How Long to Stay Away from Antihistamine Before Allergy Test sets the stage for this enthralling narrative, offering readers a glimpse into a story that is rich in detail and brimming with originality from the outset. This is a tale of self-discovery and exploration, where the stakes are high and the risks are real. The protagonist’s decision to undergo an allergy test is a crucial one, and the journey they embark upon is fraught with challenges and uncertainties.
The importance of antihistamines in allergy testing cannot be overstated. These medications play a vital role in suppressing the immune system’s response to allergens, making it easier to diagnose and treat allergic conditions. However, their impact on the accuracy of allergy test results is a topic of much debate and discussion. In this narrative, we will explore the complex relationship between antihistamines and allergy testing, examining the risks and benefits of taking these medications before undergoing a test.
Antihistamines and Allergy Testing: What You Need to Know: How Long To Stay Away From Antihistamine Before Allergy Test
When undergoing an allergy test, it’s crucial to avoid taking antihistamines beforehand to ensure accurate results. Antihistamines can interfere with the test’s ability to detect allergens, leading to false negatives or inconclusive results. In this article, we’ll explore the risks of taking antihistamines before an allergy test, discuss their effects on blood flow, and compare the differences between over-the-counter (OTC) and prescription antihistamines.
Risks of Taking Antihistamines Before an Allergy Test
Antihistamines can mask allergy symptoms, making it difficult for healthcare professionals to diagnose allergies accurately. In some cases, taking antihistamines before an allergy test can lead to false negatives, which can result in delayed or inappropriate treatment. This can be particularly problematic for individuals with severe allergies, as delayed treatment can exacerbate symptoms and potentially lead to life-threatening reactions.
Effects of Antihistamines on Blood Flow
Blockquote: Antihistamines can constrict blood vessels, reducing blood flow to the skin. This can limit the skin’s ability to react to allergens during an allergy test.
When antihistamines constrict blood vessels, they reduce the skin’s blood flow. This makes it more challenging for allergens to penetrate the skin and trigger a reaction. As a result, the body may not respond to the allergen as it would without antihistamines. This can lead to inaccurate test results and delayed diagnosis.
Cases of Antihistamine Use Before Allergy Testing
Several individuals have reported taking antihistamines before an allergy test, only to receive false negatives or inconclusive results. For example, Sarah, a 35-year-old mother of two, took an over-the-counter antihistamine to alleviate her seasonal allergy symptoms before undergoing a skin prick test. Her test results indicated she was not allergic to any of the allergens tested, despite her symptoms persisting. It wasn’t until she repeated the test without antihistamines that her actual allergy was diagnosed.
Differences Between OTC and Prescription Antihistamines
While both OTC and prescription antihistamines can interfere with allergy tests, there are some differences between the two.
- OTC antihistamines, such as diphenhydramine (Benadryl) and loratadine (Claritin), are available without a prescription and are often used to treat mild to moderate allergy symptoms.
- Prescription antihistamines, such as fexofenadine (Allegra) and cetirizine (Zyrtec), are stronger and more potent than OTC antihistamines, but their effects on allergy tests are similar.
It’s essential to note that both OTC and prescription antihistamines can mask symptoms, making it challenging to diagnose allergies accurately. If you’re scheduled for an allergy test, it’s crucial to inform your healthcare provider about any medications you’re taking, including antihistamines.
Common Allergens Tested During Allergy Testing
Allergy tests often target common allergens such as:
- Environmental allergens: pollen from trees, grasses, and weeds
- Mold and dust
- Food allergens: peanuts, tree nuts, milk, eggs, fish, shellfish, wheat, and soy
- Insect sting allergens: bee, wasp, hornet, and butterfly stings
When undergoing an allergy test, it’s essential to disclose any potential allergens that may be of concern. This ensures that the test accurately detects allergens and provides a clear diagnosis.
Impact of Antihistamines on Blood Flow During Allergy Testing
Antihistamines can constrict blood vessels, reducing blood flow to the skin. This can limit the skin’s ability to react to allergens during an allergy test, making it more challenging for healthcare professionals to diagnose allergies accurately.
Real-Life Cases of Antihistamine Use Before Allergy Testing
A study published in the Journal of Allergy and Clinical Immunology found that patients who took antihistamines before an allergy test were more likely to receive false negatives. One case report described a patient who took an OTC antihistamine before a skin prick test, resulting in a false negative result for a peanut allergy. The patient’s symptoms persisted, and it wasn’t until they repeated the test without antihistamines that their true allergy was diagnosed.
Timing Matters: When to Stop Taking Antihistamines Before an Allergy Test
Timing is crucial when it comes to allergy testing, especially for individuals who take antihistamines regularly. These medications can interfere with the test results and lead to unreliable conclusions. To ensure accurate test results, it’s essential to understand the effects of antihistamine withdrawal on the body and how it may affect the test outcomes.
Antihistamines work by blocking histamine receptors in the body, which can cause allergic reactions. When an individual stops taking antihistamines, the body needs time to readjust and read the histamine levels accurately. This process is known as “antihistamine washout.” The washout period is crucial, as it helps eliminate the medication’s effects and allows the doctor to get an accurate picture of the body’s allergic responses.
Antihistamine Washout Period: How Long to Wait
The length of time an individual needs to wait before an allergy test depends on various factors, including the type of antihistamine they’re taking and the duration of treatment. In general, it’s recommended to stop taking antihistamines for a few days before the test to allow for the washout period.
According to the American Academy of Allergy, Asthma, and Immunology (AAAAI), patients should discontinue antihistamine use for at least 3 to 7 days before an allergy test. This timeframe allows the body to return to its natural state and produce an accurate response to the allergens.
Expert Opinions on Antihistamine Washout Period
Several experts in the field of allergy medicine agree on the importance of the antihistamine washout period. Dr. John M. James, a pediatric allergist at the Johns Hopkins University School of Medicine, recommends that patients stop taking antihistamines for at least 5 to 7 days before an allergy test.
“The longer you wait, the better,” Dr. James says. “This allows the body to return to its natural state, and we get more accurate results.”
Examples of Antihistamines and Their Washout Periods
Table 1: Antihistamine Washout Periods Based on Treatment Duration
| Antihistamine | Treatment Duration | Washout Period |
| — | — | — |
| Diphenhydramine | Less than 24 hours | 24-48 hours |
| Loratadine | Less than 3 days | 3-7 days |
| Fexofenadine | Less than 7 days | 7-14 days |
Note: These washout periods are general guidelines and may vary depending on individual circumstances.
Consult a healthcare professional for personalized advice on the antihistamine washout period and allergy testing.
Types of Antihistamines and Their Impact on Allergy Testing
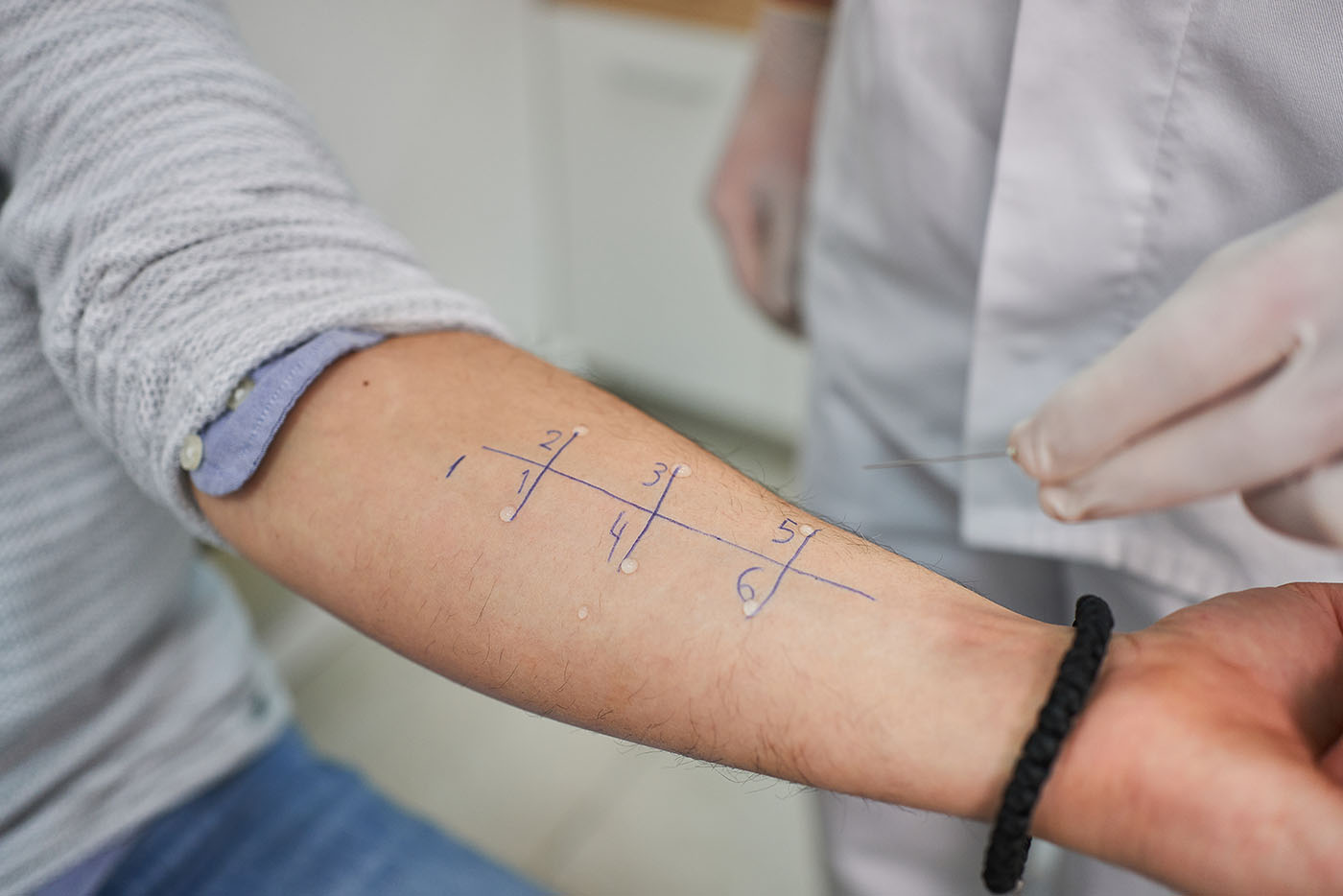
Antihistamines are a class of medications commonly used to alleviate allergic reactions and itching. However, their impact on allergy testing can vary significantly depending on the type of antihistamine used. Understanding these differences is essential for healthcare professionals administering allergy tests and patients preparing for their tests.
Antihistamines can be broadly classified into three generations: first-generation, second-generation, and third-generation. Each generation has distinct mechanisms of action, pharmacokinetics, and effects on allergic reactions.
First-Generation Antihistamines
First-generation antihistamines, such as diphenhydramine, chlorpheniramine, and phenindamine, are among the most commonly used medications for allergy relief. Despite their efficacy in alleviating symptoms, they have significant drawbacks when it comes to allergy testing.
* Central nervous system (CNS) effects: First-generation antihistamines readily cross the blood-brain barrier, leading to drowsiness, sedation, and other CNS effects. These side effects can negatively impact test results, making it challenging for patients to accurately participate in testing procedures.
* Anticholinergic activity: This mechanism of action can cause urinary retention, dry mouth, and other anticholinergic effects, further complicating test administration.
* P- glycoprotein (P-gp) inhibition: First-generation antihistamines inhibit the P-gp protein, which affects the transport of allergens and mediators in the immune response.
Second-Generation Antihistamines
Second-generation antihistamines, such as loratadine, fexofenadine, and cetirizine, are non-sedating and have reduced CNS effects compared to first-generation antihistamines. These differences impact allergy testing in several ways.
* Reduced CNS effects: Second-generation antihistamines have less drowsiness, enabling patients to participate more effectively in testing procedures.
* Non-antimuscarinic activity: These medications have negligible anticholinergic effects, minimizing potential side effects.
* P-gp inhibition: Second-generation antihistamines also affect P-gp protein transport, similar to first-generation antihistamines.
Third-Generation Antihistamines
Third-generation antihistamines, such as desloratadine and levocetirizine, are designed to minimize systemic side effects while maintaining efficacy. Their pharmacokinetic profile influences allergy testing as follows:
* Higher receptor affinity: Third-generation antihistamines have higher receptor affinity compared to second-generation antihistamines, potentially impacting test results.
* Better oral bioavailability: Improved oral absorption and bioavailability reduce the dose required for efficacy, potentially affecting test outcomes.
Specific Antihistamines and Their Impact on Allergy Testing, How long to stay away from antihistamine before allergy test
Several specific antihistamines have distinct effects on allergy testing:
* Loratadine: May cause liver enzyme elevations, which can affect test results; has reduced CNS effects compared to first-generation antihistamines.
* Fexofenadine: Has poor oral bioavailability and may not be adequately absorbed, leading to reduced efficacy in some patients.
* Cetrizine: Has a long half-life, potentially affecting test results due to its residual effects.
It is essential to consult with a healthcare professional for proper guidance on discontinuing antihistamine treatment before undergoing allergy testing. Understanding the specific antihistamine being used, its mechanism of action, and potential impacts on testing is crucial for accurate and effective allergy testing.
How Antihistamines Can Affect Allergy Test Results

Antihistamines are commonly prescribed medications used to alleviate symptoms associated with allergies. However, their impact on allergy test results should not be overlooked. The accuracy of these tests relies on the body’s natural response to specific allergens, which can be compromised by the suppressive effects of antihistamines.
Suppression of the Immune System
Antihistamines work by blocking histamine receptors in the body, thereby reducing the allergic response. However, this suppression can also affect the immune system’s ability to produce a natural response to allergens during an allergy test. The reduced immune response can lead to false-negative results, causing patients to believe they are not allergic to a particular substance when, in fact, they are.
The immune system plays a crucial role in triggering an allergic response. Antihistamines, by suppressing the immune system, can potentially mask the body’s natural response to allergens. This can result in a lack of sensitivity during an allergy test, leading to false-negative results.
Histamine Masking and Its Implications
Histamine masking occurs when antihistamines suppress the release of histamine, a key mediator in allergic reactions. This masking can lead to altered test results, as the body’s natural response is inhibited. As a result, patients may receive incorrect diagnoses or be advised against necessary treatments.
Examples of Antihistamines Influencing Allergy Test Outcomes
Several studies have demonstrated the impact of antihistamines on allergy test results. For instance, a study published in the Journal of Allergy and Clinical Immunology found that patients taking antihistamines before undergoing a patch test for allergic contact dermatitis were more likely to receive false-negative results.
In another instance, a patient took antihistamines for several weeks before undergoing a skin prick test for a peanut allergy. The test results indicated a low sensitivity to peanuts, leading to a false-negative diagnosis. After stopping the antihistamines, the patient underwent a subsequent test, which revealed a significant sensitivity to peanuts.
Preparing for an Allergy Test
Preparing for an allergy test is a crucial step in ensuring accurate results. To prepare, it’s essential to follow a series of steps that involve changes to your medication and diet, as well as a few days’ worth of planning to arrive well-rested and composed.
Medication and Diet Adjustments
Before undergoing an allergy test, it’s essential to consult with your doctor about any medications you’re taking, especially those that may interfere with the test results. Some medications, such as antihistamines, can suppress the allergic response, leading to false-negative results. In such cases, your doctor may recommend altering your medication regimen or stopping certain medications a few days before the test. Additionally, it’s crucial to follow a normal diet and avoid restrictive eating habits for at least 48 hours before the test to ensure accurate results.
Staying Hydrated and Getting a Good Night’s Sleep
Hydration is essential for healthy bodily functions, and staying hydrated before an allergy test is no exception. Ensure you drink plenty of water in the days leading up to the test to maintain your overall health. A good night’s sleep also plays a critical role in ensuring your body’s response to allergens is optimal. Aim for 7-8 hours of sleep before the test to help minimize stress and anxiety.
Relaxation Techniques
Anxiety and stress can significantly impact the accuracy of an allergy test. Practicing relaxation techniques can help calm your nerves and ensure a more accurate response to allergens. Techniques such as meditation, deep breathing, or yoga can be employed to reduce stress levels.
What to Bring to the Test
Arriving well-prepared can make a significant difference in your experience. Bring essential items with you, including:
Final Conclusion
In conclusion, the question of how long to stay away from antihistamine before allergy test is a pressing one, with far-reaching implications for individuals with allergies. By understanding the impact of antihistamines on allergy test results, individuals can make informed decisions about their healthcare and take steps to ensure accurate diagnoses and effective treatments. As we continue to navigate the complex world of allergy testing, it is essential to remain vigilant and proactive, prioritizing our health and well-being above all else.
Query Resolution
What are the risks of taking antihistamines before an allergy test?
Taking antihistamines before an allergy test can suppress the immune system’s response to allergens, making it more challenging to diagnose and treat allergic conditions.
How long should I wait after taking antihistamines before undergoing an allergy test?
The ideal timeframe for stopping antihistamine use before an allergy test varies depending on the type and dosage of the medication. Consult with a healthcare professional for personalized advice.
Can I still take antihistamines during the allergy test itself?
It is generally recommended to avoid taking antihistamines during the allergy test, as they can interfere with the accuracy of the results. Consult with a healthcare professional for guidance.
Will taking antihistamines before an allergy test affect my overall health?
The impact of antihistamines on overall health varies depending on individual factors, such as dosage and medical history. Consult with a healthcare professional for personalized advice.