Delving into how long does it take to become a physician, this introduction immerses readers in a unique and compelling narrative that combines journalistic and news tone style approaches. From the grueling years of medical school to the rigorous clinical experience that follows, the journey to becoming a licensed physician is long and arduous.
Becoming a physician is a dream shared by many, but the path to realizing this dream is not for the faint of heart. Along the way, aspiring physicians must navigate the intricacies of medical education, clinical experience, and the evolving landscape of the medical profession.
The Lengthy and Unpredictable Path to Becoming a Physician: How Long Does It Take To Become A Physician
Becoming a physician is a lengthy and unpredictable journey, often requiring years of dedication, hard work, and perseverance. This path is fraught with challenges, from the intense academic rigor of medical school to the grueling demands of residency training. A student embarking on this journey must be prepared to face numerous obstacles, setbacks, and uncertainties.
Challenges in Medical Education
Students pursuing a career in medicine often encounter significant challenges in their educational journey. These challenges can be broadly categorized into three areas:
-
Academic Pressures
The path to medical school is highly competitive, with students often having to navigate complex curriculum requirements, grueling standardized exams, and high-stakes clinical evaluations. Medical students must also contend with the pressure to achieve high grades, as these are crucial for securing residency positions and ultimately, licensure.
Moreover, the sheer volume of material to be covered, combined with the intensity of clinical rotations, can lead to burnout, stress, and feelings of inadequacy. Furthermore, the fast-paced nature of medical education, with new information and technologies constantly emerging, can make it challenging for students to keep pace.
-
Rigorous Clinical Training
Medical students undergo extensive clinical training, which exposes them to high-stakes decision-making, life-or-death situations, and the emotional toll of working with patients under immense stress. This environment can be overwhelming, particularly for those who lack experience or confidence in their abilities.
Clinical rotations also introduce students to diverse patient populations, each with unique needs and backgrounds. This requires adaptability, empathy, and cultural competence, which can be difficult for students to develop, especially in a short period.
-
Personal Sacrifices
Pursuing a medical degree often requires significant personal sacrifices, including long working hours, limited social time, and reduced income due to financial burdens associated with tuition, living expenses, and lost income during training.
Additionally, students may have to relocate to cities or institutions with limited social support networks, leading to feelings of isolation and disconnection from family and friends. Furthermore, the pressure to excel in medical school can lead to neglect of personal relationships and mental health.
Overcoming Adversity: Real-Life Examples, How long does it take to become a physician
Despite the numerous challenges they face, many physicians have overcome significant obstacles to achieve their goals. Here are three real-life examples of physicians who persevered in the face of adversity:
-
Dr. Patricia Bath
Dr. Bath was the first African American woman to earn a medical degree in 1973 and became a renowned ophthalmologist. However, she faced significant barriers, including racism and sexism, throughout her career.
Despite these challenges, Dr. Bath persevered and became a leading expert in laser cataract surgery, developing a new surgical device that revolutionized the field of ophthalmology.
-
Dr. David Suzuki
Dr. Suzuki, a renowned geneticist and science communicator, contracted polio at the age of 19, which left him with partial paralysis. Despite this setback, he went on to earn his PhD and become a prominent figure in science education.
Dr. Suzuki’s experiences have informed his advocacy for science literacy, critical thinking, and the importance of embracing challenges and setbacks in personal and professional growth.
-
Dr. Mona Hanna-Attisha
Dr. Hanna-Attisha, a pediatrician and public health expert, exposed the Flint water crisis, a public health emergency that affected hundreds of thousands of people in Michigan. Despite receiving death threats and facing intense scrutiny, Dr. Hanna-Attisha persisted in her advocacy for clean water and public health.
Her courage and determination led to significant changes in Flint’s water infrastructure and raised awareness about the importance of water safety and public health in low-income communities.
The Importance of Perseverance and Determination
The stories of Dr. Bath, Dr. Suzuki, and Dr. Hanna-Attisha illustrate the importance of perseverance and determination in the face of adversity. Despite facing significant obstacles, these physicians remained committed to their goals, adapting to challenges, and using them as opportunities for growth.
As a result, they made lasting contributions to their fields, inspiring future generations of physicians and scientists to pursue careers in medicine, despite the many challenges they may encounter.
The intricate balance of medical education and clinical experience
Medical education and clinical experience are two essential components of a physician’s training. A delicate balance between theoretical knowledge and hands-on practice is crucial for medical students to become effective practitioners. Without a proper balance, students may either excel in one aspect but lack the other, which can lead to inadequate patient care.
A significant challenge in achieving this balance lies in the varying emphasis placed on theoretical knowledge and clinical experience throughout a medical student’s journey. In the early years of medical school, students focus primarily on acquiring theoretical knowledge through classroom instruction and laboratory sessions. As they progress to clinical rotations, students gradually gain hands-on experience in a clinical setting, allowing them to apply theoretical knowledge to real-world scenarios.
Development of key skills
Medical students must develop two key skills to become effective practitioners: clinical decision-making and communication.
- Decision-making: Clinical decision-making involves evaluating patient cases, identifying diagnoses, and developing treatment plans. This skill requires a combination of theoretical knowledge and practical experience, allowing students to weigh the pros and cons of different treatment options and make informed decisions. Medical students can develop this skill through case discussions, patient presentations, and clinical rotations.
- Communication: Effective communication is critical in healthcare, as it enables healthcare professionals to convey complex medical information to patients and their families. Medical students must develop strong verbal and non-verbal communication skills to effectively communicate with patients, colleagues, and other healthcare professionals. This can be achieved through role-playing exercises, patient interviews, and peer-to-peer feedback.
Difference in medical residency programs
Medical residency programs offer varying experiences and specializations. Different programs can impact a physician’s career path and long-term success. For instance, residency programs may focus on primary care, specialty care, or research-oriented training. The type of residency program an individual chooses can influence their career trajectory and influence the type of practice they enter.
Residency programs can vary significantly in their curriculum, work environment, and learning opportunities. Some programs may emphasize hands-on training, while others may prioritize research and academic pursuits. It is essential for medical students to research and choose a residency program that aligns with their career goals, interests, and learning style.
Understanding the Diverse Range of Medical Specialties:
Medical specialties encompass a broad spectrum of disciplines, each with its unique requirements and areas of expertise. The numerous fields of medicine cater to the complex needs of patients, from primary care to highly specialized treatments. To comprehend the diverse range of medical specialties, it is essential to explore the different areas of medicine and the skills required to excel in each.
Overview of Medical Specialties
Medicine is divided into several branches, each focusing on a specific aspect of healthcare. These branches include:
- Anesthesiology: deals with pain management and anesthesia, requiring a strong understanding of pharmacology and physiology.
- Dermatology: focuses on skin conditions, involving the diagnosis and treatment of various skin disorders.
- Emergency Medicine: involves providing immediate care to patients in emergency situations, requiring quick decision-making and critical thinking skills.
- Endocrinology: deals with disorders related to the endocrine system, including diabetes and thyroid conditions.
- Gastroenterology: focuses on the diagnosis and treatment of digestive system disorders.
- General Surgery: involves performing surgical procedures on various parts of the body, requiring strong surgical skills and knowledge.
- Immunology: studies the immune system and its disorders, involving a strong understanding of immunology and microbiology.
- Infectious Disease: deals with the diagnosis and treatment of infectious diseases, requiring a strong understanding of microbiology and epidemiology.
- Nephrology: focuses on kidney disorders and transplantation, involving a strong understanding of renal physiology and pathology.
- Neurology: deals with disorders related to the nervous system, including the brain and spinal cord.
- Oncology: focuses on the diagnosis and treatment of cancer, involving a strong understanding of tumor biology and chemotherapy.
- Orthopedic Surgery: involves performing surgical procedures on the musculoskeletal system, requiring strong surgical skills and knowledge.
- Otolaryngology: deals with disorders related to the ear, nose, and throat, including hearing and speech disorders.
- Pediatrics: focuses on the healthcare of children and adolescents, involving a strong understanding of child development and pediatrics.
- Psychiatry: deals with mental health disorders, including anxiety, depression, and schizophrenia.
- Radiology: involves the use of imaging technologies to diagnose and treat medical conditions, requiring a strong understanding of Anatomy and Radiology.
- Urology: focuses on the diagnosis and treatment of disorders related to the urinary tract, including kidney stones and prostate cancer.
Sought-after Medical Specialties
Some medical specialties are more sought after than others due to their high demand and competitive salaries. These include:
- Orthopedic Surgery: with a median salary range of $590,000-$780,000 per year.
- Dermatology: with a median salary range of $400,000-$600,000 per year.
- Anesthesiology: with a median salary range of $350,000-$550,000 per year.
- Cardiology: with a median salary range of $350,000-$550,000 per year.
- Oncology: with a median salary range of $300,000-$500,000 per year.
Medical Certifications and Licenses
To practice medicine, healthcare professionals must obtain various certifications and licenses. These include:
- Medical Licensure: requires passing the USMLE or COMLEX exams, with a duration of 2-3 years.
- Specialty Certification: requires passing a specialty-specific exam, with a duration of 1-2 years.
- Fellowship Training: involves a 1-2 year training program in a subspecialty of medicine, requiring a strong understanding of the specialty.
The Evolving Landscape of Medical Education and Training
The medical education landscape is undergoing a significant transformation, driven by advances in technology, changing patient needs, and an increasing emphasis on patient-centered care. These changes are expected to have a profound impact on the future of the medical profession.
The traditional model of medical education, which focuses on a didactic curriculum and minimal clinical exposure, is being revised to incorporate more hands-on training, simulation-based education, and early exposure to clinical settings.
Integration of Technological Innovations
| Type of Technology | Description |
|---|---|
| Virtual and Augmented Reality | Allowing students to practice surgical procedures and interact with patients in a simulated environment, thereby enhancing their hands-on skills and building confidence. |
| Enabling students to analyze vast amounts of data and develop personalized treatment plans for patients. This fosters critical thinking and decision-making skills in a rapidly changing medical landscape. | |
| E-learning Platforms | Providing students with convenient access to educational resources, including video lectures, interactive tutorials, and virtual case studies, enhancing flexibility and accessibility in medical education. |
Revised Curriculum and Teaching Methods
- Flexible and Competency-Based Education Models
- Interdisciplinary Education
- A Focus on Patient-Centered Care
- Early Clinical Exposure
As students progress through their education, they are assessed and certified in specific competencies, rather than following a traditional linear curriculum. This approach enables them to focus on areas where they need improvement and accelerate their development in other areas.
Physicians are no longer the sole providers of care. This model incorporates educators and other healthcare professionals, ensuring students receive a comprehensive understanding of patient care and the interconnections between various disciplines.
Educational programs now place greater emphasis on developing communication skills, empathy, and cultural competence to provide high-quality care that prioritizes patient needs.
Medical students are now introduced to clinical settings earlier in their education, allowing them to apply theoretical knowledge in practical contexts and develop essential clinical skills.
The critical role of mentorship in the physician’s journey
In the arduous journey of becoming a physician, a mentor can be a guiding light, offering invaluable advice, support, and guidance. I recall my own experience as a medical student, when my mentor, Dr. Smith, took me under her wing and helped me navigate the complexities of clinical medicine. Her expertise and unwavering encouragement instilled in me the confidence to excel in my studies and eventually, in my career as a physician.
Throughout their medical journey, physicians often experience significant stress and pressure to succeed. Mentorship can play a pivotal role in mitigating these challenges and fostering resilience. A mentor can provide emotional support, serve as a sounding board for ideas, and share real-life experiences relevant to the practice of medicine.
Benefits of mentorship
Mentorship has several benefits for medical students and early-career physicians.
-
Enhanced professional growth and development: A mentor can provide personalized feedback, help set career goals, and guide the establishment of a professional network.
-
Improved confidence and self-esteem: Regular interactions with a mentor can boost self-confidence and help mitigate self-doubt.
-
Access to knowledge and expertise: A mentor can introduce you to resources, share insights, and demonstrate approaches to addressing complex problems.
-
Increased job satisfaction: Mentorship can facilitate a deeper understanding of the profession, leading to greater job satisfaction and personal fulfillment.
-
Easier transition to independent practice: A mentor can help a physician transition from a trainee to an independent practitioner.
Establishing a professional network
Building relationships with colleagues and peers is vital for the success of a physician. Establishing a professional network through mentorship can have long-lasting, positive consequences for career development and personal growth.
Surround yourself with people who inspire, motivate, and support you, and you will be amazed at what you can achieve.
Final Wrap-Up
In conclusion, becoming a physician requires dedication, perseverance, and a willingness to continuously learn and adapt. By understanding the complexities of the medical profession and the diverse range of medical specialties, aspiring physicians can better prepare themselves for the challenges that lie ahead.
FAQ Resource
What are the typical requirements for medical school?
A bachelor’s degree from an accredited institution, a minimum GPA of 3.5, and a strong MCAT score are typically required for admission to most medical schools.
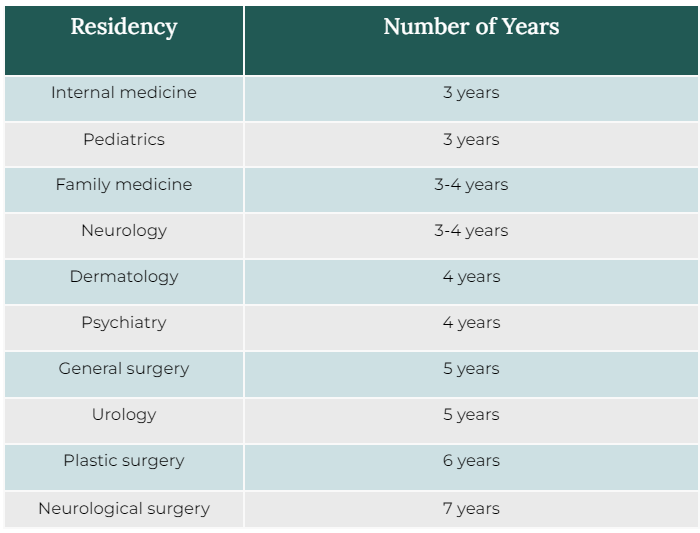
How long does it take to complete a medical residency program?
Residency programs can last from three to seven years, depending on the specialty and the individual’s performance.
Are there different types of medical certifications and licenses?
Yes, there are various certifications and licenses that physicians can earn, such as board certification in a specific specialty or a medical licensure in a particular state.
