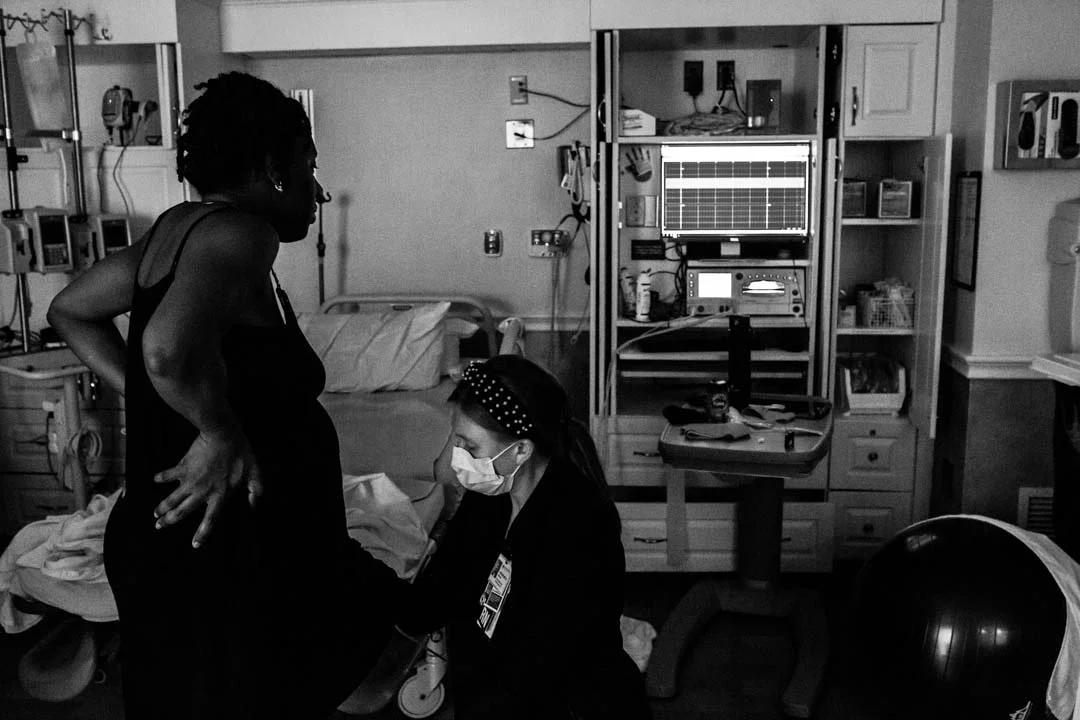
How to read contraction monitor – How to read a contraction monitor sets the stage for understanding the critical importance of fetal heart rate monitoring in a pregnant woman’s health journey. This vital process ensures the well-being of the fetus and the mother, and it’s a crucial step in ensuring a healthy pregnancy outcome.
As we delve into the world of contraction monitoring, it’s essential to prepare for the process, understand how to operate the contraction monitor device, and grasp the significance of fetal heart rate patterns. This comprehensive guide will walk you through each step, providing you with a clear and concise understanding of how to read a contraction monitor.
Preparing for a Contraction Monitor Reading
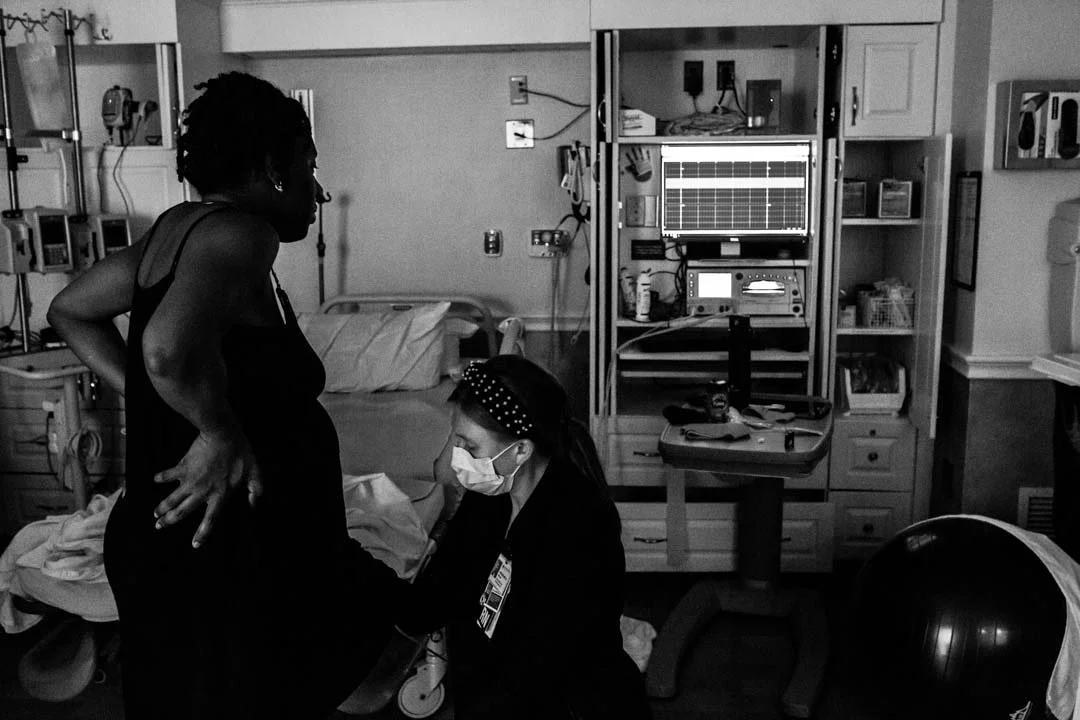
To prepare for a contraction monitor reading, a pregnant woman should consider the following checklist of essential items and follow the proper positioning and comfort guidelines.
Before attending the reading, it is essential to choose a comfortable and quiet space. The space should be away from distractions and noise that might affect the accuracy of the readings. Consider having a supportive partner or family member present for emotional support throughout the process. Also, ensure you have access to your medical history, previous test results, and any relevant medication information.
Proper Positioning
Comfortable positioning during a contraction monitor reading is vital for the accuracy of the readings and for the woman’s emotional well-being. The ideal position involves reclining on a comfortable surface, such as a bed or a cushioned chair, with legs elevated and back supported. A straight or slightly raised back is also recommended to promote good breathing and minimize discomfort. Ensure a wide, stable base for the monitor equipment to enable the healthcare provider to easily manipulate the leads as needed.
Attaching Contraction Monitor Electrodes
The healthcare provider begins by applying a gel or conductive cream to the abdomen to promote a stable connection between the electrode and the skin. A thin strip of the electrode is then attached to the abdomen, usually between the navel and the pubic bone. The strip is held firmly in place using adhesive tape. After attaching the initial electrode, the healthcare provider may attach additional electrodes to the sides or lower abdomen to capture a more comprehensive view of uterine contractions.
Risks of Electrode Irritation or Skin Irritation
Potential risks associated with contraction monitor readings include electrode irritation or skin irritation from the adhesive used to secure the electrode in place. This usually manifests as redness, itching, or mild discomfort where the electrode meets the skin. If the irritation persists or worsens, notify your healthcare provider immediately, as they can adjust the electrode’s placement or recommend alternative solutions.
Operating the Contraction Monitor Device: How To Read Contraction Monitor
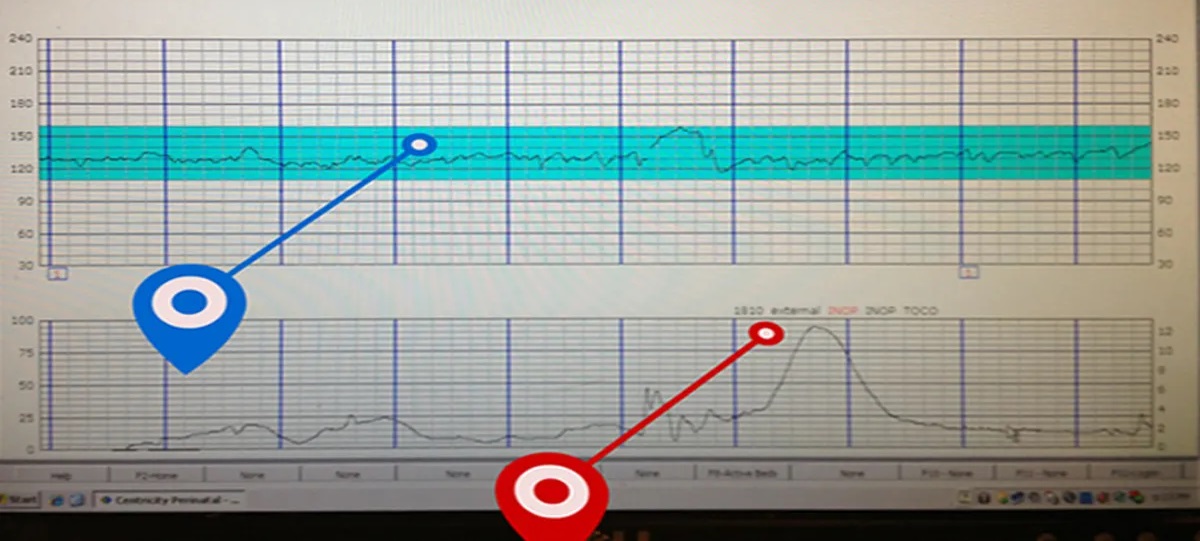
The contraction monitor device is a crucial tool in monitoring fetal wellbeing during pregnancy. It is essential to operate the device correctly to obtain an accurate reading.
The basic components of a contraction monitor device typically include a sensor or electrode that is placed on the mother’s abdomen, a transmitter that sends the data to a display or printer, and a storage system for storing the data. To set up the device for a reading, the healthcare provider will typically attach the sensor to the mother’s abdomen, connect it to the transmitter, and ensure that the device is calibrated correctly.
Components of the Contraction Monitor Device
- The sensor or electrode is typically a small, adhesive patch that is placed on the mother’s abdomen. It detects the fetal heart rate and uterine contractions, and sends the data to the transmitter.
- The transmitter is usually a small device that receives the data from the sensor and sends it to the display or printer. It may also be connected to a storage system for storing the data.
- The storage system is typically a computer or printer that stores the data from the device. It may also be used to print out the fetal heart rate tracing.
The healthcare provider will typically use the monitor to record and display fetal heart rate tracings. These tracings show the changes in the fetal heart rate over a period of time, and are used to determine the fetal wellbeing.
Recording and Displaying Fetal Heart Rate Tracing
The fetal heart rate tracing is typically recorded over a period of time, such as 20-30 minutes. During this time, the device will print out a graph of the fetal heart rate over time. This graph will show the baseline fetal heart rate, as well as any changes in the fetal heart rate over time.
The healthcare provider will use the fetal heart rate tracing to determine the fetal wellbeing. If the tracing shows any signs of distress, such as a decrease in the fetal heart rate or an increase in the uterine contractions, the healthcare provider may take action to ensure the fetal wellbeing.
Interpreting Fetal Heart Rate Tracing
The healthcare provider will typically interpret the fetal heart rate tracing by looking for any signs of distress. This may include a decrease in the fetal heart rate, an increase in the uterine contractions, or any other changes in the tracing.
If the tracing shows any signs of distress, the healthcare provider may take action to ensure the fetal wellbeing. This may include moving the mother to a different position, administering medication, or performing a cesarean section.
Clinical guidelines recommend that healthcare providers use the fetal heart rate tracing to determine the fetal wellbeing, and to take action if the tracing shows any signs of distress.
Understandiong Fetal Heart Rate Patterns
Fetal heart rate (FHR) is a critical indicator of fetal well-being during labor. It is essential to understand the different patterns of FHR to ensure the best possible outcome for both mother and baby.
Fetal heart rate patterns can be classified into three main categories: early decelerations, late decelerations, and variable decelerations.
Early Decelerations
Early decelerations are characterized by a slow, regular decrease in FHR in response to uterine contractions. They are often accompanied by fetal bradycardia, which is a slower than normal heart rate (typically below 110 beats per minute). Early decelerations are typically seen in the second stage of labor and are considered a normal response to fetal stress. Early decelerations can be further divided into two subtypes:
-
Variable decelerations with a slow slope (greater than or equal to 30 seconds)
-
Variable decelerations with a rapid slope (less than 30 seconds)
These are typically seen in the second stage of labor and may indicate fetal distress.
Variable Decelerations
Variable decelerations are characterized by an erratic decrease in FHR that is not uniform and not related to the uterine contraction wave form. They are often accompanied by fetal tachycardia, which is an abnormally fast heart rate (typically above 160 beats per minute). Variable decelerations can be seen in any stage of labor and are often considered a sign of fetal distress. They can be further divided into two subtypes:
-
Short decelerations (lasting less than 30 seconds)
-
Long decelerations (lasting 30 seconds or more)
Variable decelerations can be associated with umbilical cord compression.
Late Decelerations
Late decelerations are characterized by a slow, regular decrease in FHR after the peak of the uterine contraction. They are often accompanied by fetal bradycardia and are considered a sign of fetal distress. Late decelerations can indicate fetal hypoxia, which is a lack of oxygen in the fetus. They can be further divided into two subtypes:
-
Single late deceleration (seen in one uterine contraction)
-
Repetitive late deceleration (seen in multiple uterine contractions)
The presence of late decelerations during labor is a serious indicator of potential fetal distress.
Fetal heart rate patterns can be used to assess fetal well-being by identifying any abnormal patterns that may indicate fetal distress. Abnormal fetal heart rate patterns can be associated with various risks, including:
Fetal distress due to lack of oxygen (hypoxia)
Meconium aspiration syndrome, where the fetus swallows meconium during delivery
Neonatal encephalopathy, which is abnormally low blood glucose, metabolic acidosis, seizures, and/or abnormal muscle tone in the newborn
Fetal heart rate patterns can provide valuable information about fetal well-being during labor, enabling healthcare providers to make informed decisions and take action to ensure the best possible outcome for both mother and baby.
Preparing for a Home Contraction Monitor
Preparing for a home contraction monitor reading is an exciting and crucial step in monitoring your baby’s health during pregnancy. It allows expectant mothers to have a sense of control and reassurance, especially during the later stages of pregnancy. In this section, we will delve into the benefits of home contraction monitoring and the essential steps to prepare for a successful reading.
Benefits of Home Contraction Monitoring, How to read contraction monitor
Home contraction monitoring offers several benefits to expectant mothers, including:
- Convenience: Home contraction monitoring allows mothers to track their baby’s heartbeat from the comfort of their own home, eliminating the need to visit a hospital or clinic repeatedly.
- Increased peace of mind: Monitoring their baby’s heartbeat at home can reduce anxiety and stress associated with uncertainty about their baby’s well-being.
- Early detection of potential issues: Home contraction monitoring can help identify potential issues early on, allowing for prompt medical attention and reducing the risk of complications.
Preparing for a Home Contraction Monitor Reading
To prepare for a home contraction monitor reading, follow these steps:
- Setup and Calibration: Before using the contraction monitor, carefully read and follow the manufacturer’s instructions to ensure proper setup and calibration. It is essential to understand the device’s operation, including how to place the sensors, set the frequency, and adjust the gain.
- Data Transmission: Ensure that the device is connected to a stable power source and that the transmission link is secure and functioning correctly. Regularly check for firmware updates and follow the manufacturer’s guidelines for data transmission and storage.
- Preparation for the Reading: Take a few moments to relax, lie down comfortably, and place the sensors correctly on your abdomen. It is essential to find a quiet and distraction-free space to avoid any noise or disruptions during the reading.
- Understanding the Readings: Familiarize yourself with the contraction monitor’s display and understand the various readings, such as the baseline, acceleration, and deceleration. Take note of any significant changes or unusual patterns in the readings, and consult with your healthcare provider if you have any concerns.
Epilogue
In conclusion, reading a contraction monitor accurately is a skill that can be developed with practice and understanding. By following this guide, you’ll be equipped with the knowledge to interpret fetal heart rate patterns, detect potential complications, and respond effectively to abnormal contraction monitor readings.
Remember, a healthy pregnancy outcome depends on accurate contraction monitoring, so it’s essential to be well-prepared and knowledgeable about this process. By investing time and effort into learning how to read a contraction monitor, you’ll be able to provide crucial support to pregnant women and help ensure a smooth and successful pregnancy journey.
FAQ Guide
Q: What is the purpose of contraction monitoring?
To monitor the fetal heart rate and detect any potential complications in the pregnancy. This process ensures the well-being of the fetus and the mother.
Q: How long does a contraction monitoring test typically take?
Typically, it can take around 30 minutes to an hour to complete, depending on the type of test and the individual’s condition.
Q: What are the potential risks associated with contraction monitoring?
The potential risks include electrode irritation or skin irritation, which can be minimized by following proper preparation and positioning procedures.
Q: Can contraction monitoring be done at home?
Yes, contraction monitoring can be done at home with proper training and equipment.