How to know if you have periodontitis sets the stage for this enthralling narrative, offering readers a glimpse into a story that is rich in detail and brimming with originality from the outset.
Detecting periodontitis early on can make all the difference in preventing further complications and maintaining good overall health. With the right information and tools, you can take control of your gum health and catch any potential problems before they escalate.
Recognizing the Early Warning Signs of Periodontitis in Everyday Life
Periodontitis is a chronic bacterial infection of the gums and bone that support the teeth. It is a common condition that affects millions of people worldwide, yet many cases go undiagnosed until it’s too late. Early detection and treatment are crucial to preventing further complications, such as tooth loss and systemic diseases. Recognizing the early warning signs of periodontitis is essential for maintaining good oral health.
Subtle Symptoms of Periodontitis
The subtle symptoms of periodontitis are often overlooked by patients, leading to delayed diagnosis and treatment. Some common symptoms include:
- Red, swollen, or bleeding gums, especially during brushing or flossing
- Sensitive teeth or pain while chewing
- Loose teeth or changes in the fit of dentures
- Bad breath (halitosis) that persists despite good oral hygiene
These symptoms can be caused by various factors, including poor oral hygiene, genetics, or underlying medical conditions. However, when coupled with other risk factors, such as smoking or a family history of periodontitis, the likelihood of developing the disease increases.
Situations Where Patients Might Exhibit These Symptoms Without Realizing It
Many patients experience periodontitis symptoms in everyday situations, often without realizing it. For example:
- During athletic activities, such as contact sports, where teeth are subjected to sudden impacts
- When biting into hard foods, such as nuts or candy
- While playing musical instruments, where the mouth is subjected to constant vibrations
- During menstruation, when hormonal changes can increase gum sensitivity
These situations can exacerbate existing gum disease or trigger new symptoms, making early detection and treatment crucial.
The Importance of Early Detection and Treatment
Early detection and treatment of periodontitis are critical to preventing further complications. When left untreated, periodontitis can lead to:
- Tooth loss due to bone and gum damage
- Systemic diseases, such as diabetes, heart disease, or respiratory infections, which are linked to chronic inflammation
- Expensive dental procedures, such as dental implants or bridges, to replace lost teeth
Regular dental check-ups and good oral hygiene practices can help detect periodontitis early, allowing for prompt treatment and prevention of further complications.
How to Identify a Compromised Gumline
Visually inspecting your gumline is a crucial step in detecting periodontitis. A compromised gumline can be an indicator of underlying gum disease, which, if left untreated, can lead to tooth loss and other oral health issues. In this section, we will guide you through a step-by-step process to visually inspect your gumline and discuss the tools and equipment typically used in dental offices to assess gumline health.
Step-by-Step Visual Inspection Guide
To visually inspect your gumline, follow these steps:
- Use a mirror to view your gumline in its entirety. You can use a handheld mirror or ask someone to help you take a selfie with your mouth open.
- Look for any signs of inflammation, redness, or bleeding. Healthy gums are typically pink in color and firm to the touch.
- Check for any spacing between your teeth. A compromised gumline can cause teeth to shift or become unevenly spaced.
- Inspect your gumline for signs of recession, such as exposed roots or tooth decay.
- Check for any unusual sensations when chewing or biting food. You may notice sensitivity or discomfort if your gumline is compromised.
Tools and Equipment Used in Dental Offices
Dental professionals use various tools and equipment to assess gumline health. These include:
- Periodontal probes: These are long, thin instruments used to measure the depth of the gum pockets between your teeth and gums.
- Ultrasonic scalers: These devices are used to remove plaque and tartar from your teeth and gums, helping to prevent gum disease.
- Pocket depth measurement devices: These tools help measure the depth of the gum pockets, providing an accurate assessment of your gumline health.
Images of Healthy and Compromised Gumlines
A healthy gumline is typically pink in color and firm to the touch. When gum disease is present, the gumline may appear red, inflamed, or bleeding.
Healthy Gumline: A healthy gumline is characterized by a smooth, even texture and a firm consistency. The gums are tightly attached to the teeth, with no visible gaps or spaces.
Compromised Gumline: A compromised gumline is characterized by redness, inflammation, or bleeding. The gums may appear swollen, and there may be visible gaps or spaces between the teeth and gums.
Exposed Roots: In advanced cases of gum disease, the gumline may recede, exposing the roots of the teeth. This can make the teeth appear longer and can increase sensitivity to temperature changes.
Visible Tartar Buildup: A compromised gumline can lead to visible tartar buildup, which can make the teeth appear discolored or yellow.
Unraveling the Mystery of Periodontitis
Periodontitis, a chronic bacterial infection of the gums and bone supporting the teeth, continues to be a significant public health concern. Recent studies have shed light on the complex interplay between genetic and environmental factors that contribute to the development and progression of periodontitis. In this section, we will delve into the genetic predisposition to periodontitis and the role of environmental factors, including smoking and poor oral hygiene.
Genetic Predisposition to Periodontitis
Research has identified several genetic variants associated with an increased risk of developing periodontitis. These genetic variations can affect the function of various proteins involved in the immune response, inflammation, and tissue repair. For example, genetic variants in the NOD2/CARD15 gene have been linked to an increased risk of periodontitis in certain populations.
Environmental Factors that Contribute to Periodontitis
While genetic predisposition plays a role in the development of periodontitis, environmental factors can trigger or exacerbate the disease. Smoking, for instance, is a well-established risk factor for periodontitis, increasing the risk of tooth loss and bone loss.
Role of Gut Microbiome in Maintaining Oral Health
Recent studies have highlighted the importance of the gut microbiome in maintaining oral health. The gut microbiome plays a crucial role in regulating the immune response and inflammation in the body, which can impact oral health. An imbalance of the gut microbiome, known as dysbiosis, has been linked to various oral health conditions, including periodontitis.
Environmental Factors that can Affect Gut Microbiome
Poor oral hygiene, smoking, and a diet high in sugar and processed foods can disrupt the balance of the gut microbiome, leading to changes in the oral microbiome and increasing the risk of periodontitis.
Impact of Smoking on Oral Health
Smoking is a well-established risk factor for periodontitis, and its impact on oral health is multifaceted. Smoking can impair blood flow to the gums, reducing the delivery of oxygen and nutrients necessary for healing. Additionally, smoking can alter the chemistry of the saliva, increasing the acidity and reducing the flow of saliva, which is essential for neutralizing acids and remineralizing teeth.
Benefits of Maintaining a Healthy Gut Microbiome
Maintaining a healthy gut microbiome is crucial for oral health. A balanced gut microbiome can help regulate inflammation, promote tissue repair, and support the immune system, all of which are essential for maintaining healthy gums and teeth.
Tips for Maintaining a Healthy Gut Microbiome
To maintain a healthy gut microbiome and support oral health, consider incorporating the following habits into your daily routine:
- Practice good oral hygiene, including regular brushing and flossing,
- Quit smoking and avoid secondhand smoke,
- Eat a balanced diet rich in fruits, vegetables, and whole grains,
- Stay hydrated by drinking plenty of water,
- Consider incorporating probiotics or prebiotics into your diet to support the growth of beneficial bacteria.
Debunking Common Myths and Misconceptions Surrounding Periodontitis
Periodontitis is a common oral health condition that affects millions of people worldwide, yet there are many misconceptions and myths surrounding its causes, symptoms, and treatment. Debunking these myths is crucial for raising awareness about the importance of maintaining good gum health and preventing periodontitis.
Distinguishing Periodontitis from Gingivitis
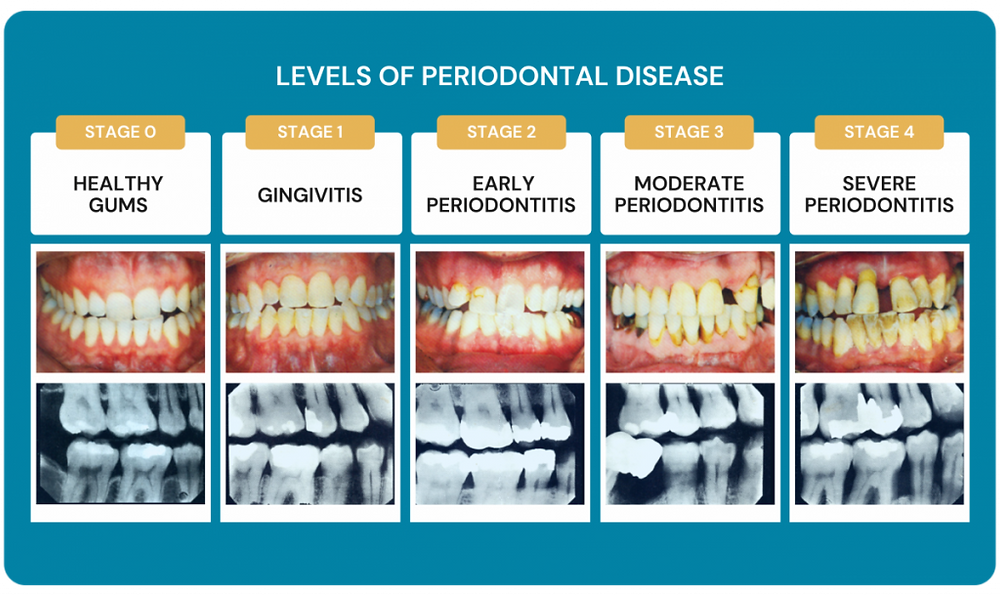
Many people are unsure about the difference between periodontitis and gingivitis, two conditions often linked to gum disease. While both conditions involve inflammation of the gums, there are significant differences between them. Gingivitis is a mild form of gum disease that can be reversed with good oral hygiene and regular dental check-ups. Periodontitis, on the other hand, is a more severe condition that can lead to the loss of teeth and bones supporting the teeth if left untreated.
The Consequences of Neglecting Gum Health
Ignoring gum health can have severe consequences, including but not limited to:
- The onset of periodontitis, a condition that can lead to tooth loss and other systemic diseases.
- The destruction of the gums and underlying bone structure, which can lead to changes in bite alignment and chewing difficulties.
- The risk of respiratory and cardiovascular diseases, which are linked to the spread of bacteria from the mouth to the bloodstream.
- The financial burden of expensive dental treatments, which can be avoided with regular dental check-ups and good oral hygiene.
The importance of maintaining good gum health cannot be overstated, and regular dental check-ups, flossing, and brushing are crucial for preventing periodontitis and other oral health issues.
Myths and Misconceptions about Periodontitis
Some common myths and misconceptions about periodontitis include:
In reality, periodontitis can affect anyone, regardless of oral hygiene habits. Factors such as genetics, hormonal changes, and certain medical conditions can increase the risk of developing periodontitis.
Unfortunately, neglecting periodontitis can lead to severe consequences, such as tooth loss and systemic diseases.
While dental restorations can help prevent periodontitis, they are not a substitute for regular dental check-ups and good oral hygiene.
Periodontitis can affect people of all ages, from children to adults. Regular dental check-ups and good oral hygiene are essential at any age.
The Importance of Maintaining a Regular Dental Routine
Maintaining a regular dental routine is crucial for preventing periodontitis and other oral health issues. This includes:
- Brushing teeth at least twice a day with a fluoride toothpaste.
- Flossing once a day to remove food particles and plaque from between teeth and below the gum line.
- Visiting the dentist for regular check-ups and cleanings every six months.
- Eating a balanced diet that includes plenty of fruits, vegetables, and whole grains.
By following these simple tips and staying informed about oral health, individuals can reduce the risk of developing periodontitis and maintain a healthy, beautiful smile.
The Role of Diet and Nutrition in Managing Periodontitis
A well-balanced diet plays a crucial role in maintaining overall health, including the health of your gums. Periodontitis, a bacterial infection that damages the gums and bone that support your teeth, has been linked to various nutritional deficiencies. Consuming a diet rich in essential nutrients can help prevent the development and progression of periodontitis.
Impact of a Poor Diet on Periodontitis Development, How to know if you have periodontitis
A diet high in processed foods, sugars, and refined carbohydrates can lead to an imbalance of the gut microbiome, resulting in an overgrowth of pathogenic bacteria that cause periodontitis. This is because these foods are often low in essential nutrients and high in inflammation-promoting compounds. Furthermore, a diet lacking in essential vitamins and minerals can impair the body’s ability to repair and regenerate gum tissue, making it more susceptible to periodontal disease.
- Consuming high amounts of sugar and refined carbohydrates can lead to an increased risk of periodontitis due to the overgrowth of pathogenic bacteria in the mouth.
- A diet low in essential nutrients such as vitamin C, calcium, and omega-3 fatty acids can impair gum health and increase the risk of periodontitis.
- Consuming a diet high in processed meats and saturated fats can lead to chronic inflammation, which can exacerbate periodontal disease.
The Importance of Vitamin C in Gum Health
Vitamin C is a crucial nutrient for maintaining healthy gums. It plays a vital role in the synthesis of collagen, a protein that gives structure to gum tissue. Vitamin C also has antioxidant properties, which help to protect gum tissue from oxidative damage caused by free radicals. Inadequate vitamin C levels have been linked to an increased risk of periodontitis.
| Vitamin C Sources | Daily Recommended Intake |
|---|---|
| Fruits (e.g., citrus fruits, strawberries), leafy greens, and bell peppers | 60 mg/day for women, 90 mg/day for men |
The Role of Calcium in Gum Health
Calcium is another essential nutrient for maintaining healthy gums. It plays a crucial role in the mineralization of bone tissue, which is essential for maintaining the structure and function of gums and teeth. Inadequate calcium levels have been linked to an increased risk of periodontitis.
- Regularly consuming calcium-rich foods such as dairy products, leafy greens, and fortified plant-based milk can help support gum health and reduce the risk of periodontitis.
- Additionally, taking a calcium supplement can help to maintain adequate calcium levels and support gum health.
Modifying Your Diet to Reduce Periodontitis Risk
To reduce your risk of periodontitis, incorporate the following dietary changes into your daily routine:
1. Increase your consumption of essential nutrients, such as vitamin C and calcium, through a balanced diet rich in fruits, vegetables, whole grains, and lean proteins.
2. Limit your intake of processed foods, sugars, and refined carbohydrates, which can lead to an imbalance of the gut microbiome and increase the risk of periodontitis.
3. Consider taking a vitamin C and calcium supplement to support gum health, particularly if you have a restrictive diet or are unable to consume enough of these nutrients through your diet alone.
Last Recap
In conclusion, it’s essential to understand the signs, symptoms, and risk factors associated with periodontitis. By taking proactive steps to maintain good gum health and seeking regular dental care, you can significantly reduce your risk of developing periodontitis and safeguard your overall well-being.
Helpful Answers: How To Know If You Have Periodontitis
What is the primary difference between periodontitis and gingivitis?
Gingivitis is a mild form of gum disease that causes inflammation of the gums, while periodontitis is a more severe condition that causes inflammation of the gum tissue and can lead to tooth loss.
Can periodontitis affect people of any age?
Yes, periodontitis can affect people of any age, including children and teenagers. However, it is more common in adults and seniors.
How often should I visit my dentist for a check-up?
The American Dental Association recommends visiting your dentist for a check-up at least twice a year to identify and address any oral health issues early on.
