care instructions, maintaining good oral hygiene, and refraining from smoking and consuming certain foods and drinks. Consult your dentist or oral surgeon for tailored advice on preventing dry socket.
Q: How long does it take for a dry socket to heal?
A: The healing time for a dry socket can vary depending on the severity of the condition, the effectiveness of treatment, and individual factors. On average, dry socket can take 7-14 days to heal. However, some cases may require prolonged treatment and healing times.
Q: Are dry socket symptoms severe enough to warrant emergency attention?
A: In severe cases, dry socket symptoms can be debilitating and warrant emergency attention. If you’re experiencing intense pain, difficulty speaking or eating, or if you suspect you have a severe dry socket, contact your dentist or oral surgeon immediately for assistance.
