Kicking off with how often to take Tylenol, this opening paragraph is designed to captivate and engage the readers, setting them up for a comprehensive journey through the world of pain relief and medication management.
The recommended dosage of Tylenol is a crucial aspect of using this medication effectively and safely. However, many individuals are unclear about how to determine the right dosage for their specific needs, including factors such as age, weight, and medical condition.
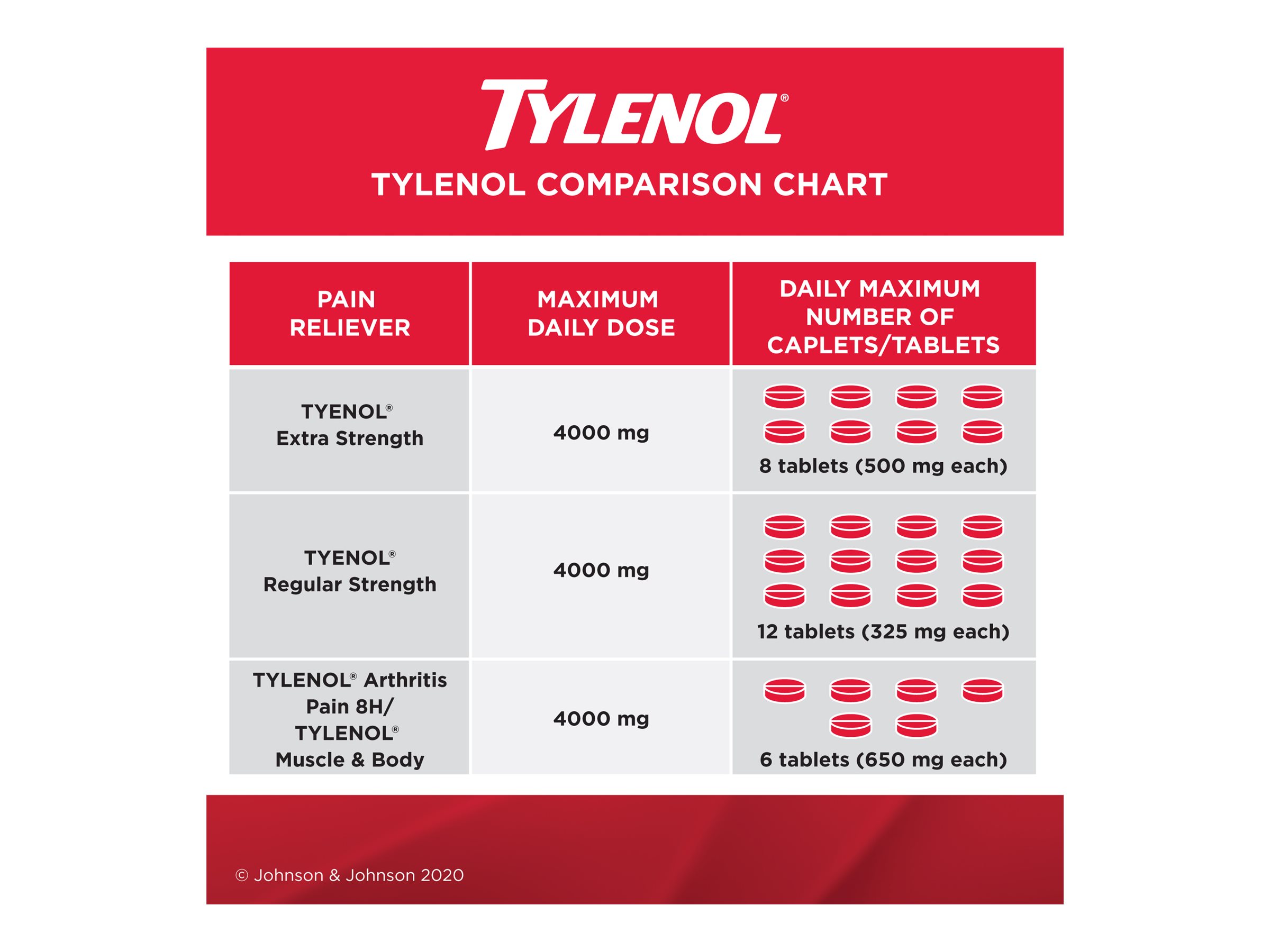
Comparing Tylenol Dosage to Other Pain Relievers
Tylenol, commonly used to alleviate headaches, fever, and minor aches, has a specific dosage recommendation that varies depending on the medical condition, age, and weight of the individual. This comparison highlights the differences in dosage and frequency between Tylenol and other common pain relievers like aspirin and ibuprofen.
Acetaminophen vs. Salicylate vs. Non-Steroidal Anti-Inflammatory Drugs (NSAIDs)
Acetaminophen, the active ingredient in Tylenol, works by reducing fever and relieving pain without decreasing inflammation. In contrast, salicylates, found in aspirin, and NSAIDs, including ibuprofen (Advil, Motrin), both reduce inflammation in addition to relieving pain and decreasing fever. This difference in mechanism of action may affect the choice of pain reliever depending on the condition being treated.
Aspirin and Tylenol Comparison
When it comes to headaches or mild pain, Tylenol is generally recommended over aspirin for people with stomach ulcers or bleeding disorders. However, for conditions like arthritis, where inflammation is a major component, aspirin or NSAIDs may be more suitable.
NSAIDs – Ibuprofen vs. Tylenol Comparison
Ibuprofen, like aspirin, is an NSAID that reduces inflammation, pain, and fever. However, ibuprofen has a lower risk of stomach problems compared to aspirin. It is often preferred for chronic pain or inflammation.
- For individuals with stomach ulcers or bleeding disorders: Tylenol (acetaminophen) may be preferred over aspirin or NSAIDs due to its lower risk of gastrointestinal side effects.
- For patients with arthritis or conditions involving inflammation: Aspirin or NSAIDs may be more suitable due to their anti-inflammatory properties.
- For chronic pain or inflammation: Ibuprofen may be a suitable choice due to its lower risk of stomach problems compared to aspirin.
Understanding the Impact of Tylenol on Children: How Often To Take Tylenol
Tylenol, also known as acetaminophen, is a widely used over-the-counter medication for pain relief and fever reduction in children. However, it’s essential to understand the proper dosage and potential risks associated with its use in children. Improper use of Tylenol can lead to serious health complications, including liver damage and overdose.
When it comes to administering Tylenol to children, the recommended dosage varies depending on the child’s age and weight. The American Academy of Pediatrics (AAP) provides guidelines for the safe use of acetaminophen in children.
Recommended Dosage for Children
According to the AAP, the recommended dosage of Tylenol for children is as follows:
- Children under 3 months: Do not use Tylenol unless directed by a pediatrician.
- Children 3-11 months: Use 80 mg (4 mL of 20 mg/1 mL liquid or 1/4 teaspoon of 160 mg/5 mL liquid) every 4-6 hours as needed.
- Children 1-2 years: Use 160 mg (8 mL of 20 mg/1 mL liquid or 1/2 teaspoon of 160 mg/5 mL liquid) every 4-6 hours as needed.
- Children 2-3 years: Use 200 mg (10 mL of 20 mg/1 mL liquid or 2/3 teaspoon of 160 mg/5 mL liquid) every 4-6 hours as needed.
- Children 4-5 years: Use 240 mg (12 mL of 20 mg/1 mL liquid or 1 teaspoon of 160 mg/5 mL liquid) every 4-6 hours as needed.
- Children 6-11 years: Use 320 mg (16 mL of 20 mg/1 mL liquid or 1 1/3 teaspoons of 160 mg/5 mL liquid) every 4-6 hours as needed.
It’s essential to note that these dosages are general guidelines and may vary depending on the child’s individual needs and medical conditions. Always consult with a pediatrician before administering Tylenol to a child.
Risks of Overdose in Children
Overdose is a significant risk associated with the use of Tylenol in children. Acetaminophen overdose can cause liver damage, seizures, and even death. Symptoms of overdose include:
- Vomiting
- Abdominal pain
- Headache
- Nausea
- Diarrhea
- Dark-colored urine
- Yellowing of the skin and eyes
If you suspect your child has overdosed on Tylenol, seek medical attention immediately.
Safely Administering Tylenol to Children, How often to take tylenol
To safely administer Tylenol to children, follow these tips:
- Use the correct dosage based on your child’s age and weight.
- Measure the correct dose using a measuring device, such as a dropper or a syringe.
- Do not exceed the recommended dosage, even if your child’s pain or fever persists.
- Do not administer Tylenol to children who are taking other medications, such as aspirin or ibuprofen.
- Do not give Tylenol to children who have a history of liver disease or other medical conditions.
- Keep Tylenol out of reach of children and supervise their use of the medication.
By following these guidelines and tips, you can ensure the safe use of Tylenol in children and minimize the risk of overdose and other complications.
The Interaction of Tylenol with Other Medications
When taking Tylenol, it’s essential to be aware of the potential interactions with other medications. This is crucial to avoid adverse effects and ensure safe treatment. While Tylenol is generally considered safe, combining it with other medications can increase the risk of side effects.
Blood Thinners (Anticoagulants)
Tylenol can interact with blood thinners, such as warfarin, and increase the risk of bleeding. This is because Tylenol can slow down the liver’s ability to metabolize warfarin, leading to increased warfarin levels in the blood. As a result, the risk of bleeding complications, such as gastrointestinal bleeding or intracranial hemorrhage, may increase.
- Warfarin (Coumadin): Blood thinners like warfarin can interact with Tylenol, increasing the risk of bleeding complications.
- Aspirin (low dose): Aspirin can also interact with Tylenol, and the combination can increase the risk of bleeding.
It’s essential to inform your healthcare provider about any medications you’re taking, including blood thinners, to ensure safe treatment. Your healthcare provider may prescribe a lower dose of Tylenol or recommend alternative pain relief medications.
Certain Antidepressants
Tylenol can also interact with certain antidepressants, such as selective serotonin reuptake inhibitors (SSRIs), and increase the risk of serotonin syndrome. Serotonin syndrome is a potentially life-threatening condition that occurs when the levels of serotonin in the body become too high.
- SSRIs (fluoxetine, sertraline): Combining Tylenol with SSRIs can increase the risk of serotonin syndrome, particularly at high doses.
- Triptans: Tylenol can also interact with triptans, a type of medication used to treat migraines, and increase the risk of serotonin syndrome.
If you’re taking antidepressants and need to take Tylenol, it’s crucial to follow the recommended dosage and inform your healthcare provider about any interactions. Your healthcare provider may adjust your medication regimen to minimize the risk of adverse effects.
Other Medications to Use with Caution
Additionally, Tylenol can interact with other medications, such as:
- Nonsteroidal anti-inflammatory drugs (NSAIDs): Combining Tylenol with NSAIDs, like ibuprofen or naproxen, can increase the risk of stomach bleeding and ulcers.
- Muscle relaxants: Tylenol can interact with muscle relaxants, such as carisoprodol or cyclobenzaprine, and increase the risk of sedation and respiratory depression.
Always consult your healthcare provider before taking Tylenol, especially if you’re taking other medications or have underlying medical conditions. They will help you determine the safe dose and minimize potential interactions.
Important Reminders
To ensure safe treatment, always follow these guidelines:
- Inform your healthcare provider about any medications you’re taking, including prescription and over-the-counter medications.
- Follow the recommended dosage of Tylenol and do not exceed the maximum daily dose.
- Monitor your body’s response to Tylenol and report any side effects or allergic reactions to your healthcare provider.
By understanding the potential interactions between Tylenol and other medications, you can mitigate the risk of adverse effects and ensure safe treatment.
Certain medications can interact with Tylenol, increasing the risk of side effects. Always consult your healthcare provider before taking Tylenol, especially if you’re taking other medications.
Managing Side Effects of Tylenol
Taking Tylenol regularly can be beneficial for pain relief, but it’s not uncommon for individuals to experience side effects, such as stomach upset and drowsiness. To effectively manage these side effects, understanding their nature and how to mitigate them is essential.
Common Side Effects of Tylenol
Some of the most frequently reported side effects of Tylenol include stomach upset, drowsiness, and skin rashes. Stomach upset, in particular, can be uncomfortable and disrupt daily activities. Understanding the underlying causes of these side effects can lead to effective management strategies.
Stomach Upset: Causes and Prevention
Stomach upset is often caused by an increase in stomach acid or inflammation of the stomach lining. To prevent stomach upset when taking Tylenol, it’s recommended to take the medication with food. This can help slow down the digestion process and reduce the acidity of the stomach. Additionally, staying hydrated by drinking plenty of water can also aid in digestion and prevent constipation, a common symptom of stomach upset.
Minimizing the Risk of Side Effects
Several strategies can be employed to minimize the risk of side effects when taking Tylenol:
- Take the lowest effective dose: This can help reduce the risk of side effects while still providing adequate pain relief.
- Take Tylenol with food: As mentioned earlier, taking Tylenol with food can help prevent stomach upset.
- Stay hydrated: Drinking plenty of water can aid in digestion and prevent constipation.
- Monitor your body: Pay attention to how your body reacts to Tylenol, and report any side effects to your doctor.
Drowsiness: Causes and Prevention
Drowsiness is another common side effect of Tylenol, particularly when taken in large doses or in individuals who are sensitive to its effects. To prevent drowsiness when taking Tylenol, it’s recommended to:
- Take the medication in the morning: This can help avoid disrupting nighttime sleep patterns.
- Avoid combining Tylenol with other sedatives: This can increase the risk of drowsiness and other side effects.
- Get regular exercise: Regular physical activity can help reduce the risk of drowsiness and improve overall health.
Conclusion
Managing side effects of Tylenol requires understanding their underlying causes and employing effective prevention strategies. By taking the lowest effective dose, taking the medication with food, staying hydrated, and monitoring your body, you can minimize the risk of side effects and enjoy the benefits of Tylenol for pain relief.
The Role of Food in Absorbing Tylenol
When taking Tylenol, understanding how food affects its absorption and peak effect is crucial. Food can influence the way your body processes the medication, potentially impacting its effectiveness or increasing the risk of adverse effects. In this section, we will explore the impact of food on Tylenol absorption and provide tips on safe food choices while taking the medication.
### Fatty Foods and Liver Damage
Food, especially those high in fat, can affect the way Tylenol is absorbed and processed by the liver. When you consume fatty foods, the medication is delayed in being absorbed by the body, which can lead to a longer peak effect but also increase the risk of liver damage. This is because the liver has to work harder to metabolize the medication, which can put additional strain on the organ.
-
Liver Damage Risks
Studies have shown that taking Tylenol with high-fat meals can increase the risk of liver damage, especially in people who consume excessive amounts of acetaminophen. This is because the medication is absorbed more slowly, allowing it to accumulate in the liver and increasing the risk of toxicity.
-
Avoiding Fatty Foods
To minimize the risk of liver damage, it’s essential to avoid consuming fatty foods, especially when taking Tylenol or other medications containing acetaminophen. Opt for low-fat meals and snacks, and choose fatty foods in moderation.
-
Food Choices While Taking Tylenol
When taking Tylenol, it’s recommended to consume low-fat meals and snacks, such as fruits, vegetables, whole grains, and lean proteins. Avoid fatty foods, including oils, fried foods, and high-fat dairy products.
### Safe Food Choices While Taking Tylenol
While taking Tylenol, it’s essential to choose safe foods to minimize the risk of adverse effects and ensure the medication’s effectiveness. Here are some food options that can be safely consumed while taking Tylenol:
- Fresh fruits, such as apples, bananas, and berries
- Leafy greens, such as spinach, kale, and lettuce
- Lean proteins, such as chicken, turkey, and fish
- Whole grains, such as brown rice, quinoa, and whole-wheat bread
- Low-fat dairy products, such as milk, cheese, and yogurt
### Important Reminders
When taking Tylenol, it’s essential to remember the following:
* Always take the medication as directed by your healthcare provider.
* Avoid consuming high-fat meals or snacks while taking Tylenol.
* Choose low-fat meals and snacks, and opt for fatty foods in moderation.
* Inform your healthcare provider about any food allergies or sensitivities before taking Tylenol.
Ultimate Conclusion
In conclusion, understanding the recommended dosage of Tylenol and how often to take it is vital for maximizing its therapeutic benefits while minimizing the risk of adverse effects. By following the recommended guidelines and being mindful of potential interactions with other medications, individuals can safely and effectively use Tylenol to manage pain and alleviate discomfort.
User Queries
Q: Can I take Tylenol with alcohol?
A: No, it’s not recommended to take Tylenol with alcohol as it can increase the risk of liver damage and other adverse effects.
Q: Can I take Tylenol with other medications?
A: Always consult your doctor or pharmacist before taking Tylenol with other medications, as it may interact with certain medications and increase the risk of adverse effects.
Q: Can I take Tylenol if I have liver disease?
A: If you have liver disease, it’s essential to consult your doctor before taking Tylenol, as it can exacerbate liver damage and increase the risk of adverse effects.
Q: Can I take Tylenol with other pain relievers?
A: No, it’s not recommended to take Tylenol with other pain relievers, such as aspirin or ibuprofen, without consulting your doctor first, as it can increase the risk of adverse effects.