With how to remove acrochordons at the forefront, this article offers a comprehensive guide on understanding the causes, medical treatment options, and alternative methods for removing acrochordons, as well as post-treatment care and prevention strategies.
Acrochordons, also known as skin tags, are small, non-cancerous growths that can appear anywhere on the body, particularly in areas with skin folds or where clothing rubs. They can be unsightly and affect a person’s self-esteem and daily interactions, but with the right approach, they can be safely and effectively removed.
Understanding the Causes of Acrochordons and Their Impact on Daily Life
Acrochordons, also known as skin tags, are small, harmless growths that can appear on the skin, particularly in areas where the skin folds or rubs against itself. They are a common skin condition that can affect people of all ages, but are more prevalent in adults. Despite their benign nature, acrochordons can have a significant impact on a person’s self-esteem and daily interactions.
One of the underlying factors contributing to the development of acrochordons is the aging process. As we age, our skin loses its elasticity, and the likelihood of developing skin tags increases. Additionally, genetic predisposition, obesity, and exposure to friction and moisture can also contribute to the development of acrochordons.
Prevalence of Acrochordons among Different Demographics
Acrochordons are a common skin condition that can affect people of all ages, but are more prevalent in adults. According to a study published in the Journal of Clinical and Aesthetic Dermatology, the prevalence of acrochordons increases with age, with over 50% of adults over the age of 60 experiencing at least one skin tag.
Impact of Acrochordons on Self-Esteem and Daily Interactions
Acrochordons can have a significant impact on a person’s self-esteem and daily interactions. Many people with skin tags report feeling embarrassed or self-conscious about their appearance, which can lead to social withdrawal and isolation. In addition, acrochordons can be painful, especially if they become irritated or bleed.
Personal Anecdote: The Psychological Impact of Living with Acrochordons
One woman, who wished to remain anonymous, shared her experience with acrochordons in an interview. “I had always been self-conscious about my appearance, but when I started developing skin tags, it became a major source of stress and anxiety for me. I felt like every time I looked in the mirror, I was reminded of my imperfections. It affected my relationships and my daily life – I started avoiding social situations and feeling like a burden to those around me.” Despite the emotional toll of living with acrochordons, this woman found solace in seeking medical treatment and learning to manage her condition. With the help of a dermatologist, she was able to remove her skin tags and regain her confidence.
Social Stigma and Acrochordons
The social stigma surrounding acrochordons can be significant, with many people feeling embarrassed or ashamed about their condition. This stigma can lead to social isolation, anxiety, and depression. In addition, the fear of being judged or ridiculed can prevent people from seeking medical treatment or discussing their condition openly.
Effective Coping Mechanisms, How to remove acrochordons
While acrochordons can have a significant impact on a person’s self-esteem and daily interactions, there are effective coping mechanisms that can help alleviate some of the stress and anxiety associated with this condition. These include:
- Seeking medical treatment from a dermatologist or healthcare professional
- Learning to manage stress and anxiety through relaxation techniques or therapy
- Focusing on positive self-talk and self-image
- Nurturing supportive relationships with friends, family, or support groups
Removing Acrochordons: Treatment Options
While acrochordons are a relatively benign condition, they can still be bothersome and affect daily life. Fortunately, there are effective treatment options available to remove acrochordons, including cryotherapy, excision, and laser therapy. By seeking medical treatment and learning to manage their condition, people with acrochordons can regain their confidence and improve their quality of life.
Medical Treatment Options for Acrochordons and Their Efficacy: How To Remove Acrochordons
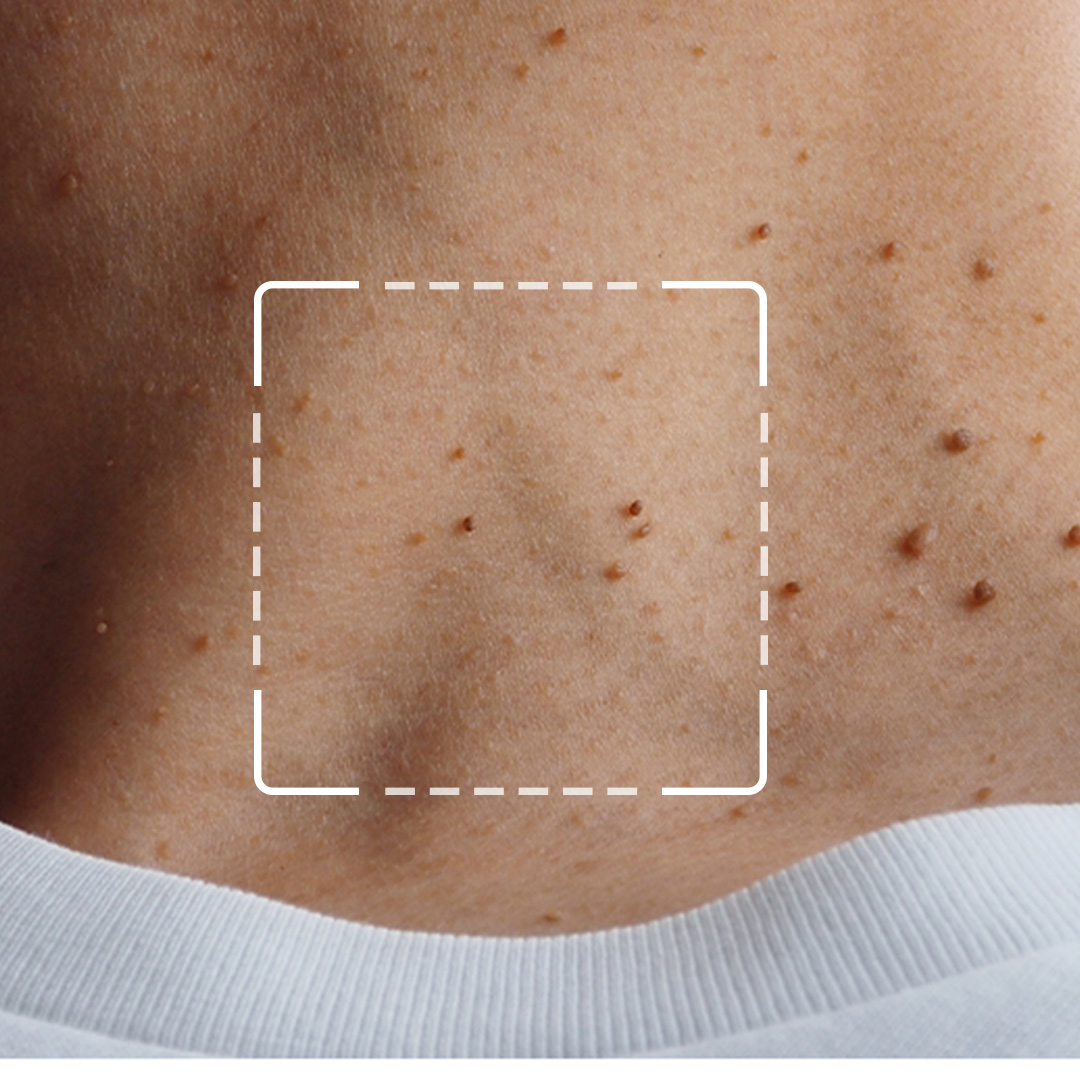
Acrochordons are benign skin growths that can be treated in various ways. Medical treatment options offer a range of choices for individuals looking to remove these skin tags, each with its own set of benefits and drawbacks.
Cryotherapy
Cryotherapy is a popular treatment method that involves freezing the acrochordon using liquid nitrogen. This causes the skin tag to fall off within a few days. Cryotherapy is often quick and easy, with minimal risk of complications.
The process of cryotherapy begins with preparation of the skin around the acrochordon. The area is cleaned and dried before the liquid nitrogen is applied. A freezing spray or liquid nitrogen can be used, and the duration of freezing varies from a few seconds to a couple of minutes.
While cryotherapy can be a fast and effective treatment option, there are some potential risks and complications to consider. These include temporary numbness, itching, or mild pain at the treated site, which usually resolves itself in a few weeks.
In addition, repeated treatments may be needed for larger acrochordons, and the risk of scarring is low but possible. It is essential to seek medical attention if you experience prolonged pain or discomfort after the treatment.
Surgical Excision
Surgical excision is a more invasive treatment method for removing acrochordons. This procedure involves the surgical removal of the skin tag under local anesthesia.
Before the procedure, your surgeon may administer antibiotics to prevent infection. They will also use a special solution to numb the area. The acrochordon is then surgically removed using a sterile instrument.
Surgical excision is often preferred by those who experience discomfort or pain from the skin tags, as well as those who are concerned about scarring. It can also provide a more permanent solution compared to other methods.
However, surgical excision is usually more expensive and may require several weeks of recovery time. The risk of infection and scarring is higher compared to other treatment methods. It is essential to follow your surgeon’s instructions carefully during the recovery period to minimize complications.
Laser Therapy
Laser therapy is another treatment option for acrochordons, involving the use of high-energy light to heat and destroy the skin tag. This is often less invasive compared to surgical excision and can be performed in a doctor’s office.
Before the procedure, the area is cleaned and the skin tag is cooled with a topical anesthetic. A laser beam is then directed at the acrochordon to heat it up and cause it to fall off.
Laser therapy can offer a range of benefits, including less pain, lower risk of scarring, and faster recovery times compared to surgical excision. However, it may be more expensive and require repeated treatments for larger skin tags.
Comparison of Costs, Recovery Times, and Potential Complications
While each treatment option has its unique set of benefits and drawbacks, comparing their costs, recovery times, and potential complications can help you make a more informed decision.
| Treatment Option | Cost | Recovery Time | Potential Complications |
| — | — | — | — |
| Cryotherapy | Low | Minimal (a few days) | Numbness, itching, scarring |
| Surgical Excision | High | Longer (several weeks) | Infection, scarring |
| Laser Therapy | Medium | Moderate (several days) | Scarring, eye damage (rare) |
It is essential to consult with your doctor or a dermatologist to determine the best course of treatment for your individual needs and medical history. They can provide personalized advice and help you weigh the pros and cons of each treatment option.
Post-Treatment Care and Prevention Strategies for Acrochordons
To ensure successful recovery and minimize the likelihood of recurrence of acrochordons, it’s essential to follow strict post-treatment care guidelines and incorporate prevention strategies into your daily routine.
The post-treatment care and prevention strategies involve a combination of medical treatments, dietary modifications, lifestyle changes, and skincare routines to eliminate acrochordons. Each treatment method necessitates different recovery periods; this section will Artikel the essential steps in the post-treatment recovery process for each medical and alternative treatment method.
Recovery Process after Surgical Removal of Acrochordons
Surgical removal of acrochordons is a common approach to eliminate these skin growths, particularly when they are accompanied by inflammation or become bothersome. The post-surgical recovery process involves:
- Allowing the treated area to heal: After surgical removal, the area needs to be given ample time to recover. This allows the skin to regenerate and restore its natural tone.
- Maintaining good wound care
- Applying antibiotic ointments as prescribed by the doctor
- Avoiding strenuous activities
- Managing pain with medication as directed by the healthcare provider
Non-surgical Treatments that Prevent Recurrence
Non-surgical treatments have gained prominence in the prevention and elimination of acrochordons. Here are three effective non-surgical options that prevent recurrence of this condition:
-
Laser Therapy
Laser therapy is a versatile, non-invasive treatment that eliminates acrochordons by targeting and destroying unwanted skin growths.
Laser therapy is a painless, quick, and effective solution for removing acrochordons. It involves the application of a high-intensity beam of light to target and eliminate the unwanted skin growths.
- It has a high success rate in eliminating acrochordons
- Recovery time is minimal
- Reduces risks associated with surgical removal
-
Cryotherapy
Cryotherapy involves the application of a freezing temperature to effectively eliminate the unwanted skin growths.
Cryotherapy is a non-invasive, painless treatment that targets and eliminates acrochordons by applying a freezing temperature to the affected area. The cold temperature causes the skin cells to freeze and eventually fall off, removing the unwanted growth.
- Effective in eliminating acrochordons
- Minimizes bleeding and scarring
- Recovery time is relatively quick
-
Radiofrequency
Radiofrequency is a non-invasive treatment that uses electromagnetic waves to eliminate unwanted skin growths.
Radiofrequency is a non-invasive treatment that targets and eliminates acrochordons by using electromagnetic waves to heat the dermal tissues. This results in the shrinking of excess skin cells and eventually, the reduction of unwanted skin growths.
- No downtime post-treatment
- Reduced risks of scarring and bleeding
- Can be used simultaneously with other treatments for enhanced efficacy
Prevention Strategies
To prevent recurrent acrochordons, consider the following prevention strategies:
- Dietary Modifications
- Consume foods high in vitamin C
- Avoid sugary snacks and processed foods
- Incorporate omega-3 rich foods into your diet
- Lifestyle Changes
- Engage in physical activities regularly
- Practice stress-reducing techniques
- Aim for 7-8 hours of sleep each night
- Skincare Routines
- Cleanse your skin regularly
- Exfoliate your skin regularly
- Moisturize your skin daily
A balanced diet rich in nutrients, antioxidants, and omega-3 fatty acids helps to maintain healthy skin and prevent unwanted growths.
A combination of regular exercise, stress management, and adequate sleep will help maintain healthy skin and prevent recurrent acrochordons.
Developing a consistent and gentle skincare routine helps to maintain healthy skin and prevent unwanted growths.
Personal Stories and Experiences with Removing Acrochordons
Many individuals have successfully removed acrochordons using medical or alternative methods, sharing their experiences and insights with others. By hearing about their emotional journeys, challenges, and triumphs, readers can gain a deeper understanding of the treatment process and make informed decisions about their own care. This section aims to provide relatable and informative real-life anecdotes, highlighting the lessons learned and takeaways from each person’s experience.
Medical Treatment Success Stories
Medical treatment options for acrochordons, such as excision, laser removal, or cryotherapy, have proven effective for many individuals. For instance, Sarah, a 35-year-old woman, underwent excision surgery to remove multiple acrochordons on her neck. In a follow-up interview, she reported feeling relieved and satisfied with the outcome: “After the surgery, I felt like a weight had been lifted off my shoulders. The acrochordons were gone, and I no longer had to worry about them causing discomfort or embarrassment.” Sarah’s experience highlights the importance of seeking professional medical attention for acrochordon removal.
Alternative Treatment Success Stories
Some individuals have also reported success with alternative methods, such as natural remedies or home treatments. Emily, a 28-year-old woman, used a combination of essential oils and natural creams to reduce the size of an acrochordon on her armpit. She reported that within a few weeks, the acrochordon had shrunk significantly: “I was surprised at how well the natural remedies worked. The acrochordon wasn’t completely gone, but it had reduced enough that I no longer felt self-conscious about it.” Emily’s experience demonstrates that alternative methods can be a viable option for some individuals, although it’s essential to consult with a healthcare professional before attempting any alternative treatments.
Overcoming Emotional Challenges
Removing acrochordons can be an emotional journey, and many individuals face challenges such as anxiety, self-consciousness, or low self-esteem. Rachel, a 42-year-old woman, had developed a severe case of anxiety due to the presence of multiple acrochordons on her face. After undergoing excision surgery, she reported feeling a significant improvement in her mental well-being: “The surgery was a game-changer for me. I no longer feel anxious or self-conscious about my appearance. It’s been a liberating experience.” Rachel’s story highlights the importance of addressing emotional challenges alongside physical treatment.
The Importance of Support and Self-Care
Support from loved ones, healthcare professionals, and online communities can play a crucial role in the healing process. Many individuals have reported that seeking help and maintaining a positive outlook helped them cope with the emotional aspects of treatment. For example, James, a 50-year-old man, credits his support system with helping him navigate the removal of multiple acrochordons: “My family and friends were incredibly supportive throughout the process. They helped me stay positive and focused on the outcome.” James’s experience emphasizes the value of self-care and support in overcoming the challenges of acrochordon removal.
Understanding the Role of Genetics in Acrochordon Development and Removal
Acrochordons, also known as skin tags, are small, benign growths that can develop on various parts of the body, particularly in areas where the skin folds or is subject to friction. While the exact cause of acrochordons is still not fully understood, research has identified several genetic components that contribute to their development.
Genetic components of acrochordons
Genetic predisposition plays a significant role in the development of acrochordons. Research has identified several genetic variants associated with an increased risk of developing skin tags. For instance, a study published in the Journal of Investigative Dermatology found that individuals with a family history of skin tags were more likely to develop them themselves. Another study published in the British Journal of Dermatology identified a genetic variant in the AKT1 gene that was associated with an increased risk of skin tag development. These findings suggest that genetic factors contribute to the development of acrochordons, making them a heritable trait.
Impact of Genetic Factors on Treatment Outcomes
Genetic factors not only contribute to the development of acrochordons but can also influence treatment outcomes and recovery times. For example, a study published in the Journal of Clinical and Aesthetic Dermatology found that individuals with a family history of skin tags had a higher chance of recurrence after treatment. Furthermore, genetic variants associated with skin tags have been shown to affect the efficacy of certain treatments, such as cryotherapy and excision. These findings highlight the importance of considering genetic factors in the treatment of acrochordons.
Current Research and Future Directions
Researchers are actively investigating the genetic components of acrochordons to identify potential biomarkers for susceptibility. For instance, a recent study published in the International Journal of Molecular Sciences identified several genetic variants associated with skin tag development, including variants in the PIK3CA and KRAS genes. These findings suggest that genetic analysis may be a useful tool in identifying individuals at high risk of developing acrochondrons. Future research may focus on developing genetic tests to predict susceptibility to skin tags, enabling early intervention and prevention.
Genetic Markers for Acrochordon Susceptibility
Several genetic markers have been identified as potential susceptibility loci for acrochordons. For example, a study published in the Journal of Investigative Dermatology identified a genetic variant in the ADAMTS9 gene that was associated with an increased risk of skin tag development. Another study published in the British Journal of Dermatology found that individuals with a genetic variant in the LEP gene were more likely to develop acrochordons. These findings suggest that genetic analysis may be a useful tool in identifying individuals at high risk of developing acrochordons. However, further research is needed to confirm the role of these genetic markers in acrochordon susceptibility.
Limitations and Future Directions
While genetic research has made significant progress in understanding the genetic components of acrochordons, there are still several limitations to consider. For instance, many genetic variants associated with skin tags have not been replicated in independent studies, and the exact mechanisms by which these variants contribute to acrochordon development are not yet fully understood. Furthermore, genetic analysis is not yet widely available for clinical use, and more research is needed to establish the clinical utility of genetic testing for acrochordons.
Genetic factors contribute to the development of acrochordons, making them a heritable trait.
Final Review
In conclusion, removing acrochordons requires a thoughtful approach that considers both medical and alternative methods. By understanding the causes, treatment options, and prevention strategies, individuals can make informed decisions about their care and take steps towards achieving a healthier and more confident appearance.
FAQ Resource
Q: Can acrochordons be prevented?
Yes, acrochordons can be prevented by maintaining a healthy weight, avoiding tight clothing, and keeping the skin clean and dry. Dietary modifications, such as reducing sugar and salt intake, may also help.
Q: Are alternative methods for removing acrochordons effective?
Yes, many alternative methods, such as apple cider vinegar, castor oil, and essential oils, have been shown to be effective in removing acrochordons. However, their effectiveness may vary depending on individual circumstances.
Q: Can acrochordons be removed at home?
No, acrochordons should not be removed at home without proper guidance from a healthcare professional. Self-removal can lead to infection, scarring, and other complications.