How to stay in sinus rhythm after cardioversion is a crucial aspect of maintaining overall cardiovascular health and preventing complications. The narrative unfolds in a compelling and distinctive manner, drawing readers into a story that promises to be both engaging and uniquely memorable, and provides a comprehensive overview of the topic.
The importance of maintaining sinus rhythm after cardioversion cannot be overstated, as it directly affects the overall cardiovascular health. Electrocardiogram testing plays a significant role in identifying underlying cardiac conditions that may impact sinus rhythm post-conversion, and optimizing medication regimens and addressing comorbidities before proceeding with cardioversion is crucial.
Understanding the Importance of Maintaining Sinus Rhythm After Cardioversion
Maintaining sinus rhythm after cardioversion is crucial for the overall cardiovascular health of an individual. Cardioversion is a medical procedure that converts an abnormal heart rhythm, known as arrhythmia, to a normal sinus rhythm. However, it is essential to maintain this normal rhythm after the procedure to prevent complications and ensure optimal cardiac function.
When sinus rhythm is not maintained after cardioversion, it can lead to various complications, including increased risk of thrombosis and cardiac arrhythmias. Thrombosis occurs when a blood clot forms in the heart, which can lead to a heart attack or stroke. Cardiac arrhythmias, on the other hand, can cause a range of symptoms, including palpitations, shortness of breath, and fatigue. In severe cases, cardiac arrhythmias can lead to cardiac arrest or even death.
Tachycardia: A Potential Complication of Sinus Rhythm Loss
Tachycardia is a common complication of sinus rhythm loss, characterized by a rapid heart rate exceeding 100 beats per minute. This can lead to decreased cardiac output, resulting in symptoms such as dizziness, lightheadedness, and shortness of breath.
Bradycardia: A Potential Complication of Sinus Rhythm Loss, How to stay in sinus rhythm after cardioversion
Bradycardia, on the other hand, is characterized by a slow heart rate, typically below 60 beats per minute. This can lead to decreased cardiac output, resulting in symptoms such as fatigue, weakness, and shortness of breath.
Increased Risk of Thrombosis
The loss of sinus rhythm can increase the risk of thrombosis, as the abnormal heart rhythm can cause blood to pool in the heart, leading to the formation of blood clots. If these clots break loose, they can travel to other parts of the body, such as the brain or lungs, causing a stroke or pulmonary embolism.
Cardiac Arrhythmias
Cardiac arrhythmias are a common complication of sinus rhythm loss, characterized by an abnormal heart rhythm that can be too fast or too slow. These arrhythmias can range from mild symptoms to life-threatening conditions, such as ventricular fibrillation or cardiac arrest.
Post-Conversion Care and Monitoring for Sinus Rhythm
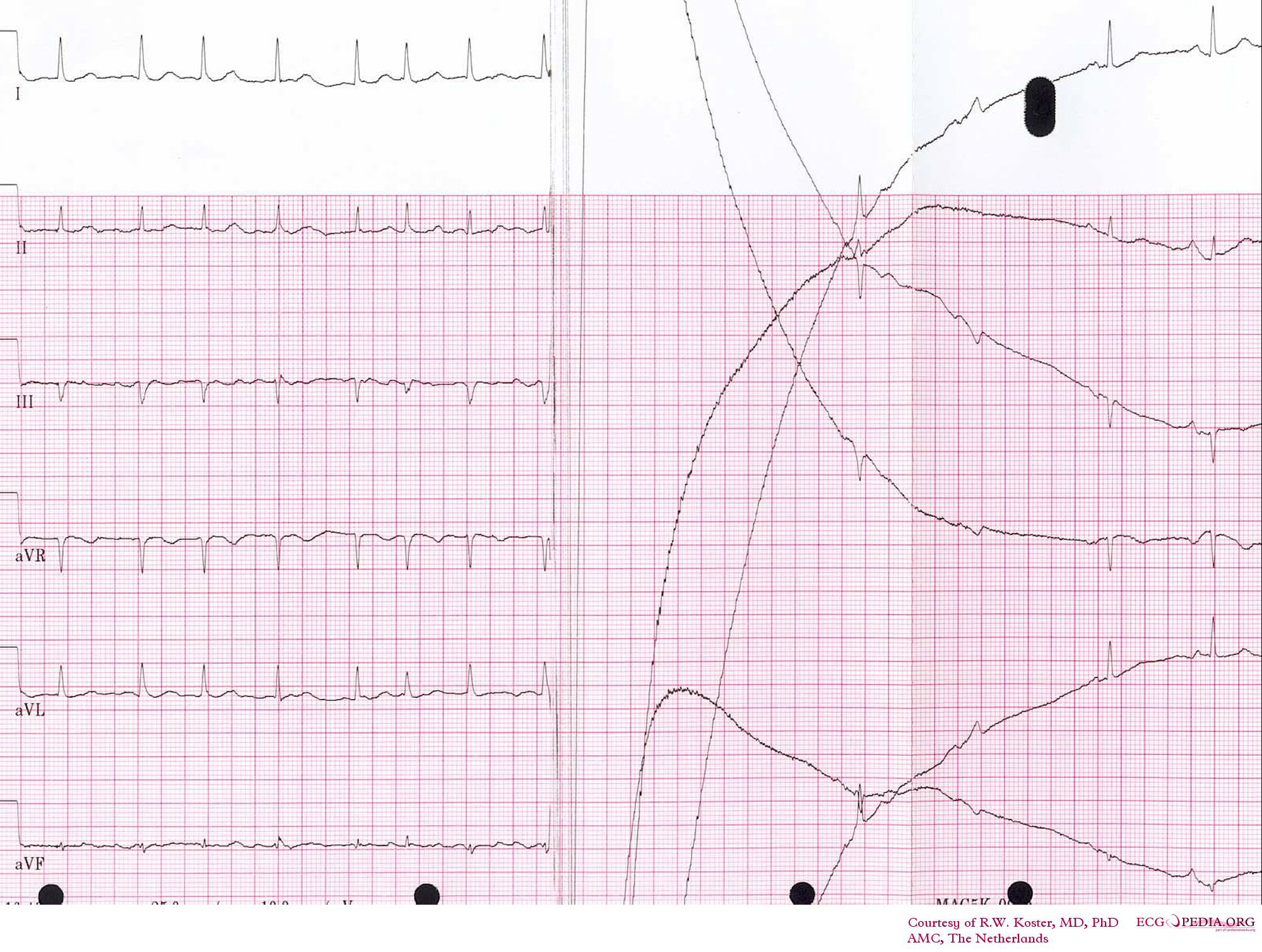
Ensuring a stable and sustained sinus rhythm after cardioversion requires attentive post-conversion care and monitoring. Close observation and regular assessments enable healthcare providers to promptly identify and address potential complications, thereby minimizing the risk of adverse outcomes and facilitating optimal patient recovery.
Essential Components of Post-Conversion Care
Post-conversion care involves a comprehensive approach to monitoring and managing the patient’s recovery. The essential components of post-conversion care include:
- Continuous Electrocardiogram (ECG) Monitoring: Continuous ECG monitoring is crucial for detecting any arrhythmias or abnormal heart rhythms that may occur after cardioversion. This monitoring enables healthcare providers to intervene promptly in case of any irregularities, thereby preventing potential complications.
- Regular Blood Work: Regular blood work includes routine blood tests to monitor the patient’s electrolyte levels, cardiac enzymes, and liver function. This monitoring ensures that the patient’s physiological processes are functioning within the normal range, thereby minimizing the risk of cardiac dysfunction or other systemic complications.
- Close Monitoring of Vital Signs: Close monitoring of vital signs, including blood pressure, heart rate, and oxygen saturation, is essential for detecting any potential complications. This monitoring enables healthcare providers to promptly address any abnormalities, thereby preventing potential adverse outcomes.
- Assessment of Cardiac Function: Assessment of cardiac function includes evaluating the patient’s left ventricular ejection fraction, cardiac output, and other relevant parameters. This monitoring ensures that the patient’s cardiac function is within the normal range, thereby minimizing the risk of cardiac dysfunction or other systemic complications.
- Patient Education and Support: Patient education and support are crucial for ensuring that patients understand the importance of post-conversion care and monitoring. This education enables patients to recognize potential complications and take prompt action to prevent adverse outcomes.
Significance of Monitoring for Potential Complications
Monitoring for potential complications is essential for preventing adverse outcomes and ensuring optimal patient recovery. Some of the potential complications that may arise after cardioversion include:
- Bleeding Complications: Bleeding complications, including hemopericardium and cardiac tamponade, may occur after cardioversion due to the anticoagulation therapy used to prevent thromboembolism. Close monitoring of vital signs and regular blood work can help detect potential bleeding complications.
- Infection Complications: Infection complications, including endocarditis and pericarditis, may occur after cardioversion due to the catheter-based procedures. Close monitoring of vital signs and regular blood work can help detect potential infection complications.
- Cardiac Dysfunction Complications: Cardiac dysfunction complications, including heart failure and cardiac arrest, may occur after cardioversion due to the stress of the procedure. Close monitoring of vital signs and regular blood work can help detect potential cardiac dysfunction complications.
Prevention of Complications
Prevention of complications is essential for ensuring optimal patient recovery and minimizing the risk of adverse outcomes. Some of the strategies that can be used to prevent complications include:
- Early Detection and Intervention: Early detection and intervention of potential complications can help prevent adverse outcomes. Close monitoring of vital signs and regular blood work can help detect potential complications.
- Optimal Anticoagulation Management: Optimal anticoagulation management is essential for preventing thromboembolism and minimizing the risk of bleeding complications. Close monitoring of international normalized ratio (INR) levels can help ensure optimal anticoagulation management.
- Proper Post-Conversion Care: Proper post-conversion care, including continuous ECG monitoring and regular blood work, can help prevent complications and ensure optimal patient recovery.
Managing Medications to Maintain Sinus Rhythm
Adjusting medication regimens post-cardioversion is crucial to minimize the risk of arrhythmias and promote sustained sinus rhythm. The goal of this adjustment is to ensure that the patient’s medication regimen effectively manages the underlying cause of the arrhythmia, preventing recurrence and promoting long-term sinus rhythm. Effective management of medications post-cardioversion requires close collaboration between the patient, the patient’s healthcare provider, and other healthcare professionals involved in the patient’s care.
Role of Anti-arrhythmic Medications
Anti-arrhythmic medications are a crucial component of managing medications post-cardioversion to maintain sinus rhythm. These medications work by altering the electrical activity of the heart to prevent arrhythmias. There are four main classes of anti-arrhythmic medications: Class I (sodium channel blockers), Class II (beta blockers), Class III (potassium channel blockers), and Class IV (calcium channel blockers). Each class of medication has a different mechanism of action and is used to treat specific types of arrhythmias.
- Class I Anti-arrhythmic Medications
- Class II Anti-arrhythmic Medications
- Class III Anti-arrhythmic Medications
- Class IV Anti-arrhythmic Medications
Class I medications, also known as sodium channel blockers, work by inhibiting the sodium channels in the heart. This inhibition reduces the conduction velocity of the electrical impulse through the heart, thereby preventing arrhythmias. However, Class I medications can have significant side effects, including QT prolongation and torsades de pointes.
Class II medications, also known as beta blockers, work by blocking the effects of epinephrine (adrenaline) on the heart. By blocking epinephrine, Class II medications reduce the heart rate and the force of contraction, thereby reducing the electrical activity of the heart. Common side effects of Class II medications include fatigue, dizziness, and shortness of breath.
Class III medications, also known as potassium channel blockers, work by inhibiting the potassium channels in the heart. This inhibition prolongs the action potential and refractory period of the cardiac myocytes, thereby preventing arrhythmias. Common side effects of Class III medications include QT prolongation and torsades de pointes.
Class IV medications, also known as calcium channel blockers, work by blocking the effects of calcium on the heart. By blocking calcium, Class IV medications reduce the contractility of the heart muscle, thereby reducing the electrical activity of the heart. Common side effects of Class IV medications include peripheral edema, headaches, and dizziness.
Side Effects of Anti-arrhythmic Medications
While anti-arrhythmic medications are effective in managing arrhythmias, they can have significant side effects. The most common side effects include:
- QT prolongation: This is a condition where the QT interval (the time between the Q and T waves on the electrocardiogram) is longer than normal.
- Torsades de pointes: This is a type of arrhythmia that can lead to ventricular fibrillation and sudden cardiac death.
- Bradyarrhythmias: This is a condition where the heart rate is slower than normal.
- Cardiac failure: This is a condition where the heart is unable to pump enough blood to meet the body’s needs.
These side effects can be severe and even life-threatening. Therefore, it is essential to closely monitor patients taking anti-arrhythmic medications and adjust their regimens as necessary to minimize the risk of side effects.
Minimizing the Risk of Recurrence with Sinus Rhythm Maintenance Strategies: How To Stay In Sinus Rhythm After Cardioversion
Regular follow-up appointments and electrocardiogram (ECG) monitoring are crucial for identifying potential issues early on in maintaining sinus rhythm after cardioversion. The importance of close monitoring cannot be overstated, as it enables healthcare providers to promptly address any concerns that may arise, thereby reducing the risk of recurrence and promoting optimal health outcomes.
Regular Follow-up Appointments
Regular follow-up appointments with a healthcare provider are essential for ensuring that individuals who have undergone cardioversion continue to maintain sinus rhythm. During these appointments, the healthcare provider will assess the individual’s overall health, perform an ECG, and discuss any concerns or questions that the individual may have. Regular follow-up appointments also provide an opportunity for healthcare providers to make any necessary adjustments to medications or other treatments to prevent recurrence.
- Monitoring ECG results to identify potential issues early on
- Assessing overall health and making recommendations for lifestyle modifications
- Addressing concerns or questions from the individual
- Adjusting medications or other treatments as needed to prevent recurrence
Electrocardiogram Monitoring
ECG monitoring is a vital component of maintaining sinus rhythm after cardioversion. This non-invasive test uses sensors to track the electrical activity of the heart and can help identify potential issues before they become serious. ECG monitoring can be performed in a healthcare provider’s office, at home, or through a portable device.
- Providing a detailed picture of the heart’s electrical activity
- Enabling healthcare providers to identify potential issues early on
- Allowing for prompt treatment of any concerns that may arise
- Reducing the risk of recurrence and promoting optimal health outcomes
Cardiac Device Implantation
Cardiac device implantation, such as pacemakers and implantable cardioverter-defibrillators (ICDs), can play a vital role in preventing arrhythmias and maintaining sinus rhythm. These devices can be used in individuals who have a history of atrial fibrillation or other arrhythmias, and can help regulate the heartbeat and prevent recurrence.
- Pacemakers: used to regulate the heartbeat in individuals with bradycardia (slow heart rate)
- ICDs: used to detect and treat life-threatening arrhythmias, such as ventricular fibrillation
- Reducing the risk of recurrence and promoting optimal health outcomes
- Providing peace of mind for individuals who have a history of arrhythmias
Importance of Cardiac Device Implantation
Cardiac device implantation can be a lifesaving treatment for individuals who have a history of arrhythmias. By regulating the heartbeat and preventing recurrence, cardiac devices can help reduce the risk of stroke, heart failure, and other complications associated with atrial fibrillation and other arrhythmias. Furthermore, cardiac devices can provide peace of mind for individuals who have a history of arrhythmias, allowing them to live a more active and fulfilling life.
The American Heart Association estimates that cardiac devices have reduced the risk of death from heart rhythm disorders by 50% over the past decade.
Closing Notes
By following the Artikeld guidelines and strategies, individuals can significantly reduce the risk of arrhythmias and maintain sinus rhythm. Regular follow-up appointments, electrocardiogram monitoring, and cardiac device implantation are essential for identifying potential issues early and preventing complications. Ultimately, staying in sinus rhythm after cardioversion requires a multidisciplinary approach, and it is crucial to be proactive and adhere to post-conversion care and monitoring recommendations.
Top FAQs
Q: What are the most common medications used to maintain sinus rhythm after cardioversion?
A: Anti-arrhythmic medications such as beta-blockers, calcium channel blockers, and anti-arrhythmic agents are commonly used to maintain sinus rhythm after cardioversion. However, the choice of medication depends on individual patient needs and medical history.
Q: How can stress management techniques help maintain sinus rhythm?
A: Stress management techniques such as meditation, yoga, and deep breathing exercises can help manage stress and anxiety, which are risk factors for arrhythmias and sinus rhythm disturbances. Regular practice can lead to improved cardiovascular health and reduced stress levels.
Q: What is the role of echocardiography in assessing cardiac structure and function post-conversion?
A: Echocardiography allows for non-invasive assessment of cardiac structure and function, enabling healthcare professionals to evaluate the heart’s anatomy and detect any potential issues. This can help identify patients at risk for complications and guide post-conversion care.
Q: Can lifestyle changes and behavioral modifications prevent complications?
A: Yes, incorporating lifestyle changes such as a balanced diet, regular physical activity, and stress management techniques can help maintain sinus rhythm and prevent complications by promoting overall cardiovascular health.
Q: What is the importance of regular follow-up appointments and electrocardiogram monitoring?
A: Regular follow-up appointments and electrocardiogram monitoring are crucial for identifying potential issues early and preventing complications. This close monitoring enables healthcare professionals to adjust treatment plans as needed, minimizing the risk of arrhythmias and maintaining sinus rhythm.