Delving into how to tell if you have hemorrhoids, this introduction immerses readers in a unique and compelling narrative, with a dash of American pop culture style that’s both engaging and thought-provoking from the very first sentence. So, let’s get started.
The symptoms of hemorrhoids can be subtle, but they’re often a mix of itching, pain, swelling, and rectal bleeding. To determine if you have hemorrhoids, it’s essential to know the risk factors and contributing conditions, including a diet high in processed foods, low in fiber, and excessive consumption of processed meat. Additionally, chronic constipation, pregnancy, and prolonged sitting can also contribute to hemorrhoid development.
Recognizing the Symptoms of Hemorrhoids
Are you experiencing a burning sensation down there? Before you rush to the toilet, let’s get to know our friend hemorrhoids. Hemorrhoids are like those pesky relatives that you only meet when they want money or a favor, but unlike them, hemorrhoids will only visit when they want to cause you pain and discomfort. So, how do you know if you’re hosting these unwanted guests?
Common Symptoms of Hemorrhoids
When hemorrhoids appear, they can bring a variety of symptoms, which can be quite painful. Here are some common symptoms you might experience:
- Itching around the anus: Imagine the sensation of sitting on a thorn, but instead of just a thorn, it’s a big cluster of thorns, and they’re all itching at the same time. Ouch!
- Pain or discomfort while sitting: Hemorrhoids can make sitting feel like you’re on a bed of nails. No, it’s not just the couch that’s been set up for torture!
- Bleeding during bowel movements: Yes, you read that right – bleeding. Imagine a tiny faucet that’s been turned on, and the only way to stop the bleeding is to… well, you get the idea.
- Swelling or lumps around the anus: They’re like little volcanoes waiting to erupt, but instead of lava, they’ll just ooze out, and you’ll be left with a mess.
- Discharge or mucus: It’s like your body is trying to tell you, “Hey, I’ve got a problem here!
It’s essential to know that hemorrhoid symptoms can vary depending on the type and stage of hemorrhoid development. For instance, external hemorrhoids might cause pain and swelling, while internal hemorrhoids might not be so noticeable but can still cause bleeding.
Now, you might be wondering, “How can I tell if it’s just hemorrhoids and not something more serious?” Well, it’s crucial to distinguish hemorrhoid symptoms from other rectal problems, such as abscesses and fistulas. These issues can be just as painful and discomforting, but they require different treatment. Think of it like this: just because you have a headache, it doesn’t mean you have a brain tumor. You get a check-up, a diagnosis, and then a treatment plan. Same thing here.
The takeaway is that knowing your body and its little quirks is crucial. If you notice any of these symptoms, don’t be afraid to visit a doctor. Trust me, it’s better to be safe than sorry. After all, a healthy butt is a happy butt!
Identifying Risk Factors and Contributing Conditions
A diet consisting mainly of processed foods can lead to an increased risk of developing hemorrhoids. These foods often lack essential nutrients, such as fiber, and can cause strain on the digestive system, which may contribute to hemorrhoid development.
A diet high in processed foods, low in fiber, and excessive consumption of processed meat has been linked to an increased risk of developing hemorrhoids. Processed foods can cause constipation, which can lead to straining during bowel movements, thereby increasing the pressure on the veins in the rectum.
The Impact of Diet on Hemorrhoid Development
A diet rich in fiber can help to maintain healthy bowel movements and reduce the pressure on the veins in the rectum. Foods high in fiber, such as fruits, vegetables, and whole grains, can help to soften stool and make it easier to pass, reducing the risk of constipation and straining during bowel movements.
On the other hand, a diet high in processed foods can lead to constipation, which can cause hemorrhoids to form. Processed foods often contain low amounts of fiber and high amounts of sugar and salt, which can cause the body to absorb more water and lead to hard, dry stools that are difficult to pass.
The excessive consumption of processed meat has also been linked to an increased risk of developing hemorrhoids. Processed meat is often high in sodium and low in fiber, which can cause the body to retain more water and lead to swelling in the rectum, thereby increasing the pressure on the veins and increasing the risk of hemorrhoid formation.
When it comes to hemorrhoids, people often think they’ll just disappear on their own or that they’re a minor nuisance. Unfortunately, left untreated or poorly managed, hemorrhoids can lead to some serious complications. In this chapter, we’ll explore the potential complications of hemorrhoids and how they can compromise your quality of life.
Anal Fissures: A Painful Consequence of Hemorrhoids
An anal fissure is a small tear in the lining of the anus. It can be incredibly painful and may cause bleeding or itching. Anal fissures can occur when a hemorrhoid becomes severely thrombosed (blood clots) or when the skin around the anus becomes irritated from constant straining during bowel movements. Symptoms of anal fissures include intense pain during and after bowel movements, as well as a small amount of bright red blood on the stool or toilet paper.
- Painful bowel movements, ranging from mild discomfort to severe pain that can persist for several days.
- Bleeding, which may appear as a small amount of bright red blood on the stool or toilet paper.
- Prolonged symptoms, as anal fissures can take several weeks to several months to heal.
In severe cases, anal fissures can result in chronic pain, decreased quality of life, and even the inability to engage in regular physical activities.
Perianal Abscesses: A Serious Complication of Hemorrhoids
A perianal abscess is a pocket of pus that forms near the anus. It can occur when bacteria enter the body through a small crack or tear in the skin. Perianal abscesses can be extremely painful and may cause swelling, redness, and discharge. Symptoms of perianal abscesses include intense pain, swelling around the anal region, and a foul-smelling discharge.
- Pus-filled abscesses that may rupture, causing an intense, sharp pain.
- Swelling around the anal region, which can be tender to the touch.
- Foul-smelling discharge that may contain blood or pus.
Perianal abscesses can lead to infection, abscess rupture, or even chronic conditions like Crohn’s disease or ulcerative colitis.
Rectal Prolapse: A Compromised Quality of Life
Rectal prolapse occurs when the rectum loses its normal attachment inside the body, causing it to protrude through the anus. This can be caused by straining due to hemorrhoids, constipation, or other conditions. Symptoms of rectal prolapse include a feeling of incomplete bowel movements, rectal discomfort, and visible protrusion through the anus.
- Feeling of incomplete bowel movements, as if stool is still in the rectum after passing.
- Rectal discomfort, pain, or pressure, especially during bowel movements.
- Visible protrusion through the anus of the rectum or anus itself.
Rectal prolapse can lead to difficulty with bowel movements, chronic pain, and decreased self-esteem due to visible symptoms.
The Psychological Impact of Living with Hemorrhoids
Hemorrhoids can not only cause physical discomfort but also have a profound psychological impact. Living with constant pain, itching, or bleeding can lead to anxiety, depression, and body image issues. The fear of being alone during bowel movements or avoiding social activities due to symptoms can exacerbate these feelings. In some cases, people may feel embarrassed, ashamed, or frustrated by their condition, leading to a negative self-image.
Living with hemorrhoids is not just about treating the physical symptoms but also addressing the emotional and psychological impact.
Lifestyle Modifications for Prevention and Management: How To Tell If You Have Hemorrhoids
Lifestyle modifications play a significant role in preventing and managing hemorrhoids. By incorporating simple changes into your daily routine, you can reduce the risk of developing hemorrhoids and alleviate symptoms if they occur.
A balanced diet rich in high-fiber foods, fruits, and vegetables is essential for maintaining good digestive health.
High-Fiber Foods in Your Diet
Foods high in fiber help promote regular bowel movements and prevent constipation, which is a common cause of hemorrhoids. Include the following high-fiber foods in your diet:
- Legumes such as lentils, chickpeas, and black beans, which are rich in both fiber and protein
- Leafy green vegetables like spinach, broccoli, and Brussels sprouts, which are rich in fiber and antioxidants
- Nuts and seeds, including almonds, chia seeds, and flaxseeds, which are high in fiber and healthy fats
- Fruits like apples, berries, and pears, which are rich in fiber, vitamins, and antioxidants
Regular physical activity is also crucial for maintaining good digestive health and preventing constipation. Regular exercise can help stimulate bowel movements and improve the overall function of the digestive system.
Regular Exercise
Incorporate the following exercises into your daily routine to help prevent and manage hemorrhoids:
- Walking: Aim for at least 30 minutes of brisk walking per day to promote regular bowel movements
- Yoga: Practice gentle yoga poses, such as forward bends and pelvic tilts, to help relax the pelvic muscles and improve digestion
- Pelvic floor exercises: Perform Kegel exercises to strengthen the muscles in the pelvic floor and improve bladder control and digestion
Stress can exacerbate hemorrhoid symptoms and make them more uncomfortable. Practicing stress-reducing techniques can help alleviate symptoms and improve overall well-being.
Stress-Reducing Techniques
Try the following stress-reducing techniques to help manage hemorrhoid symptoms:
- Meditation: Practice mindfulness meditation or guided meditation to calm the mind and reduce stress
- Deep breathing: Engage in deep breathing exercises to slow down the heart rate and promote relaxation
- Therapy: Consider seeking professional help from a therapist or counselor to address stress and anxiety related to hemorrhoids
Treating Hemorrhoids with Medications, Creams, and Ointments
Treating hemorrhoids requires a multi-faceted approach that often involves medications, creams, and ointments to alleviate symptoms and prevent further complications. In this section, we will delve into the various types of medications and creams available, as well as their potential side effects and interactions.
Pain Relief Medications
Pain relief medications are often the go-to solution for individuals suffering from hemorrhoids. Pain relievers such as acetaminophen (Tylenol) or ibuprofen (Advil) can help reduce discomfort and inflammation. However, it is essential to note that these medications should be used under the guidance of a healthcare professional and in moderation.
- Acetaminophen (Tylenol): A common over-the-counter pain reliever that can help alleviate mild to moderate pain associated with hemorrhoids.
- Ibuprofen (Advil): A nonsteroidal anti-inflammatory drug (NSAID) that can help reduce inflammation and pain.
- Codeine: A stronger pain reliever that may be prescribed for severe hemorrhoid discomfort, but it can have side effects such as drowsiness and constipation.
Anti-Inflammatory Creams and Ointments
Anti-inflammatory creams and ointments can help reduce swelling, itching, and discomfort associated with hemorrhoids. Some popular options include topical creams and ointments that contain witch hazel, hydrocortisone, or lidocaine.
- Witch hazel: A natural astringent that can help reduce swelling and itching.
- Hydrocortisone: A topical steroid that can help reduce inflammation and itching.
- Lidocaine: A topical anesthetic that can help numb the area and reduce pain.
Potential Side Effects and Interactions
While medications and creams can be effective in managing hemorrhoid symptoms, they can also have side effects and interactions. It is crucial to consult with a healthcare professional before trying any new medications or creams, especially if you are taking other medications or have underlying medical conditions.
Symptoms of potential side effects may include:
- Drowsiness or fatigue
- Stomach upset or nausea
- Diarrhea or constipation
- Interactions with other medications, such as blood thinners or antacids
Nonsurgical Treatments for Hemorrhoids
Nonsurgical treatments for hemorrhoids are designed to alleviate symptoms and prevent complications without the need for surgery. These options are often used as an alternative to more invasive procedures or as a precursor to surgical interventions. In this section, we will explore three nonsurgical treatments for hemorrhoids: rubber band ligation, sclerotherapy, and cryotherapy.
Rubber Band Ligation
Rubber band ligation is a procedure used to treat internal hemorrhoids. It involves placing a rubber band around the base of the hemorrhoid, cutting off its blood supply and preventing further bleeding. The procedure is typically performed in a doctor’s office and takes only a few minutes to complete.
Here’s how rubber band ligation works:
- First, the doctor will use a special tool to guide a rubber band onto the base of the hemorrhoid.
- The rubber band is placed around the base of the hemorrhoid, cutting off its blood supply.
- Over time, the hemorrhoid will shrink and eventually fall off on its own.
Sclerotherapy
Sclerotherapy is another nonsurgical treatment for hemorrhoids. It involves injecting a solution into the hemorrhoid, which causes it to shrink and eventually disappear. The solution used in sclerotherapy is usually a chemical that irritates the skin and causes scarring, but it’s a safer alternative to surgery.
Here’s how sclerotherapy works:
- First, the doctor will cleanse the area around the hemorrhoid and administer a local anesthetic to minimize discomfort.
- The doctor will then insert a needle into the hemorrhoid and inject the solution.
- The solution will cause the hemorrhoid to shrink and eventually disappear over time.
Cryotherapy
Cryotherapy is a procedure that involves freezing off hemorrhoids using liquid nitrogen. The cold temperature causes the hemorrhoid to shrink and eventually fall off on its own. Cryotherapy is a relatively new treatment for hemorrhoids and has shown promising results in reducing pain and discomfort.
Here’s how cryotherapy works:
- First, the doctor will cleanse the area around the hemorrhoid and administer a local anesthetic to minimize discomfort.
- The doctor will then apply liquid nitrogen to the hemorrhoid using a special applicator.
- The liquid nitrogen will cause the hemorrhoid to freeze and eventually fall off on its own.
Surgical Treatment Options for Hemorrhoids
When conservative treatments fail to alleviate the symptoms of hemorrhoids, surgical intervention becomes a viable option. This chapter explores the available surgical treatments for hemorrhoids, highlighting the procedures, risks, and potential complications.
Hemorrhoidectomy
A hemorrhoidectomy is a surgical procedure that involves the removal of hemorrhoids. This is typically performed under general anesthesia or local anesthesia with sedation. During the procedure, the surgeon will make an incision around the anal opening and remove the affected hemorrhoid using a technique called excision. Once the hemorrhoid is removed, the incision is closed with stitches, and the area is left to heal.
Stapled Hemorrhoidopexy, How to tell if you have hemorrhoids
Stapled hemorrhoidopexy, also known as hemorrhoid stapling, is a minimally invasive procedure that involves the staple removal of hemorrhoids in a few minutes. This procedure is typically performed under general anesthesia or local anesthesia with sedation. During the procedure, the surgeon will insert a specialized stapling device into the rectum and staple the hemorrhoids to reposition them.
Potential Risks and Complications of Surgical Treatments
While surgical treatments can be effective in alleviating the symptoms of hemorrhoids, they do carry certain risks and complications. These may include:
- Postoperative bleeding: There is a risk of bleeding after surgery, which may require further treatment.
- Anal stricture: The anal sphincter may become narrow or narrow during the healing process, which can cause difficulties during bowel movements.
- Pain and discomfort: Pain and discomfort are common during the recovery period after surgical treatments.
- Infection: As with any surgical procedure, there is a risk of infection after hemorrhoid surgery.
It is essential to discuss the potential risks and complications with a healthcare professional before undergoing any surgical treatment. Regular follow-up appointments and adherence to postoperative instructions can help minimize the risk of complications and ensure a smooth recovery.
Alternative Therapies and Natural Remedies
Alternative therapies and natural remedies offer a complementary approach to managing hemorrhoids, often used in conjunction with conventional treatments. These remedies focus on alleviating symptoms, promoting healing, and preventing further complications. From herbal remedies to acupuncture, alternative therapies can provide relief and enhance overall well-being.
Herbal Remedies for Hemorrhoids
Herbal remedies have been used for centuries to treat various health conditions, including hemorrhoids. Two popular herbs, psyllium and aloe vera, have been shown to provide relief from hemorrhoid symptoms.
– Psyllium is a soluble fiber that helps soften stool, reduce constipation, and promote bowel movements. It absorbs excess water in the gut, which reduces inflammation and discomfort associated with hemorrhoids. The recommended dosage is one to two tablespoons per day, mixed with water or other liquids.
– Aloe vera is known for its anti-inflammatory and soothing properties, which can help reduce swelling, itching, and pain in hemorrhoids. Aloe vera gel can be applied topically to the affected area using a cotton swab or finger.
The benefits of herbal remedies lie in their natural, gentle approach to symptom relief. Psyllium and aloe vera can be consumed orally or applied topically, making them a convenient addition to your hemorrhoid treatment plan.
Probiotics and Prebiotics for Hemorrhoid Prevention
Maintaining a healthy gut microbiome is crucial for overall health, including the prevention of hemorrhoids. Probiotics and prebiotics can help regulate the balance of gut bacteria, reducing symptoms and preventing complications.
– Probiotics are live bacteria and yeasts that are beneficial for gut health. They can help alleviate symptoms such as constipation, diarrhea, and bloating, all of which can contribute to hemorrhoid development. A variety of probiotics are available, including lactobacillus and bifidobacterium.
– Prebiotics, on the other hand, are non-digestible fibers that serve as food for beneficial bacteria. They help promote the growth of healthy gut bacteria, which can reduce inflammation and improve overall health. Examples of prebiotics include inulin and galacto-oligosaccharides.
A healthy gut microbiome is key to preventing hemorrhoids. By incorporating probiotics and prebiotics into your diet, you can promote a balanced gut ecosystem, reducing the risk of hemorrhoid development.
Acupuncture and Acupressure for Hemorrhoid Treatment
Acupuncture and acupressure are alternative therapies that have gained popularity in recent years. While their efficacy in treating hemorrhoids is not universally accepted, some studies suggest they can provide relief.
– Acupuncture involves inserting fine needles into specific points on the body, stimulating the release of certain chemicals and promoting healing. Some studies have shown that acupuncture can reduce pain and inflammation associated with hemorrhoids.
– Acupressure, on the other hand, involves applying manual pressure to specific points on the body. Similar to acupuncture, acupressure can stimulate healing, reduce pain, and promote relaxation.
Acupuncture and acupressure may seem unconventional, but they offer a non-invasive approach to hemorrhoid treatment. While the scientific evidence is limited, these therapies can be considered as part of a comprehensive treatment plan, used in conjunction with conventional treatments.
Seeking Medical Attention and When to Consult a Doctor
Seeking medical attention for hemorrhoids is crucial, especially if your symptoms persist or worsen over time. Untreated hemorrhoids can lead to severe complications, such as anal fissures, painful ulcers, and even bowel obstruction. In this section, we will discuss the importance of seeking medical attention and explain how to determine when to consult a doctor.
When to Consult a Doctor
If you experience any of the following symptoms, it’s essential to consult a doctor:
- Severe pain in the anal or rectal area, especially while sitting or after bowel movements
- Visible hemorrhoids that are large, painful, or bleeding profusely
- Prolonged rectal bleeding that doesn’t stop with conservative treatments
- Difficulty passing stool or feeling a lump in the rectum
- Anal itching or burning sensation that persists
Additionally, you should seek medical attention if you have any underlying medical conditions, such as diabetes, obesity, or a family history of colon cancer.
Types of Doctors Who Can Treat Hemorrhoids
While primary care physicians can diagnose and treat hemorrhoids, there are other specialists who can provide more advanced care. These include:
- Primary Care Physicians (PCPs): Can diagnose and treat mild to moderate hemorrhoids
- Gastroenterologists: Specialize in digestive system diseases, including hemorrhoids and rectal bleeding
- Colorectal Specialists: Highly trained in treating rectal and colon diseases, including hemorrhoids and colon cancer
When seeking medical attention, it’s essential to choose a healthcare provider with experience in treating hemorrhoids. This ensures you receive the best possible care and avoid unnecessary complications.
Urgent Care vs. Emergency Room
If you experience severe, sudden, or life-threatening symptoms, such as intense rectal pain, difficulty breathing, or fever over 101.5°F (38.6°C), seek emergency medical attention. For less severe symptoms, consider visiting an urgent care center or scheduling an appointment with your primary care physician.
“If your symptoms persist or worsen over time, don’t hesitate to seek medical attention. Timely treatment can prevent severe complications and improve your quality of life.”
Final Conclusion
That’s a wrap on how to tell if you have hemorrhoids. Remember, prevention and early detection are key. By understanding the symptoms, risk factors, and contributing conditions, you can take the first step towards a life free from the discomfort and complications of hemorrhoids. So, stay healthy, and stay informed!
FAQ Explained
Q: What is the primary cause of hemorrhoids?
A: The primary cause of hemorrhoids is increased pressure on the veins in the rectum, which can be caused by a variety of factors, including straining during bowel movements, chronic diarrhea, and excessive weight gain.
Q: Can hemorrhoids be prevented?
A: Yes, hemorrhoids can be prevented by maintaining a healthy lifestyle, including a balanced diet, regular exercise, and good hygiene. Additionally, avoiding straining during bowel movements, managing chronic diarrhea, and maintaining a healthy weight can also help prevent hemorrhoids.
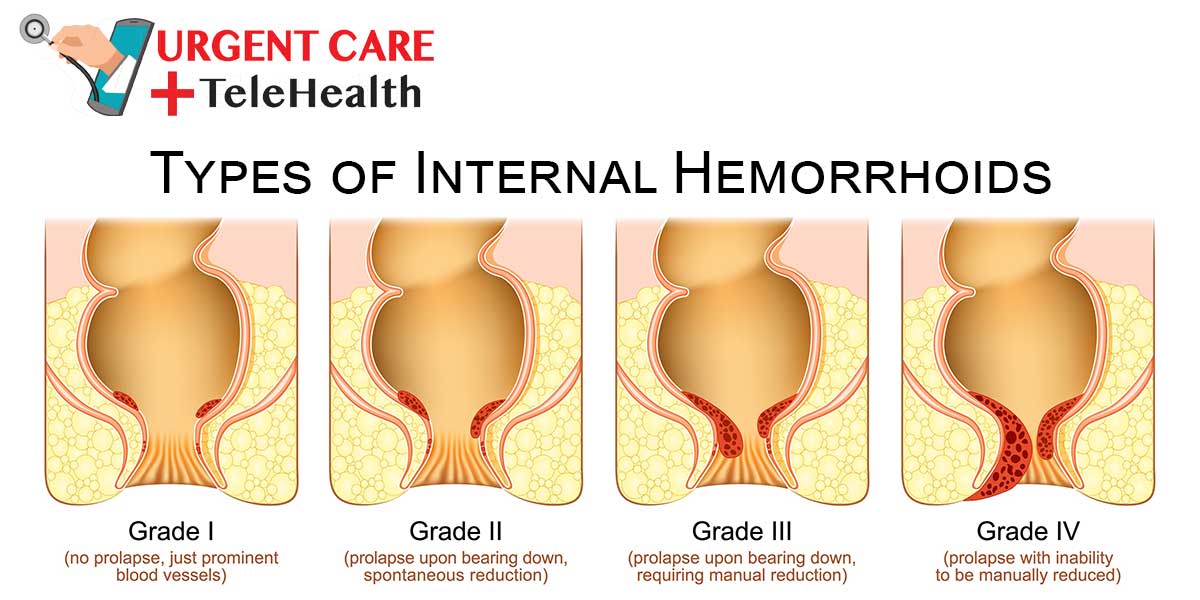
Q: What are the different types of hemorrhoids?
A: There are two main types of hemorrhoids: internal and external. Internal hemorrhoids occur inside the rectum, while external hemorrhoids occur outside the rectum.
Q: Can hemorrhoids be treated with medications and creams?
A: Yes, hemorrhoids can be treated with medications and creams. Over-the-counter creams and ointments, such as witch hazel and hydrocortisone, can help reduce itching and inflammation. However, it’s essential to consult a doctor before using any medications or creams, as they may have side effects and interact with other medications.