As how to get rid of varicose veins takes center stage, this opening passage beckons readers with a deep dive into a world crafted with good knowledge, ensuring a reading experience that is both absorbing and distinctly original. Varicose veins are a common condition that affects millions of people worldwide, causing discomfort, pain, and aesthetic concerns. But what exactly are varicose veins, and how can we get rid of them?
The answer lies in understanding the underlying causes and risk factors that contribute to the development of varicose veins. Genetic predisposition, lifestyle choices, and underlying medical conditions all play a significant role in increasing the likelihood of developing varicose veins. By addressing these risk factors, we can take proactive steps towards preventing the progression of varicose veins.
Understanding the Cause and Risk Factors of Varicose Veins
Varicose veins are a common condition characterized by the enlargement and twisting of veins, often leading to symptoms such as pain, swelling, and discoloration. While the exact cause of varicose veins is still not fully understood, research has identified several risk factors that contribute to their development.
Genetic Predisposition
Genetics play a significant role in the development of varicose veins. Individuals with a family history of varicose veins are more likely to develop the condition. A study published in the Journal of Vascular Surgery found that 70% of people with varicose veins had a family history of the condition. This suggests that genetic factors can contribute to the risk of developing varicose veins.
Genetic predisposition can manifest in several ways, including:
- Weak vein walls: Individuals with weak vein walls are more susceptible to varicose veins. Genetically, some people may inherit weak vein walls, making them more prone to varicose veins.
- Poor blood circulation: Genetics can also affect blood circulation, leading to poor circulation and an increased risk of varicose veins.
- Abnormal blood clotting: Certain genetic disorders can lead to abnormal blood clotting, which can increase the risk of varicose veins.
Lifestyle Choices
In addition to genetic factors, lifestyle choices can also contribute to the risk of developing varicose veins. Some of the most significant lifestyle factors include:
- Prolonged standing or sitting: Individuals who spend long periods standing or sitting may experience increased pressure on their veins, leading to varicose veins.
- Smoking: Smoking can damage the walls of veins, increasing the risk of varicose veins.
- Obesity: Excess weight can put additional pressure on veins, leading to varicose veins.
- Pregnancy: Hormonal changes during pregnancy can cause the veins to relax, leading to varicose veins.
Underlying Medical Conditions
Certain underlying medical conditions can increase the risk of developing varicose veins. Some of the most significant conditions include:
- High blood pressure: Increased blood pressure can cause veins to become damaged, leading to varicose veins.
- Thyroid disease: Certain thyroid conditions can affect blood circulation, leading to varicose veins.
- Diabetes: Diabetes can damage blood vessels, increasing the risk of varicose veins.
Importance of Addressing Risk Factors
Addressing risk factors is crucial in preventing the progression of varicose veins. By modifying lifestyle choices and managing underlying medical conditions, individuals can reduce their risk of developing varicose veins. Additionally, individuals with a family history of varicose veins should consider consulting with their healthcare provider to discuss their risk and develop a plan to prevent or manage the condition.
Early Detection and Diagnosis of Varicose Veins
Varicose veins are a common medical condition that can cause significant discomfort and impact daily life. Early detection and diagnosis are crucial in managing varicose veins effectively. A comprehensive diagnosis involves a combination of physical examination, imaging tests, and diagnostic procedures to determine the severity of the condition and develop an appropriate treatment plan.
Physical Examination, How to get rid of varicose veins
A physical examination is the initial step in diagnosing varicose veins. A healthcare provider will typically perform a visual examination of the affected area to look for signs of varicose veins, such as swelling, discoloration, and thickening of the skin. They may also use a Doppler ultrasound to identify any blood flow abnormalities. This method is non-invasive and can be done in a doctor’s office.
Physical examination has several benefits, including being non-invasive and cost-effective. However, it may not detect underlying causes of varicose veins, such as underlying medical conditions. Physical examination is a good starting point, but additional diagnostic methods may be necessary for an accurate diagnosis.
Imaging Tests
Imaging tests, such as Doppler ultrasound and magnetic resonance imaging (MRI), are used to visualize the blood vessels and determine the extent of the condition. These tests can help identify blood flow abnormalities, such as deep vein thrombosis, and provide a more accurate diagnosis.
Imaging tests are beneficial as they can provide detailed images of the affected area, allowing for a more accurate diagnosis. However, they may not be necessary for all cases of varicose veins. Additionally, imaging tests can be more expensive and may require specialized equipment.
Diagnostic Procedures
Diagnostic procedures, such as venogram and duplex ultrasound, are used to visualize the blood vessels and determine the severity of the condition. These procedures involve injecting a contrast agent into the affected vein to visualize its blood flow.
Diagnostic procedures are beneficial as they can provide detailed images of the affected area and help identify underlying causes of varicose veins. However, they may be more expensive and may require specialized equipment. Additionally, some diagnostic procedures may require sedation, which can be a drawback.
Ultrasound Tests
Ultrasound tests, such as Doppler ultrasound and duplex ultrasound, are widely used to diagnose varicose veins. These tests use sound waves to visualize the blood vessels and determine the extent of the condition.
Ultrasound tests have several benefits, including being non-invasive and cost-effective. They can also be used to monitor the effectiveness of treatment and detect any complications. However, they may not be as effective as other diagnostic methods in detecting underlying causes of varicose veins.
Comprehensive Diagnosis
A comprehensive diagnosis of varicose veins involves a combination of physical examination, imaging tests, and diagnostic procedures. This approach allows for an accurate diagnosis and development of an effective treatment plan.
A comprehensive diagnosis has several benefits, including allowing for early detection and treatment of varicose veins. It can also help prevent complications and improve quality of life for individuals affected by varicose veins.
Limitations of Diagnostic Methods
While diagnostic methods are beneficial in detecting varicose veins, they have several limitations. For example, physical examination may not detect underlying causes of varicose veins, and imaging tests may not be necessary for all cases.
The limitations of diagnostic methods are crucial to consider when developing a treatment plan for varicose veins. By understanding the benefits and limitations of each diagnostic method, healthcare providers can develop a more effective treatment plan that addresses the individual needs of each patient.
Importance of Early Detection
Early detection of varicose veins is crucial in managing the condition effectively. It allows for timely treatment and prevents complications, such as blood clots and skin ulcers.
Early detection has several benefits, including improving quality of life for individuals affected by varicose veins. It can also help prevent complications and reduce the risk of hospitalization. By detecting varicose veins early, healthcare providers can develop an effective treatment plan that addresses the individual needs of each patient.
Conservative Management of Varicose Veins
Conservative management of varicose veins involves non-surgical treatments to alleviate symptoms and prevent complications. These treatments aim to improve blood flow, reduce inflammation, and promote wound healing.
Compression Stockings
Compression stockings are a widely used conservative treatment for varicose veins. They work by applying pressure to the legs, which helps to push blood upwards towards the heart, reducing swelling and pain. Compression stockings are available in different compression classes, from mild to severe, and should be worn for at least 8 hours a day.
Compression stockings are usually made of a special elastic material that provides graduated compression, increasing the pressure from the foot to the thigh.
Elevation
Elevation is another conservative treatment that involves raising the legs above the level of the heart to improve blood flow and reduce swelling. This can be done by using a recliner or pillows to elevate the legs while sitting or lying down. It is essential to elevate the legs for at least 30 minutes, 3-4 times a day, to reduce pain and discomfort.
Exercise
Regular exercise is crucial in managing varicose veins. Exercise helps to improve blood flow, reduce inflammation, and promote wound healing. Activities such as walking, cycling, and swimming are recommended, as they are low-impact exercises that do not strain the legs. Additionally, exercises that strengthen the muscles in the legs, such as leg lifts and calf raises, can help improve blood flow and reduce swelling.
Lifestyle Modifications
Lifestyle modifications play a significant role in managing varicose veins. Maintaining a healthy weight, through a balanced diet and regular exercise, can reduce the pressure on the veins and improve blood flow. Avoiding prolonged standing or sitting can also help reduce swelling and pain. Furthermore, wearing loose-fitting clothing and avoiding tight socks can reduce pressure on the veins and improve circulation.
Weight Management
Maintaining a healthy weight is essential in managing varicose veins. Excess weight can put additional pressure on the veins, leading to swelling and pain. Research has shown that even a small weight loss of 5-10% can significantly improve symptoms and reduce the risk of complications.
For example, a study published in the Journal of Vascular Surgery found that weight loss was associated with improved symptoms and reduced risk of venous ulceration in patients with varicose veins.
Regular Exercise
Regular exercise is crucial in managing varicose veins. Exercise helps to improve blood flow, reduce inflammation, and promote wound healing. Activities such as walking, cycling, and swimming are recommended, as they are low-impact exercises that do not strain the legs. Additionally, exercises that strengthen the muscles in the legs, such as leg lifts and calf raises, can help improve blood flow and reduce swelling.
Avoiding Prolonged Standing
Avoiding prolonged standing or sitting can help reduce swelling and pain associated with varicose veins. Regular breaks to stretch and move around can help improve blood flow and reduce pressure on the veins. It is also essential to wear comfortable shoes and avoid high heels, which can increase pressure on the feet and legs.
Additional Tips
In addition to the above-mentioned treatments, there are several other tips that can help manage varicose veins. These include:
– Avoiding tight clothing that can constrict the veins
– Elevating the legs while sleeping
– Avoiding crossing the legs or ankles, which can reduce blood flow
– Avoiding standing or sitting for long periods
Surgical and Minimally-Invasive Treatments for Varicose Veins
Varicose veins can be managed through various surgical and minimally-invasive treatments that offer relief from symptoms and improve the appearance of the affected area.
Surgical and minimally-invasive treatments for varicose veins involve procedures that are designed to eliminate damaged or enlarged veins. These procedures can vary in terms of complexity, duration, and recovery time.
Sub-types of Surgical and Minimally-Invasive Treatments for Varicose Veins
Varicose vein treatments can include the following sub-types:
- Sclerotherapy: This procedure involves injecting a solution into the damaged vein to close it off. The solution causes the vein to collapse, and eventually, the body absorbs the dead tissue.
- Phlebectomy: This procedure involves surgically removing the damaged vein from the leg. The incision is usually small and can be made under local anesthesia.
- Radiofrequency Ablation: This procedure uses heat to close the damaged vein. A catheter is inserted into the vein, and radiofrequency energy is used to heat the vein, causing it to shrink and eventually close off.
In addition to these procedures, endo-vascular laser treatment and microwave ablation are also available. These procedures use heat or laser energy to close the damaged vein.
Comparison and Contrast of Surgical and Minimally-Invasive Treatments for Varicose Veins
When it comes to treating varicose veins, each procedure has its own advantages and disadvantages.
- Scarring: All surgical procedures involve some level of scarring. However, the extent and appearance of the scar can vary depending on the procedure.
- Pain: Most procedures involve some level of pain, but this is usually manageable with local anesthesia or pain medication.
- Recovery Time: Recovery time varies greatly depending on the procedure. Some procedures require only a few days of recovery, while others can take several weeks or even months.
- Risks and Complications: While rare, some complications can arise from these procedures, including infection, bruising, or scarring.
In general, minimally-invasive procedures such as sclerotherapy and radiofrequency ablation are considered less invasive and have a faster recovery time compared to surgical procedures like phlebectomy. However, the most effective treatment option for a patient will depend on their individual circumstances and the severity of their condition.
Important Considerations and Precautions
When deciding on the best course of treatment for varicose veins, it is essential to consider several factors, including the extent and severity of the condition, the patient’s overall health, and their individual preferences and needs.
Key Points to Keep in Mind
- Varicose veins can be treated with surgical and minimally-invasive procedures.
- The most effective treatment option will depend on the individual circumstances and severity of the condition.
- It’s crucial to consider various factors, including overall health, patient preferences, and the extent of the condition.
- Complications and risks should be carefully weighed against the potential benefits.
Alternative and Complementary Therapies for Varicose Veins
Alternative and complementary therapies have gained popularity in managing varicose veins, offering a holistic approach to alleviate symptoms and improve overall health. While these therapies may not be a replacement for conventional treatments, they can be used in conjunction with them to enhance the treatment outcome. In this section, we will discuss the use of herbal remedies, acupuncture, and essential oils in managing varicose veins.
Herbal Remedies
Herbal remedies have been used for centuries to treat various health conditions, including varicose veins. Some herbs have been found to have anti-inflammatory, antioxidant, and vasoconstrictive properties, which can help alleviate symptoms of varicose veins. Examples of herbal remedies that may be beneficial for varicose veins include:
- Cayenne pepper: Cayenne pepper contains capsaicin, which has been shown to improve circulation and reduce inflammation.
- Ginkgo Biloba: Ginkgo Biloba has been found to improve circulation and reduce the risk of blood clots.
- Butcher’s Broom: Butcher’s Broom has been used to treat varicose veins due to its anti-inflammatory and vasoconstrictive properties.
- Horse Chestnut: Horse Chestnut seed extract has been found to improve circulation and reduce inflammation.
These herbs can be consumed in various forms, including capsules, teas, or tinctures. However, it is essential to consult with a healthcare professional before using any herbal remedies, as they may interact with medications or have side effects.
Acupuncture
Acupuncture is an ancient Chinese practice that involves inserting thin needles into specific points on the body to stimulate the body’s natural healing processes. Studies have shown that acupuncture can help alleviate symptoms of varicose veins, including pain, swelling, and heaviness in the legs.
According to traditional Chinese medicine, varicose veins are caused by an imbalance of yin and yang energies in the body. Acupuncture is used to restore balance to these energies, which can help alleviate symptoms and improve circulation.
Essential Oils
Essential oils are highly concentrated plant extracts that can be used to promote relaxation, reduce inflammation, and improve circulation. Some essential oils that may be beneficial for varicose veins include:
- Lavender oil: Lavender oil has been found to promote relaxation and reduce anxiety, which can help alleviate symptoms of varicose veins.
- Peppermint oil: Peppermint oil has been shown to improve circulation and reduce inflammation.
- Eucalyptus oil: Eucalyptus oil has been used to treat varicose veins due to its anti-inflammatory and vasoconstrictive properties.
Essential oils can be used in various ways, including topical application, inhalation, or aromatherapy. However, it is essential to dilute essential oils with a carrier oil and consult with a healthcare professional before using them.
Creating a Treatment Plan for Varicose Veins
A well-structured treatment plan for varicose veins is a crucial step in providing effective management and relief for patients suffering from this condition. The plan should incorporate a combination of conservative management, surgical or minimally-invasive treatments, and alternative therapies. Developing a treatment plan requires careful consideration of several factors, including the severity of varicose veins, medical history, and patient preferences.
Assessing the Severity of Varicose Veins
Assessing the severity of varicose veins is a critical step in creating a treatment plan. This involves evaluating the size and appearance of the varicose veins, as well as any symptoms such as swelling, pain, or skin changes. A thorough evaluation helps determine the best course of treatment and whether conservative management or more invasive interventions are necessary.
Evaluating Medical History
Evaluating medical history is essential in developing a treatment plan for varicose veins. This includes reviewing a patient’s medical history, including any previous treatments or surgeries, as well as their current medication and lifestyle habits. A comprehensive review of medical history allows healthcare providers to identify potential risks and complications and develop a personalized treatment plan that takes into account any underlying medical conditions.
Considering Patient Preferences
Considering patient preferences is a crucial aspect of creating a treatment plan for varicose veins. Patients should be actively involved in the decision-making process, and their preferences and concerns should be taken into account when developing a treatment plan. This includes discussing the potential benefits and risks of different treatment options, as well as any lifestyle or lifestyle adjustments that may be necessary.
Developing a Personalized Treatment Plan
Developing a personalized treatment plan for varicose veins involves a comprehensive evaluation of the patient’s medical history, severity of varicose veins, and patient preferences. A thorough evaluation helps determine the best course of treatment, which may include a combination of conservative management, surgical or minimally-invasive treatments, and alternative therapies. The treatment plan should be tailored to the individual needs of each patient, taking into account their unique medical history, lifestyle, and preferences.
Examples of Treatment Plans
Developing a treatment plan for varicose veins requires a comprehensive evaluation of the patient’s medical history, severity of varicose veins, and patient preferences. Here are some examples of treatment plans that may be developed based on the severity of varicose veins and patient preferences:
*
- Conservative management, including compression stockings and elevation
- Surgical or minimally-invasive treatments, such as sclerotherapy or endovenous laser treatment
- Alternative therapies, such as acupuncture or herbal supplements
Benefits of a Personalized Treatment Plan
A personalized treatment plan for varicose veins offers several benefits, including improved management of symptoms, enhanced patient outcomes, and better quality of life. By tailoring a treatment plan to the individual needs of each patient, healthcare providers can ensure that patients receive the most effective and appropriate care for their condition.
Challenges in Developing a Treatment Plan
Developing a treatment plan for varicose veins can be challenging, particularly in patients with complex medical histories or multiple comorbidities. However, by taking a comprehensive and individualized approach, healthcare providers can overcome these challenges and develop effective treatment plans that meet the unique needs of each patient.
Treatment Plan Evaluation and Revision
Evaluating and revising a treatment plan for varicose veins is essential in ensuring that patients receive ongoing effective care. Treatment plans should be regularly reviewed and revised as necessary to reflect changes in a patient’s medical condition, symptoms, or treatment preferences. This may involve adjusting the treatment plan, adding new interventions, or discontinuing ineffective treatments.
Managing Pain and Discomfort Associated with Varicose Veins
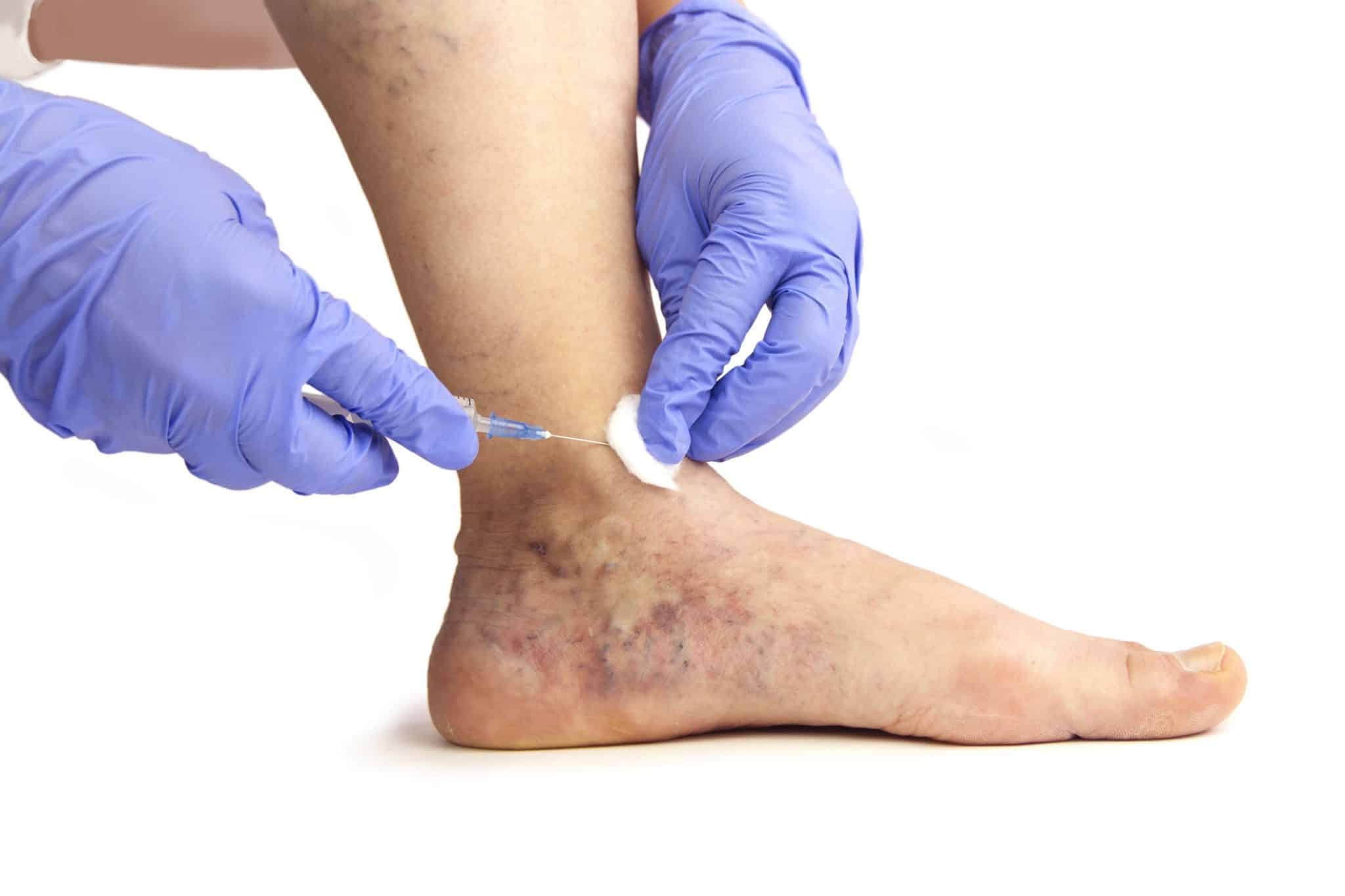
Managing pain and discomfort associated with varicose veins is an essential aspect of treatment. Varicose veins can cause a range of symptoms, including pain, itching, swelling, and discomfort, which can significantly impact a person’s quality of life. Effective management of pain and discomfort is crucial to ensure that individuals with varicose veins can maintain their daily activities and improve their overall well-being.
Pain Medication Options
There are several pain medication options available to manage pain and discomfort associated with varicose veins. Ibuprofen, acetaminophen, and naproxen are commonly used over-the-counter pain medications that can help alleviate pain and reduce inflammation. In some cases, prescription pain medications such as oxycodone or hydrocodone may be necessary to manage severe pain. It is essential to consult a healthcare professional to determine the best pain medication option for individual needs.
Heat Therapy
Heat therapy is another effective way to manage pain and discomfort associated with varicose veins. Applying a warm compress or heating pad to the affected area can increase blood flow and relax muscles, reducing pain and discomfort. Soaking in a warm bath or using a heating pad for 15-20 minutes several times a day can help alleviate symptoms.
Exercise and Stretching
Regular exercise and stretching can help reduce pain and discomfort associated with varicose veins. Aerobic exercises such as walking, cycling, or swimming can improve circulation and reduce pressure on the veins. Gentle stretching exercises, such as extending the legs or flexing the feet, can also help alleviate symptoms. It is essential to consult a healthcare professional before starting any new exercise program.
Compression Stockings
Wearing compression stockings can help reduce pain and discomfort associated with varicose veins by applying pressure to the affected area. Compression stockings can improve circulation and reduce swelling, which can help alleviate symptoms. It is essential to wear compression stockings according to the recommended compression level and to follow the care instructions provided.
Last Point
In the following sections, we will delve into the different treatment options available for varicose veins, from conservative management to surgical and minimally-invasive procedures. We will also explore alternative and complementary therapies, as well as the importance of creating a personalized treatment plan that addresses the unique needs of each individual. By the end of this article, you will have a comprehensive understanding of how to get rid of varicose veins and take control of your vein health.
Clarifying Questions: How To Get Rid Of Varicose Veins
What are the signs and symptoms of varicose veins?
The signs and symptoms of varicose veins include swollen, twisted, and blue-colored veins, especially in the legs. Additionally, you may experience pain, itching, and burning sensations in the affected area.
Can varicose veins be prevented?
Yes, varicose veins can be prevented by maintaining a healthy lifestyle, including regular exercise, weight management, and avoiding prolonged standing. Wearing compression stockings and elevating your legs can also help to prevent the development of varicose veins.
What are the treatment options for varicose veins?
The treatment options for varicose veins include conservative management, surgical procedures, and alternative therapies. Your doctor can help you determine the best course of treatment based on the severity of your condition.
How long does it take to recover from varicose vein surgery?
The recovery time from varicose vein surgery can vary depending on the type of procedure and individual factors. Typically, you can expect to return to normal activities within 1-2 weeks, although full recovery can take several months.