As how to know if you have a cavity takes center stage, this opening passage beckons readers into a world of good knowledge, ensuring a reading experience that is both absorbing and distinctly original.
The early warning signs of a cavity can be subtle, but recognizing them is crucial for preventing further tooth decay. In this article, we will delve into the early warning signs of a cavity, how cavities form and progress, the factors that contribute to their development, common places where they tend to form, methods of diagnosing them effectively, and treatment options for different stages of cavities.
Recognizing Early Warning Signs of Tooth Decay
Tooth decay is a common oral health issue affecting millions of people worldwide. Ignoring its early warning signs can lead to more severe and costly problems. Therefore, it is essential to recognize the early warning signs of tooth decay to prevent its progression.
Incipient Cavity Symptoms and Implications, How to know if you have a cavity
Incipiemt cavities can exhibit specific symptoms that, if ignored, can lead to tooth decay. The following three symptoms are commonly associated with incipient cavities:
- Discoloration or Enamel Loss: In the early stages of tooth decay, a yellow or brown spot may appear on the tooth surface, indicating enamel loss and potential cavity formation.
- Tooth Sensitivity: The decay process can cause the tooth’s dentin to be exposed, leading to sensitivity, especially when consuming hot, cold, sweet, or sour substances.
- Mild Pain or Ache: As the decay progresses, patients may experience a mild pain or ache, particularly when biting or chewing.
These symptoms are critical in identifying incipient cavities, allowing prompt treatment and prevention of more severe tooth decay.
Distinguishing Normal Tooth Sensitivity from Decaying Tooth Sensitivity
Tooth sensitivity is a common complaint, but it can be challenging to distinguish between normal sensitivity and sensitivity caused by incipient cavities. Normal sensitivity can be triggered by factors such as:
- Gum recession: Exposed roots can cause sensitivity, leading to discomfort when consuming hot, cold, or sweet substances.
- Tooth wear: Grinding, erosion, or attrition can expose dentin, resulting in sensitivity.
- Orthodontic treatment: Teeth being moved or manipulated during orthodontic treatment can cause sensitivity.
In contrast, sensitivity associated with incipient cavities tends to:
- Appear gradually: Sufferers often report a steady increase in sensitivity over time.
- Elicit pain or ache under pressure: A sharp bite or pressure can trigger pain or ache.
A dentist can diagnose the cause of tooth sensitivity by examining the tooth and performing a thorough oral health evaluation.
Common Misconceptions about Early Signs of Cavities
Misconceptions about early signs of cavities can lead to delayed treatment or neglect. Two common misconceptions are:
- Cavities only occur in sugary foods: While sugary foods do contribute to tooth decay, consuming sugary substances is not the sole cause of cavities. Other factors, such as saliva flow, oral hygiene, and genetics, also play crucial roles.
- Tooth decay only affects adults: Tooth decay can affect people of any age, including children. Regular dental check-ups and oral hygiene practices are essential, regardless of age.
Understanding these misconceptions and being aware of the early warning signs of tooth decay can help prevent more severe problems and maintain optimal oral health.
Understanding How Cavities Form and Progress
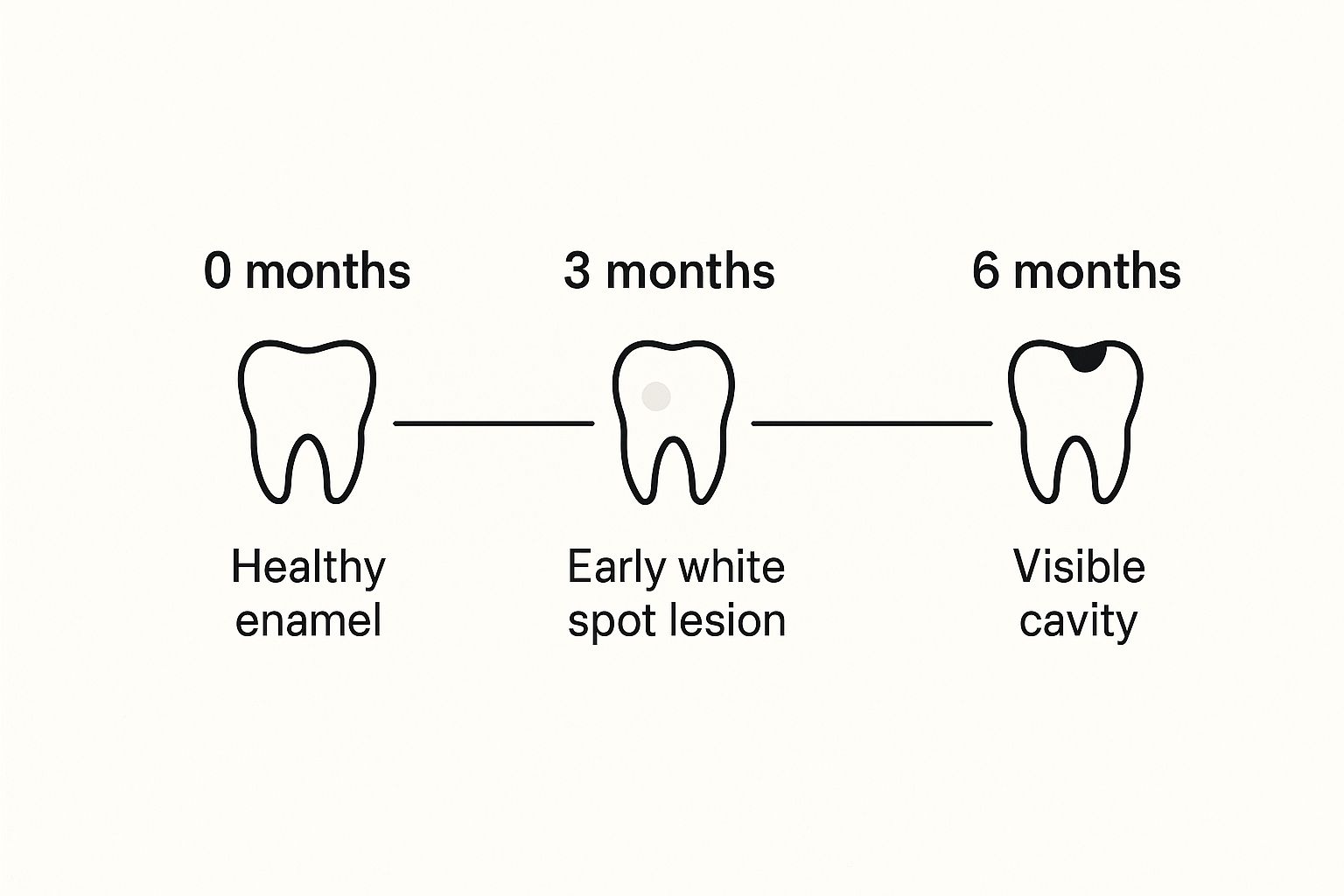
Cavities, also known as dental caries, are a common dental issue that affects millions of individuals worldwide. They are caused by a combination of factors, including diet, oral hygiene, and genetics. Understanding the process of cavity formation is crucial in preventing and treating them. In this section, we will delve into the process of demineralization and remineralization, the roles of bacteria, acid, and minerals, as well as the differences in cavity formation between permanent and baby teeth.
Demineralization and Remineralization Process
Demineralization is the process of tooth enamel losing its minerals, primarily calcium and phosphate, which makes it more susceptible to decay. This process is initiated by the presence of acid-producing bacteria in the mouth, such as Streptococcus mutans. When these bacteria feed on sugars and starches, they produce acid as a byproduct, which dissolves the minerals in the tooth enamel, causing it to weaken and decay. On the other hand, remineralization is the process of tooth enamel regaining its minerals. This process occurs naturally when the teeth are exposed to fluoride, which is found in toothpaste, mouthwash, and community water supplies. Fluoride helps to strengthen tooth enamel and make it more resistant to demineralization.
ApJ=Ca5(PO4)3OH
The chemical formula above represents the composition of tooth enamel. Tooth enamel is made up of hydroxyapatite, which is a calcium phosphate mineral. When acid dissolves the minerals in tooth enamel, it disrupts the crystal structure of hydroxyapatite, leading to tooth decay.
Roles of Bacteria, Acid, and Minerals in Cavities Formation
Bacteria play a crucial role in the formation of cavities. Certain types of bacteria, such as Streptococcus mutans, feed on sugars and starches and produce acid as a byproduct, which dissolves the minerals in tooth enamel. Acid is the primary agent of tooth decay, as it dissolves the minerals in tooth enamel, making it more susceptible to decay. Minerals, particularly calcium and phosphate, are essential in maintaining the health and strength of tooth enamel. When teeth are exposed to fluoride, it helps to strengthen tooth enamel and make it more resistant to demineralization.
Differences in Cavities Formation in Permanent Teeth versus Baby Teeth
Cavities can form in both permanent teeth and baby teeth, but the process of formation differs between the two. Baby teeth are more prone to cavities due to their thin enamel and open dental anatomy. They have larger pulp chambers and more exposed dentinal tubules, making them more susceptible to decay. Permanent teeth, on the other hand, have thicker enamel and more developed dentinal tubules. However, permanent teeth are also more prone to cavities, especially in older adults, due to the accumulation of plaque and tartar.
- Baby teeth are more prone to cavities due to their thin enamel and open dental anatomy.
- Permanent teeth have thicker enamel and more developed dentinal tubules, but are still susceptible to cavities, especially in older adults.
The differences in cavity formation between permanent and baby teeth are mainly due to the anatomy and development of the teeth. Baby teeth are more susceptible to decay due to their thinner enamel and more open dental anatomy, while permanent teeth are more prone to cavities due to the accumulation of plaque and tartar, as well as the wear and tear of the teeth over time.
Factors Influencing Demineralization and Remineralization
Several factors influence the demineralization and remineralization process. These include:
- Diet: Consuming a diet high in sugars and starches can increase the production of acid, leading to demineralization.
- Oral Hygiene: Failing to practice good oral hygiene can lead to the accumulation of plaque and tartar, which can contribute to demineralization.
- Genetics: Some people may be more prone to cavities due to their genetic makeup.
- Fluoride: Exposure to fluoride can help strengthen tooth enamel and make it more resistant to demineralization.
In summary, cavities form through a complex process involving the interaction of bacteria, acid, and minerals. Understanding the process of demineralization and remineralization is crucial in preventing and treating cavities. By knowing the factors that influence demineralization and remineralization, we can take steps to prevent the formation of cavities and maintain good oral health.
Common Places Where Cavities Tend to Form

Cavities can develop in various parts of the mouth, with some areas being more prone to decay than others due to factors like anatomy and function. Understanding the common places where cavities tend to form can help identify potential problem areas and inform dental care strategies.
The anatomy of the mouth plays a crucial role in determining the susceptibility of different tooth locations to cavities. Teeth that are difficult to clean or have a complex shape are more prone to decay.
Tooth Locations with High Prevalence of Cavities
The following table highlights the prevalence of cavities in different tooth locations:
| Tooth Location | Prevalence of Cavities (%) | Anatomical Reason | Function-Related Reason |
|---|---|---|---|
| Molars | 70-80% | Complex shape makes brushing challenging | Increased biting force and contact with opposing teeth |
| Pre-molars | 40-50% | Rounded shape and close proximity to molars | Increased risk of food impaction and decay |
| Incisors | 20-30% | Direct contact with opposing teeth and increased biting force | Difficulties in cleaning due to tongue and lip opposition |
| Canines | 10-20% | Pointed shape and limited contact with opposing teeth | Lower risk of decay compared to molars and pre-molars |
More Prone to Decay Areas in the Mouth
Two areas in the mouth are more prone to decay due to their anatomy and function:
* The chewing surface of the molars is prone to decay due to its complex shape and increased contact with opposing teeth. This area is also difficult to clean, making it susceptible to plaque buildup and decay.
* The area between the molars and pre-molars is prone to decay due to food impaction and difficulties in cleaning. This area is also subject to increased pressure from opposing teeth and masticatory forces.
Impact of Chewing Gum Habits on Cavity Formation
Chewing gum habits can have a significant impact on cavity formation in specific tooth regions. Research has shown that frequent gum chewing can lead to increased salivary flow, which can help to wash away food particles and neutralize acids. However, excessive gum chewing can also lead to tooth wear and increased risk of decay in the incisors and canines. Furthermore, using sugary gum can contribute to the development of cavities in areas where the gum is frequently chewed.
In addition, the following points should be noted regarding the impact of sugar-free gum on cavity formation:
* Sugar-free gum contains artificial sweeteners that can be up to 300 times sweeter than sugar and may be less effective in reducing the risk of cavities.
* The effect of sugar-free gum on cavity formation is still a subject of debate, and more research is needed to fully understand its impact.
* Regular dental check-ups and good oral hygiene practices are essential for maintaining a healthy smile, regardless of chewing gum habits.
Methods of Diagnosing Cavities Effectively
Regular dental check-ups are crucial for early detection of cavities and prevention measures. A dental professional can visually inspect the teeth, gums, and surrounding tissues for signs of tooth decay and provide personalized advice on oral hygiene and preventative care. Moreover, regular dental visits enable dentists to identify potential dental health issues in their early stages, making treatment more effective.
Importance of Regular Dental Check-Ups
Dental professionals use a combination of visual inspections, radiographs, and other diagnostic tools to identify signs of tooth decay and other oral health issues. Regular dental check-ups help in:
- Preventative treatments to prevent tooth decay and other oral health issues
- Early detection of oral health issues to prevent more complex treatments
- Personalized advice on oral hygiene and preventative care
Non-Invasive Procedures for Detecting Tooth Decay
Advanced technology has made it possible to detect tooth decay without invasive procedures. Two non-invasive procedures for detecting tooth decay are:
- Digital Intra-Oral Cameras: These cameras capture high-resolution images of the teeth and gums, enabling dentists to identify early signs of tooth decay, cracks, and other oral health issues.
- Laser Fluorosis Detection: This technology uses laser light to detect early signs of tooth decay and monitor the effectiveness of fluoride treatments.
Comparing Traditional Radiographs with Digital Radiographs
Dental radiographs have been a crucial tool for detecting tooth decay and other oral health issues. However, traditional radiographs have some limitations, such as:
- Exposure to radiation
- Degradation of image quality over time
Digital radiographs have addressed these limitations and provide:
- Better image quality
- Lower radiation exposure
- Easy image storage and retrieval
- Enhanced diagnostic capabilities
Digital radiographs use sensors that capture two-dimensional images of the teeth and surrounding tissues. These images can be enhanced and manipulated using computer software, enabling dentists to:
“Get a clearer picture of the teeth and surrounding tissues, making it easier to detect tooth decay and other oral health issues.” – American Dental Association
Digital radiographs can be used to detect tooth decay at various stages, from early signs to more advanced cavities. Dentists can use this technology to:
“Monitor the effectiveness of fluoride treatments and make informed decisions about further treatment.” – Academy of General Dentistry
This technology has revolutionized the way dentists detect and treat tooth decay, enabling them to provide more accurate diagnoses and effective treatments.
Treatment Options for Different Stages of Cavities
When a cavity is detected, prompt action is necessary to prevent further damage to the tooth and surrounding tissues. Treatment options vary depending on the stage and severity of the cavity. Early detection and intervention are crucial to prevent the need for more extensive and costly treatments.
Filling a Tooth with a Cavity
A filling is a common treatment for tooth decay. The procedure involves the following steps:
The process begins with the administration of local anesthesia to numb the area. This helps reduce discomfort during the procedure.
The dentist will then use a drill to remove the damaged portion of the tooth, taking care to preserve as much of the healthy tooth structure as possible.
Next, the cleaned and prepared tooth is filled with a filling material, typically amalgam or composite resin, which is then shaped and polished to match the natural contours of the tooth.
Once the filling is in place, the tooth is checked for proper fit and function, and any necessary adjustments are made.
Restoring a Tooth Beyond the Scope of a Filling
In cases where the cavity is advanced or extensive, a filling may not be sufficient to restore the tooth. In such instances, more complex procedures may be required, including:
-
Root canal treatment
This involves removing infected pulp tissue from within the tooth and replacing it with a filling material or dental implant.
-
Crown or inlay replacement
A crown is a cap placed over the entire tooth to restore its shape, size, and function, while an inlay is a custom-made filling inserted into a prepared cavity.
-
Tooth extraction
In severe cases, the tooth may be beyond repair, and extraction is necessary to prevent further complications.
These procedures may involve additional appointments, x-rays, and diagnostic tests to determine the best course of treatment. Your dentist will work with you to develop a personalized treatment plan.
Comparing Home Treatments and Professional Treatments for Early Cavities
For early cavities, various home treatments and professional treatments are available. Some home treatments include:
- Fluoride mouthwash or toothpaste
- Desensitizing toothpaste or gel
- Saliva stimulants or supplements
However, these treatments may not be as effective as professional treatments, which often involve customized care and advanced diagnostic tools. Professional treatments typically include:
- X-rays to diagnose and monitor the progression of the cavity
- Regular cleanings and check-ups to catch the cavity early
- Prescription-strength fluoride treatments or gels
It is essential to maintain regular dental check-ups and practice good oral hygiene to prevent the onset of cavities and ensure the effectiveness of treatment options.
Closure: How To Know If You Have A Cavity
In conclusion, knowing the early warning signs of a cavity and understanding how cavities form and progress can go a long way in preventing tooth decay. Regular dental check-ups, proper oral hygiene, and a balanced diet can significantly reduce the risk of developing cavities. By being aware of the common places where cavities tend to form and knowing how to diagnose them effectively, you can take control of your oral health and prevent unnecessary toothaches.
Essential FAQs
Is a cavity visible to the naked eye?
No, a cavity may not be visible to the naked eye until it has advanced significantly. In the early stages, a cavity may only appear as a small white spot on the tooth.
Can I diagnose a cavity myself?
No, it’s best to consult a dentist for an accurate diagnosis. A dentist can use specialized equipment to detect cavities in the early stages.
Can cavities be reversed?
Yes, some cavities can be reversed with the help of remineralization treatment. This involves applying a fluoride paste or gel to the tooth to help reverse early stages of decay.