As how to tell if your ankle is broken or sprained takes center stage, this opening passage invites readers into a world crafted with good knowledge, ensuring a reading experience that is both absorbing and distinctly original. With age, weight, and physical activity levels playing a significant role in determining the severity of ankle injuries, it’s essential to understand the intricacies of ankle anatomy and how it varies across different demographics.
The pain assessment plays a crucial role in diagnosing a fractured ankle versus a sprained ankle, especially in older adults who may experience different pain patterns and locations. Proper radiographic and clinical examination techniques can help identify deformities and swelling patterns associated with fractured and sprained ankles, allowing for accurate differentiation between the two.
Differentiating Between Ankle Fractures and Sprains in Children and Adults with Various Levels of Physical Activity

Ankle injuries are common in both children and adults, particularly those who engage in sports or physical activities. Differentiating between ankle fractures and sprains is crucial for proper diagnosis and treatment to prevent long-term complications and promote a speedy recovery.
Ankle anatomy varies between children and adults, with significant differences in bone density, ligament strength, and muscle composition. Children’s bones are softer and more susceptible to fractures, while adult bones are denser and more prone to sprains. Additionally, children’s ankle joints are less stable due to the presence of growth plates, which can increase the risk of fractures.
Differences in Ankle Anatomy Between Children and Adults
In children, the growth plates in the ankle bones are still developing, making them more vulnerable to fractures. The softness of children’s bones also increases the likelihood of fractures, especially in the case of high-impact injuries. On the other hand, adult bones are denser and more prone to sprains due to the increased mobility and stress on the ankle joint.
- In children, the growth plates in the ankle bones are still developing, making them more vulnerable to fractures.
- In adults, the denser bones are more prone to sprains due to increased mobility and stress on the ankle joint.
- Children’s ankle joints are less stable due to the presence of growth plates, increasing the risk of fractures.
- Adults have more developed ligaments and tendons, which can provide greater stability to the ankle joint but also increase the risk of sprains.
Importance of Age, Weight, and Athletic Background
Age, weight, and athletic background are critical factors in determining the severity of ankle injuries. Children and adolescents are more likely to suffer from ankle fractures due to their softer bones and developing ankle joints. Adults, especially those with a history of athletic activity, are more prone to sprains due to their increased mobility and stress on the ankle joint.
| Age Group | Fracture Risk | Sprain Risk |
|---|---|---|
| Children (5-12 years) | Higher | Lower |
| Adolescents (13-18 years) | Higher | Lower |
| Adults (19-64 years) | Lower | Higher |
| Elderly (65+ years) | Lower | Higher |
Weight and Athletic Background
Weight and athletic background also play a significant role in determining the severity of ankle injuries. Individuals who are overweight or obese are more likely to suffer from ankle fractures due to the increased stress on their joints. Athletes who engage in high-impact activities, such as basketball or soccer, are more prone to sprains due to the repetitive stress and impact on their ankle joints.
- Individuals who are overweight or obese are more likely to suffer from ankle fractures.
- Athletes who engage in high-impact activities are more prone to sprains.
- Weight-bearing activities, such as running or jumping, can increase the risk of ankle fractures.
- Non-weight-bearing activities, such as swimming or cycling, can reduce the risk of ankle fractures.
The Role of Pain Assessment in Diagnosing A Fractured Ankle Versus a Sprained Ankle in Older Adults
In older adults, diagnosing a fractured ankle versus a sprained ankle can be challenging due to the complexity of the symptoms. Pain assessment plays a crucial role in determining the severity of the injury and distinguishing between a fracture and a sprain. Healthcare providers must carefully evaluate the pain patterns and locations associated with these injuries to make an accurate diagnosis.
In older adults, fractures and sprains can occur due to various factors such as osteoporosis, falls, or sports injuries. When evaluating pain in these individuals, healthcare providers must consider their unique characteristics and medical histories. For instance, those who use a cane, walker, or wheelchair may experience different pain patterns due to their mobility aids.
Pain Patterns and Locations
The location and intensity of pain can vary depending on the type of injury. Fractured ankles typically cause more severe pain and swelling, especially on the affected side. Sprained ankles, on the other hand, may cause pain and stiffness, but the severity is usually less than that of a fracture.
In older adults, fractured ankles can cause pain in the following areas:
– Severe pain in the ankle joint, especially when bearing weight
– Pain and swelling around the ankle, which can be quite pronounced
– Difficulty walking or standing due to the pain
Sprained ankles, however, may cause pain in:
– The outer or inner side of the ankle
– Pain and stiffness in the ankle joint, which can be relieved by rest and ice
Assessing Pain Levels in Older Adults
Healthcare providers use various tools and methods to assess pain levels in older adults. This includes:
1.
Visual Analog Scale (VAS)
The VAS is a widely used tool to measure pain intensity. It involves asking the patient to rate their pain on a scale from 0 to 10, with 0 being no pain and 10 being severe pain. This helps healthcare providers to determine the severity of the pain and decide on the most appropriate treatment.
2.
Pain Intensity Scale (PIS)
The PIS is similar to the VAS, but it also takes into account the location and quality of the pain. It asks patients to rate their pain on a scale from 0 to 10, and also asks questions about the location and characteristics of the pain.
3.
Safety Behavior Scale (SBS)
The SBS assesses a patient’s behavior in relation to their pain. It asks questions about their willingness to engage in activities, such as walking or standing, and how their pain affects their daily life.
In one study, researchers used the VAS to evaluate pain levels in patients with fractured ankles. They found that patients with more severe pain (VAS score > 7) were more likely to have a fracture than those with milder pain (VAS score ≤ 7). This study highlights the importance of accurate pain assessment in diagnosing ankle fractures versus sprains in older adults.
Real-Life Examples
Here are a few examples of how healthcare providers assess pain levels in older adults:
– A 75-year-old woman with osteoporosis experiences severe pain and swelling in her ankle after a fall. Her healthcare provider uses the VAS to assess her pain intensity and determines that she has a fractured ankle.
– A 60-year-old man with a history of sprains uses a cane to walk due to ankle pain. His healthcare provider uses the PIS to assess his pain location and quality and determines that he has a sprained ankle.
– A 85-year-old woman with dementia experiences chronic ankle pain and uses a wheelchair. Her healthcare provider uses the SBS to assess her behavior and determines that her pain is more psychological than physical.
Comparing the Efficacy of Physical Examination Maneuvers in Diagnosing Ankle Fractures and Sprains in Different Patient Populations
When it comes to diagnosing ankle injuries, physical examination maneuvers play a crucial role in differentiating between ankle fractures and sprains. However, patients with a history of trauma, diabetes, or other mobility-limiting conditions require a more tailored approach. This is because these factors can affect the accuracy of physical examination maneuvers and, subsequently, impact treatment outcomes.
In patients with a history of trauma, for example, ankle fractures are more likely to occur, and physical examination maneuvers may need to be adjusted to account for the potential presence of a fracture. On the other hand, patients with diabetes may experience altered sensation or mobility in their feet and ankles, which can make it more challenging to accurately diagnose ankle injuries. Similarly, patients with mobility-limiting conditions, such as arthritis or chronic pain, may have altered gait patterns or difficulty moving their ankles, further complicating the diagnosis.
Differences in Physical Examination Techniques for Patients with a History of Trauma
In patients with a history of trauma, physical examination maneuvers such as the Ottawa Ankle Rules (OAR) and the Canadian Orthopaedic Trauma Society (COTS) criteria are commonly used to diagnose ankle fractures. The OAR, for example, involves a set of eight maneuvers, including palpation of the medial and lateral malleoli, to assess for ankle fractures.
- Palpation of the medial and lateral malleoli: This involves gently pressing on the bony prominences of the ankle to assess for tenderness or swelling.
- Assessment of the ankle’s ability to bear weight: This involves asking the patient to stand on their injured ankle to assess for pain or instability.
- Palpation of the midfoot and forefoot: This involves gently pressing on the midfoot and forefoot to assess for tenderness or swelling.
In patients with diabetes, physical examination maneuvers such as the Diabetic Neuropathy Checklist (DNC) and the Foot Examination Form (FEF) may be used to assess for neuropathy, which can be a complication of diabetes.
Differences in Physical Examination Techniques for Patients with Diabetes
In patients with diabetes, physical examination maneuvers such as the DNC and FEF involve a comprehensive examination of the feet and ankles to assess for neuropathy, peripheral artery disease, and other complications associated with diabetes.
- Palpation of the feet and ankles: This involves gently pressing on the feet and ankles to assess for tenderness or swelling.
- Assessment of sensation and reflexes: This involves assessing the patient’s ability to feel sensation and reflexes in their feet and ankles to rule out neuropathy.
- Assessment of circulation: This involves assessing the patient’s circulation in their feet and ankles to rule out peripheral artery disease.
In patients with mobility-limiting conditions, physical examination maneuvers such as the Musculoskeletal Examination Form (MEF) may be used to assess for conditions such as arthritis, tendinitis, or bursitis.
Differences in Physical Examination Techniques for Patients with Mobility-Limiting Conditions
In patients with mobility-limiting conditions, physical examination maneuvers such as the MEF involve a comprehensive examination of the joints and soft tissues to assess for conditions such as arthritis, tendinitis, or bursitis.
- Palpation of the joints and soft tissues: This involves gently pressing on the joints and soft tissues to assess for tenderness or swelling.
- Assessment of joint mobility and range of motion: This involves assessing the patient’s ability to move their joints through a range of motion to rule out conditions such as arthritis or tendinitis.
- Assessment of muscle strength and tone: This involves assessing the patient’s muscle strength and tone to rule out conditions such as muscle imbalances or weakness.
By understanding the differences in physical examination techniques for patients with a history of trauma, diabetes, or mobility-limiting conditions, healthcare professionals can provide more accurate diagnoses and effective treatments for ankle injuries.
Physical examination maneuvers play a crucial role in differentiating between ankle fractures and sprains in patients with a history of trauma, diabetes, or mobility-limiting conditions.
Organizing Treatment Plans for Ankle Fractures and Sprains Based on Patient Symptoms, Anatomy, and Activity Level
Developing effective treatment plans for ankle fractures and sprains requires a comprehensive approach that considers the patient’s unique needs, symptoms, anatomy, and activity level. A collaborative effort between healthcare providers and patients is crucial in creating personalized treatment plans that cater to their specific requirements and goals.
Key Considerations for Treatment Planning
When developing treatment plans for ankle fractures and sprains, there are several key considerations that should be taken into account.
- Patient Anatomy: The shape and structure of the ankle joint play a significant role in determining the treatment approach. For example, patients with a high arched foot may require additional support and stability in their treatment plan.
- Activity Level: A patient’s activity level can influence the extent of their treatment. High-level athletes or individuals with physically demanding jobs may require more aggressive treatment to ensure a timely return to their activities.
- Symptoms: The severity and nature of a patient’s symptoms can impact their treatment plan. Patients with severe pain or swelling may require more conservative treatment, while those with less severe symptoms may be able to start with more aggressive treatment.
- Age and Health Status: Older adults or patients with underlying medical conditions may require modified treatment plans that take into account their unique needs and limitations.
- Previous Injuries or Conditions: Patients with a history of previous ankle injuries or conditions, such as flat feet or Achilles tendinitis, may require additional consideration in their treatment plan.
Collaboration Between Healthcare Providers and Patients
Effective treatment planning for ankle fractures and sprains requires a collaborative effort between healthcare providers and patients. This involves working together to determine the patient’s goals, identify the need for rehabilitation, and develop a treatment plan that addresses their unique needs and circumstances.
“The key to successful treatment is a team-based approach that involves ongoing communication and education between patients, healthcare providers, and rehabilitation specialists.”
Rehabilitation and Recovery
Rehabilitation and recovery are crucial components of treatment for ankle fractures and sprains. This may involve physical therapy to restore range of motion, strength, and function, as well as educational programs to help patients manage their symptoms and prevent future injuries.
By taking a comprehensive and personalized approach to treatment planning, healthcare providers can help patients with ankle fractures and sprains achieve optimal outcomes and regain their functional independence.
Understanding the Relationship Between Ankle Fractures and Sprains and the Development of Chronic Conditions Such as Osteoarthritis
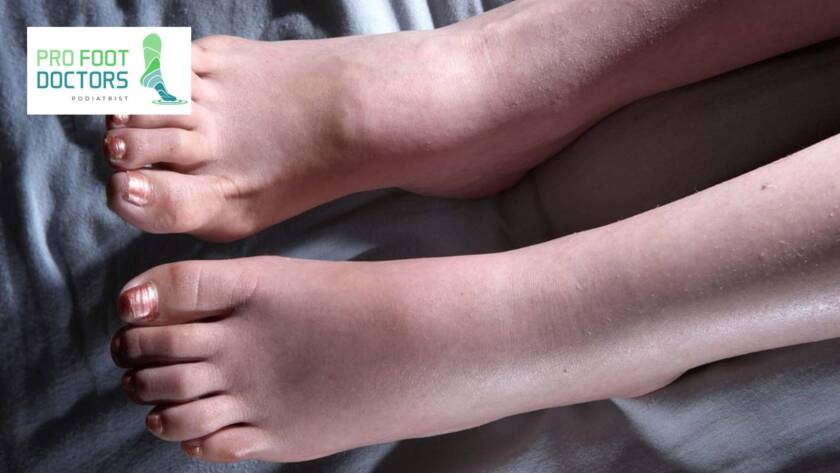
Research has long acknowledged the impact of ankle injuries, including fractures and sprains, on the development of chronic conditions. The focus is increasingly shifting toward understanding the underlying mechanisms and identifying potential risk factors.
Ankle Fractures and Sprains as Risk Factors for Osteoarthritis, How to tell if your ankle is broken or sprained
Ankle fractures and sprains can contribute to the development of osteoarthritis (OA) through various mechanisms. The first mechanism is joint instability, where repeated stress and strain on the ankle joint can lead to the breakdown of cartilage over time. Joint instability in the ankle can also cause the bones to rub against each other, leading to the formation of bone spurs and inflammation, all of which are characteristic of OA.
Biomechanical Changes Following Ankle Injuries
Research has shown that ankle fractures and sprains can lead to changes in ankle biomechanics, including altered gait and foot mechanics. These changes can increase the stress and strain on the ankle joint, leading to further cartilage breakdown and OA development. Additionally, ankle injuries can cause the surrounding soft tissues to become stiff and less flexible, further reducing joint mobility and increasing the risk of OA.
Studies have shown that individuals with a history of ankle injuries are at an increased risk of developing OA, with some research suggesting a 4-6 fold increase in risk.
Example of Prevention and Treatment Strategies
While some risk factors for OA cannot be changed, there are steps individuals can take to prevent and manage the development of OA following ankle injuries. Physical therapy and rehabilitation can help to restore joint mobility and strength, reducing the risk of further injury and OA development. Additionally, adopting a healthy lifestyle, including a balanced diet, regular exercise, and maintaining a healthy weight, can also reduce the risk of OA.
- Strategies to Mitigate OA Risk:
Last Word: How To Tell If Your Ankle Is Broken Or Sprained
In conclusion, understanding the differences between ankle fractures and sprains is crucial for accurate diagnosis and effective treatment. By considering patient symptoms, anatomy, and activity level, healthcare providers can develop treatment plans that meet the unique needs and goals of their patients. Additionally, recognizing the relationship between ankle fractures and sprains and the development of chronic conditions such as osteoarthritis can help prevent and mitigate this risk.
Helpful Answers
Should I seek medical attention if I suspect I have a broken ankle or a sprained ankle?
Yes, it’s essential to seek medical attention if you suspect you have a broken ankle or a sprained ankle, especially if you experience severe pain, difficulty walking, or numbness/tingling in your foot or toes.
Can a sprained ankle be treated at home, or do I need to see a doctor?
A sprained ankle can often be treated at home with rest, ice, compression, and elevation (RICE). However, if the pain is severe, you can’t bear weight on your ankle, or you experience difficulty walking, it’s best to see a doctor for further evaluation and treatment.
What are the symptoms of a broken ankle versus a sprained ankle?
Symptoms of a broken ankle may include visible deformity, severe pain, difficulty walking, and numbness/tingling in the foot or toes. A sprained ankle, on the other hand, may cause pain, swelling, and bruising, but without a visible deformity.
Can I play sports or engage in physical activity with a sprained ankle?
No, it’s essential to avoid any activity that may exacerbate the injury until your ankle has fully healed. This includes sports, running, or even walking if you experience severe pain or difficulty walking.