How to know if you need hip surgery – Kicking off with understanding hip pain patterns that indicate the need for surgery, this opening section will explore the various signs and symptoms that may signal the requirement for surgical intervention. Identifying these patterns and understanding the role of radiating pain and numbness in determining the necessity for hip surgery are crucial steps in making informed decisions about one’s health. Additionally, we will delve into the connection between hip surgery and age-related decline, exploring how osteoarthritis can accelerate the need for hip surgery and the importance of maintaining a healthy lifestyle to slow down age-related hip decline. With a focus on empowering readers to take control of their health, we will navigate the complexities of hip surgery, including the weighing of risks and benefits, as well as alternative treatment options, such as nonsurgical therapies. By the end of this journey, readers will have a clear understanding of when it’s time to consider hip surgery and how to approach this decision with confidence.
Let’s talk about the distinctive patterns of hip pain that may signal the requirement for surgical intervention. We’ll also explore how osteoarthritis can accelerate the need for hip surgery by explaining its progression and consequences. Furthermore, we’ll delve into the importance of maintaining a healthy lifestyle to slow down age-related hip decline and examine the potential risks associated with hip surgery. By the end of this section, you’ll have a deeper understanding of when it’s time to consider hip surgery and how to approach this decision with confidence.
Identifying Hip Pain Patterns that Indicate the Need for Surgery
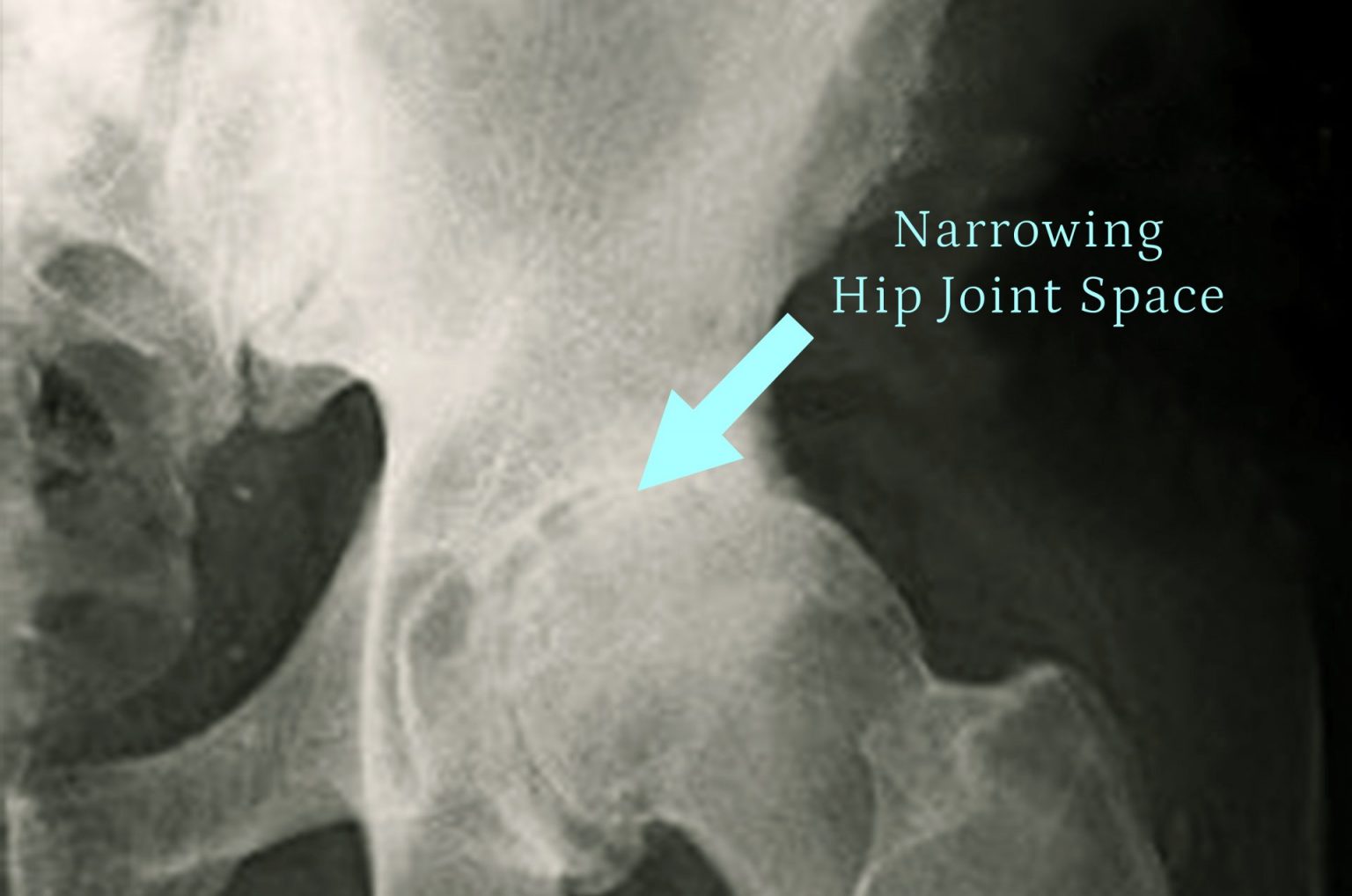
Hip pain is a common issue that affects millions of people worldwide, and in many cases, it can be managed with conservative treatments such as physical therapy, pain medications, and lifestyle modifications. However, in some instances, hip pain can be a sign of a more serious underlying condition that may require surgical intervention. Identifying the distinctive patterns of hip pain that may signal the need for surgery is crucial in ensuring timely and effective treatment.
Radiating pain and numbness are common symptoms of nerve compression or damage in the hip region. When pain radiates from the hip to other areas such as the thighs, knees, or buttocks, it may indicate nerve compression or damage, which can be a sign of a more serious underlying condition that requires surgical intervention. Similarly, numbness or tingling sensations in the legs can indicate nerve damage or compression, which may require surgical correction.
### Conditions that Increase the Likelihood of Surgery
Certain conditions may increase the likelihood of surgery being recommended for hip pain. These conditions include:
### Osteoarthritis
* Characterized by Wear and tear on the Cartilage
* The joint space is reduced leading to reduced movement
* Bony spurs develop and cause bone on bone wear
### Rheumatoid Arthritis
* A chronic autoimmune condition that causes Inflammation and Cartilage degeneration
* Morning stiffness is common, and joint pain worsens through the day
* Often leads to deformities and requires Surgical intervention
### Hip Labral Tear
* A Tear in the Cartilage around the socket of the joint
* Can cause Pain, Stiffness and reduced movement
* Surgical intervention is required to repair or replace the Labrum
### Hip Impingement
* A condition where the bones of the hip joint Rub and Grind against each other
* Can cause Pain during activities and at rest
* Surgical intervention is required to repair or replace the hip joint
### Hip Avulsion Fracture
* A condition where a piece of bone is Avulsed from the bone
* Can cause Severe pain and Instability of the joint
* Surgical intervention is required to repair the bone and restore the joint
### Hip Dysplasia
* A condition where the hip joint is not properly formed
* Can cause Pain, Stiffness and reduced movement
* Surgical intervention is required to stabilize the joint and improve mobility
Understanding the Effects of Wear and Tear on Hip Joint Health: How To Know If You Need Hip Surgery
Over time, our hip joints undergo a natural wear and tear process, which can lead to various health issues. One of the most common conditions that result from this wear and tear is osteoarthritis, a degenerative joint disease that affects millions of people worldwide. Understanding the progression and consequences of osteoarthritis is crucial in determining the need for hip surgery.
Osteoarthritis progresses through several stages, each with distinct symptoms and consequences. In the initial stages, cartilage loss occurs, causing friction between the bones, leading to pain and stiffness. As the disease advances, the cartilage breaks down completely, resulting in bone-on-bone grinding, a painful and debilitating condition. This grinding can lead to further complications, such as joint deformity and muscle weakness.
Bone-on-Bone Grinding: The Consequence of Advanced Osteoarthritis
Bone-on-bone grinding is a hallmark of advanced osteoarthritis. It occurs when the cartilage that cushions the bones wears down, allowing the bones to rub against each other. This friction generates intense pain, stiffness, and limited mobility. The grinding noise, often compared to the sound of sandpaper or fingernails on a chalkboard, is a result of the bone-to-bone contact.
Bone-on-bone grinding can be incredibly painful, making everyday activities challenging. It can also lead to muscle atrophy, further compromising joint function. In severe cases, joint deformity can occur, significantly impacting quality of life.
Differences in Hip Joint Wear between Men and Women
Research has shown that hip joint wear differs between men and women. Women are at a higher risk of developing osteoarthritis due to various factors, including hormonal changes, joint instability, and obesity. Women’s hips also tend to have a shallower joint space, making them more susceptible to joint wear.
Men, on the other hand, tend to have a larger joint space, which can delay the onset of osteoarthritis. However, men still experience hip joint wear due to factors such as muscle imbalances, poor biomechanics, and injury.
In women, hormonal fluctuations during menopause can accelerate joint degeneration. The decrease in estrogen levels can lead to a reduction in the production of cartilage and other joint fluids, making women more prone to osteoarthritis.
Muscle Weakness and Impaired Function
In addition to pain and grinding noise, osteoarthritis can lead to significant muscle weakness and impaired function. As the joint wears down, surrounding muscles compensate for the loss of joint support, leading to muscle fatigue and weakness. This can result in limited mobility, making everyday activities challenging.
In severe cases, joint fusion or replacement surgery may be necessary to alleviate pain and restore function. Understanding the progression and consequences of osteoarthritis is essential in determining the need for surgical intervention and developing effective treatment plans.
In the next section, we will discuss the importance of maintaining a healthy lifestyle to slow down hip joint wear and reduce the risk of osteoarthritis.
The Connection Between Hip Surgery and Age-Related Decline
As people age, their hip joints naturally undergo changes that can lead to degenerative conditions such as osteoarthritis. The wear and tear on hip cartilage and bone density accelerates with each passing year, increasing the likelihood of requiring hip surgery.
The relationship between aging and hip joint health is well documented. Hip cartilage wears down faster than other tissues in the body, and bone density decreases, making bones more prone to fractures. This decline in hip joint health can lead to severe pain, reduced mobility, and decreased quality of life.
Aging and Hip Joint Health: A Comparative Analysis
Understanding the effects of age on hip joint health is crucial in determining when surgical intervention may be necessary. The following table highlights the key differences in hip joint health among various age groups:
| Age Group | Age-Related Decline Factors | Hip Condition Risks | Surgical Intervention Rates |
|---|---|---|---|
| 20-39 years | Minimal wear and tear, normal bone density | Low risk of hip conditions | <1% |
| 40-59 years | Gradual wear and tear, normal to mildly decreased bone density | Moderate risk of hip conditions | 5-15% |
| 60-79 years | Significant wear and tear, noticeably decreased bone density | High risk of hip conditions | 20-40% |
| 80+ years | Severe wear and tear, severely decreased bone density | Very high risk of hip conditions | 40-60% |
Maintaining a Healthy Lifestyle to Slow Down Age-Related Hip Decline
While age-related hip decline is unavoidable, maintaining a healthy lifestyle can significantly slow down the process. By incorporating regular exercise, eating a balanced diet, and staying hydrated, individuals can reduce their risk of developing severe hip conditions.
Regular exercise, such as walking, swimming, or cycling, can help maintain strong muscles and bones, reducing the risk of osteoporosis and osteoarthritis. A balanced diet rich in fruits, vegetables, whole grains, and lean proteins provides essential nutrients for bone health.
Furthermore, maintaining a healthy weight can reduce the strain on hip joints, slowing down the wear and tear process. Smoking cessation and limiting excessive alcohol consumption also contribute to overall bone health.
Engaging in activities that promote mobility, such as yoga or tai chi, can also help maintain flexibility and balance, reducing the risk of falls and related hip injuries. By taking a proactive approach to hip health, individuals can mitigate the effects of age-related hip decline and maintain their quality of life.
Weighing the Risks and Benefits of Elective Hip Surgery
When considering elective hip surgery, it’s essential to weigh the potential risks against the benefits. While surgery can help alleviate pain and improve mobility, it’s crucial to understand the potential risks involved.
Risks Associated with Hip Surgery
There are several potential risks associated with hip surgery, including:
- Bleeding and blood clots: As with any surgery, hip replacement surgery carries a risk of bleeding and blood clots. This can be managed with medication and anticoagulant therapy, but it’s essential to discuss the risks with your surgeon.
- Infection: As with any surgical procedure, there is a risk of infection with hip surgery. This can be minimized with proper antibiotic treatment and post-operative care.
- Nerve damage: The nerves surrounding the hip joint can be damaged during surgery, leading to numbness, tingling, or weakness in the affected area.
- Dislocation: The artificial hip joint can dislocate, especially in the first few months after surgery. This can be managed with physical therapy and pain management.
- Metal allergy: Some people may be allergic to the metal used in hip replacement implants. This can cause an allergic reaction and discomfort.
- Bone fractures: The bone may be weakened during surgery, leading to fractures. This can be managed with medication and physical therapy.
Each of these risks can be minimized with proper pre-operative planning, surgery, and post-operative care.
When to Consider Elective Hip Surgery without Pain
In some cases, patients may consider elective hip surgery even without pain. For example:
- Advanced osteoarthritis: Patients with advanced osteoarthritis may consider surgery to prevent further joint damage and alleviate potential pain in the future.
- Young patients: Young patients with hip dysplasia or other congenital conditions may consider surgery to prevent long-term damage to the hip joint.
- High-impact lifestyle: Patients with a high-impact lifestyle, such as athletes or dancers, may consider surgery to prevent joint damage and alleviate potential pain in the future.
These scenarios can be complex and require careful consideration with your surgeon.
Advantages of Minimally Invasive Surgical Approach
Minimally invasive surgical approaches, such as laparoscopic or arthroscopic surgery, have been developed to reduce the risks associated with traditional open surgery. These approaches often result in:
- Smaller incisions: Minimally invasive approaches require smaller incisions, leading to less tissue damage and scarring.
- Reduced blood loss: Minimally invasive approaches often result in less blood loss, reducing the risk of complications.
- Shorter recovery time: Patients who undergo minimally invasive surgery often experience a shorter recovery time and less pain in the first few days after surgery.
However, the suitability of minimally invasive approaches depends on individual patient factors and should be discussed with your surgeon.
Alternative Treatment Options to Hip Surgery

If you’re experiencing hip pain or discomfort, you may be considering surgical options to alleviate symptoms. However, there are alternative treatment options available that can help you manage hip conditions without undergoing surgery. In this section, we’ll explore effective nonsurgical treatments for hip conditions, including physical therapy and injections.
Physical therapy is a non-invasive treatment option that helps improve hip movement, strength, and flexibility. It often involves exercises and stretches that target specific muscle groups, such as the hip abductors and extensors. Physical therapy can be tailored to address a range of hip conditions, from tendonitis to osteoarthritis.
Injectable Therapies
Injectable therapies, such as corticosteroid injections and hyaluronic acid injections, can provide short-term relief from hip pain. Corticosteroid injections involve injecting a corticosteroid medication into the affected joint to reduce inflammation. Hyaluronic acid injections involve injecting a substance that helps maintain joint lubrication and reduce friction. While injectable therapies may not offer long-term solutions, they can provide temporary symptom relief.
Physical Therapy Approaches
Physical therapy approaches for hip conditions often involve a combination of exercises and stretches. These may include:
- Pelvic tilts: A pelvic tilt exercise involves lying on your back with your knees bent and feet flat on the floor. Slowly tilt your pelvis upwards and then back down again, repeating the motion for several repetitions.
- Glute bridges: A glute bridge exercise involves lying on your back with your knees bent and feet flat on the floor. Slowly lift your hips up towards the ceiling, squeezing your glutes as you lift.
- Lateral leg lifts: A lateral leg lift exercise involves lying on your side with your legs straight. Slowly lift your top leg up towards the ceiling, keeping it straight, and then lower it back down again.
When to Choose Nonsurgical Therapies
The decision to choose nonsurgical therapies over hip surgery depends on several factors, including:
- Severity of symptoms: If your symptoms are mild to moderate, nonsurgical therapies may be sufficient to alleviate symptoms.
- Age and overall health: If you’re younger or have underlying health conditions, nonsurgical therapies may be a safer option.
- Extent of joint damage: If the joint damage is minimal, nonsurgical therapies may be more effective in preserving joint health.
- Personal preferences: If you prefer non-invasive treatments or have a strong preference for avoiding surgery, nonsurgical therapies may be a better option.
Combining Strategies for Maximum Benefit
To maximize the benefits of nonsurgical therapies, it’s often recommended to combine multiple strategies. This may involve a combination of physical therapy, injections, and lifestyle modifications, such as weight loss and exercise programs. By addressing multiple aspects of hip health, you can reduce symptoms and delay the need for surgery.
Real-Life Examples, How to know if you need hip surgery
Many people have successfully used nonsurgical therapies to manage hip conditions. For example, a study published in the Journal of Orthopaedic & Sports Physical Therapy found that a group of patients with hip osteoarthritis who underwent physical therapy showed significant improvements in pain and functional ability.
Final Review
As we conclude this journey, remember that understanding the signs and symptoms of hip pain is the first step towards making informed decisions about your health. By being aware of the distinctive patterns of hip pain that may indicate the need for surgery, you’ll be empowered to take control of your health and make the best decisions for your body. Whether you’re facing surgery or exploring alternative treatment options, it’s essential to prioritize your health and well-being. By doing so, you’ll be taking the first step towards a healthier, happier you.
General Inquiries
Can hip surgery be avoided through lifestyle changes?
While lifestyle changes cannot completely avoid hip surgery, maintaining a healthy weight, exercising regularly, and managing stress can slow down age-related hip decline and potentially reduce the need for surgery.
What are the potential risks associated with hip resurfacing or replacement?
Common risks associated with hip resurfacing or replacement include infection, dislocation, and nerve damage. However, modern surgical techniques and advancements in technology have significantly reduced these risks.
Can physical therapy delay the need for hip surgery?
Physical therapy can help alleviate symptoms and delay the need for hip surgery in some cases, especially for patients with mild to moderate hip joint damage. However, for more severe cases, hip surgery may still be necessary.