How to Tell If You Have Periodontal Disease – This article will take you through the basics of periodontal disease, its impact on oral health, and what you can do to protect your smile. Periodontal disease, also known as gum disease, is a chronic infection of the gums that can lead to bone loss, tooth loss, and even affect your overall health.
Regular dental check-ups are crucial in identifying early signs of periodontal disease. Your dentist can assess your gum health and identify any potential issues before they become serious. But what are the early signs of periodontal disease? In this article, we will dive into the symptoms and signs of periodontal disease and what you can do to prevent and manage it.
Understanding the Basics of Periodontal Disease and Its Impact on Oral Health
Periodontal disease, often referred to as gum disease, is a chronic bacterial infection of the gums and bone that support the teeth. It is a leading cause of tooth loss and has been linked to various systemic diseases. In this section, we will delve into the relationship between periodontal disease and systemic diseases, as well as the differences between gingivitis and periodontitis.
Relationship Between Periodontal Disease and Systemic Diseases
Periodontal disease has been linked to various systemic diseases, such as cardiovascular disease, diabetes, rheumatoid arthritis, and Alzheimer’s disease. The exact mechanisms behind this association are not fully understood, but research suggests that the bacteria that cause periodontal disease can enter the bloodstream and contribute to inflammation and oxidative stress in other parts of the body.
Main Differences Between Gingivitis and Periodontitis
Gingivitis and periodontitis are two stages of periodontal disease that have distinct differences in terms of severity and progression.
Gingivitis is a mild form of periodontal disease that is characterized by inflammation of the gums and is often reversible with proper oral hygiene and professional cleaning.
| Gingivitis | Periodontitis | |
|---|---|---|
| Severity | Mild | Severe |
| Duration | Acute | Chronic |
| Treatment | Reversible with oral hygiene and professional cleaning | Requires surgical intervention and antibiotics to manage symptoms and prevent further progression |
In summary, periodontal disease is a chronic bacterial infection that can have significant implications for oral health and systemic disease. Understanding the relationship between periodontal disease and systemic diseases is crucial for developing effective prevention and treatment strategies to manage and prevent periodontal disease.
Recognizing the Early Signs and Symptoms of Periodontal Disease

Regular dental check-ups are essential in identifying early signs of periodontal disease. Early detection allows for prompt treatment, preventing the progression of the disease and minimizing the risk of complications. A dentist can examine the gums and teeth to detect any signs of inflammation or infection.
During a check-up, your dentist may also ask about your medical history, including any previous dental work or medications that may be contributing to gum disease. Your dentist will also check for other risk factors, such as smoking or excessive sugar consumption, which can increase your risk of developing periodontal disease.
Visual and Physical Symptoms of Periodontal Disease
Periodontal disease can cause a range of visual and physical symptoms, including:
- Gum inflammation (gingivitis): Red, swollen, or bleeding gums
- Bad breath (halitosis)
- Loose teeth
- Changes in the way your teeth fit together when you bite
In its early stages, periodontal disease may not be visible to the naked eye. However, as it progresses, you may notice changes in the appearance of your gums. For example, they may become red, swollen, or bleed easily when you brush or floss.
Gum inflammation (gingivitis) is a key symptom of periodontal disease. It can manifest as follows:
– Red gums: The gums may appear red or inflamed due to an increase in blood flow.
– Swollen gums: The gums may swell due to the collection of bacteria and other substances in the gum pockets.
– Bleeding gums: The gums may bleed when you brush, floss, or eat hard, crunchy, or sticky foods.
Gum inflammation can be a precursor to more severe periodontal disease.
In advanced cases of periodontal disease, the gums may pull away from the teeth, creating deep pockets that trap bacteria and other substances. This can lead to the loss of teeth and other complications.
In addition to visual changes, periodontal disease can cause discomfort and pain in the mouth, making it difficult to perform daily activities such as eating, speaking, or brushing your teeth. In some cases, the disease can also lead to systemic inflammation, which has been linked to various health conditions, such as heart disease and diabetes.
Image 1: A healthy gum line, with the gum tissue fit snugly around the teeth.
Image 2: Red, swollen gum tissue, indicating inflammation.
Image 3: Bleeding gum tissue, a symptom of advanced periodontal disease.
In these images, note the differences in the appearance of the gum tissue. A healthy gum line should be pink and smooth, while inflamed or infected gums may appear red, swollen, or bleed easily.
The Role of Risk Factors in Developing Periodontal Disease
Periodontal disease is a common and often preventable condition that affects millions of people worldwide. Several risk factors contribute to the development and progression of this disease. Understanding these factors can help individuals take proactive steps to protect their oral health and prevent periodontal disease.
Tobacco Use Contributes to Periodontal Disease
=============================================
Tobacco use is a significant risk factor for periodontal disease. Tobacco products contain over 7,000 chemicals, many of which are toxic and can harm the gums, bones, and other tissues in the mouth. Smoking and chewing tobacco can increase the risk of developing periodontal disease by 2-6 times compared to non-smokers.
- Tobacco products reduce blood flow to the gums, making them more susceptible to damage and infection.
- Tobacco smoke contains chemicals that can weaken the bones that support the teeth, leading to tooth loss.
- Tobacco users are more likely to have a higher severity of periodontal disease, making treatment more challenging.
The Relationship Between Diabetes and Periodontal Disease
=====================================================
Diabetes is a complex condition that affects the body’s ability to regulate blood sugar levels. Periodontal disease is 2-3 times more common in people with diabetes than in those without the condition. The relationship between diabetes and periodontal disease is bidirectional, meaning that diabetes can increase the risk of developing periodontal disease, and periodontal disease can worsen blood sugar control.
- High blood sugar levels can damage the blood vessels and nerves that supply the gums, making them more susceptible to damage and infection.
- Periodontal disease can lead to chronic inflammation, which can worsen blood sugar control and make it more challenging to manage diabetes.
- People with diabetes are more likely to develop aggressive periodontal disease, which can lead to rapid progression and tooth loss.
Diagnostic Tools and Methods for Identifying Periodontal Disease
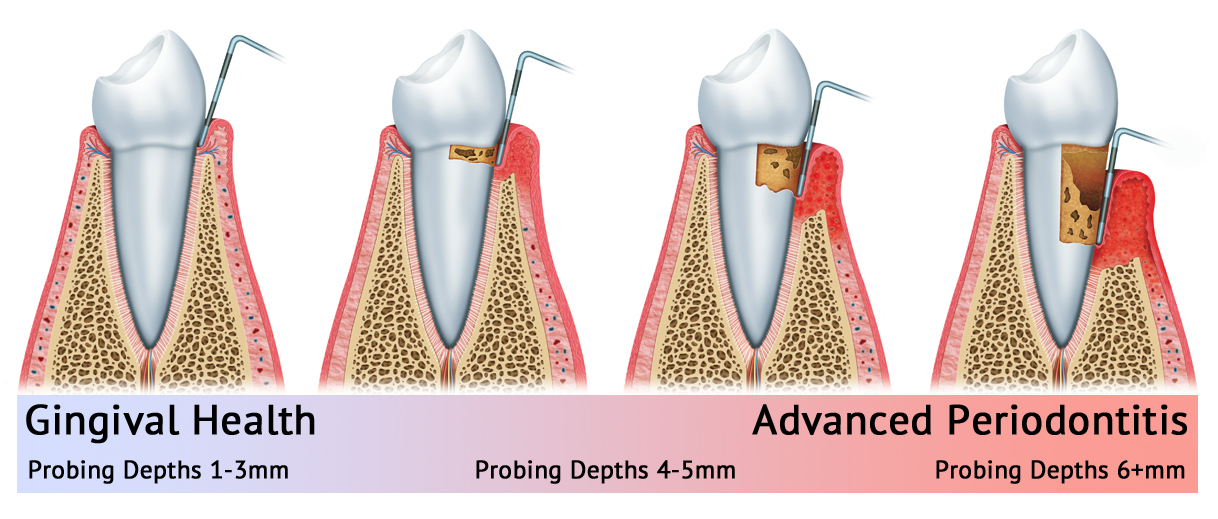
A dental examination is a crucial step in identifying periodontal disease. A thorough examination involves a visual assessment of the teeth, gums, and other oral tissues. The dentist uses various tools to evaluate the gum health, including a periodontal probe to measure the pocket depth between the teeth and gums.
The Role of Visual Examination in Periodontal Disease Diagnosis
During a visual examination, the dentist assesses the gum health by checking for signs of inflammation, bleeding, or swelling. They also inspect the teeth for any signs of decay, cracks, or wear. Additionally, the dentist evaluates the way the teeth fit together and the overall alignment of the teeth.
The Use of Radiographs in Diagnosing Periodontal Disease
Radiographs, also known as x-rays, are widely used in dentistry to detect and diagnose periodontal disease. They provide a detailed image of the teeth, gums, and bone structure, allowing the dentist to identify any signs of periodontal disease, such as bone loss or gum recession.
- Bitewing radiographs are typically used to detect interproximal decay and check for any signs of periodontal disease in the upper and lower teeth.
- Periapical radiographs are used to evaluate the entire tooth structure, including the roots and surrounding bone, to detect any signs of periodontal disease.
- Panoramic radiographs provide a broad view of the entire mouth, allowing the dentist to evaluate the overall status of the oral tissues and identify any potential signs of periodontal disease.
However, radiographs have their limitations. They may not detect early signs of periodontal disease, and some cases may require more advanced imaging modalities, such as cone beam computed tomography (CBCT) scans.
Limitations of Radiographs in Periodontal Disease Diagnosis
Radiographs are not ideal for detecting early signs of periodontal disease, as bone loss may not be apparent at this stage. Furthermore, radiographs may not provide a complete picture of the gum health, as some areas may be difficult to access or may require more advanced imaging modalities.
According to the American Academy of Periodontology, radiographs should be used in conjunction with other diagnostic tools, such as visual examination, to provide a comprehensive evaluation of periodontal health.
Treatment Options for Periodontal Disease and Management Strategies: How To Tell If You Have Periodontal Disease
Preventing the progression of periodontal disease is closely linked to good oral hygiene practices. Regular brushing and flossing are essential in removing plaque and bacteria from teeth and gums, which helps prevent inflammation and infection. In addition to good oral hygiene, attending regular dental check-ups can also help in early detection and treatment of periodontal disease.
Non-Surgical Treatment Options
Non-surgical treatments are often used as the first line of treatment for periodontal disease, and they are generally less invasive than surgical options. These treatments aim to remove plaque and bacteria from the gums and teeth, and to reduce inflammation.
-
Scaling and Root Planing
is a non-surgical procedure that involves the removal of plaque and bacteria from teeth and gums. This is often done using ultrasonic scalers or manual instruments. Scaling and root planing can help reduce inflammation and prevent further progression of the disease.
-
Antibiotic Therapy
involves the use of antibiotics to kill bacteria in the mouth. Antibiotics can be administered in the form of mouthwash, tablets, or gels. Antibiotic therapy can help reduce inflammation and prevent further progression of the disease.
-
Antimicrobial Therapy
involves the use of antimicrobial agents to kill bacteria in the mouth. Antimicrobial agents can be administered in the form of mouthwash, tablets, or gels. Antimicrobial therapy can help reduce inflammation and prevent further progression of the disease.
Surgical Treatment Options
Surgical treatments are often used when non-surgical treatments are not effective, or when the disease has progressed to a more severe stage. Surgical treatments aim to remove infected tissue and bone from the mouth, and to promote healing and regeneration.
-
Pocket Depth Reduction
involves the removal of infected tissue and bone from the pockets between the teeth and gums. This helps reduce the pocket depth and prevent further progression of the disease.
-
Bone Grafting
involves the use of bone grafts to replace lost bone tissue in the mouth. Bone grafting can help restore the natural shape and function of the mouth.
-
Soft Tissue Grafting
involves the use of grafts to replace lost tissue in the gums. Soft tissue grafting can help restore the natural shape and function of the gums.
Preventing and Managing Periodontal Disease at Home
Maintaining good oral hygiene is crucial in preventing and managing periodontal disease. Regular brushing and flossing can help remove plaque and bacteria that can lead to periodontal disease. A combination of proper oral hygiene practices and regular dental cleanings can help prevent and manage periodontal disease at home.
Maintaining Good Oral Hygiene
Maintaining good oral hygiene is essential in preventing periodontal disease. Brushing your teeth at least twice a day with a fluoride toothpaste can help remove plaque and bacteria from your teeth. Flossing at least once a day can help remove food particles and plaque from between your teeth. In addition, regular tongue scraping can help remove bacteria and debris from the surface of your tongue.
- Bristle brush: Use a soft-bristled toothbrush to clean your teeth. The bristles should be small enough to reach between your teeth and along the gumline.
- Fluoride toothpaste: Use a fluoride toothpaste to help prevent tooth decay and strengthen your teeth. Look for a toothpaste with the American Dental Association (ADA) Seal of Acceptance.
- Interdental brushes: Use interdental brushes to clean between your teeth where a regular toothbrush cannot reach.
- Floss: Use floss to remove food particles and plaque from between your teeth and under your gumline.
- Tongue scraper: Use a tongue scraper to remove bacteria and debris from the surface of your tongue.
Regular Dental Cleanings
Regular dental cleanings are essential in preventing and managing periodontal disease. A dental cleaning involves removing plaque and tartar from your teeth to help prevent periodontal disease. A dental cleaning can also help remove stains and freshen your breath. Dental cleanings should be scheduled every 6 months, or as recommended by your dentist.
| Benefits of Regular Dental Cleanings | Description |
|---|---|
| Prevents periodontal disease | Dental cleanings help remove plaque and tartar from your teeth to help prevent periodontal disease. |
| Removes stains | Dental cleanings can help remove stains and discolorations from your teeth. |
| Freshens breath | Dental cleanings can help remove bacteria and debris from your teeth and mouth that can cause bad breath. |
Importance of Regular Check-ups, How to tell if you have periodontal disease
Regular check-ups with your dentist are essential in preventing and managing periodontal disease. Your dentist can help identify any signs of periodontal disease early on, and provide you with guidance on how to improve your oral hygiene. Regular check-ups can also help prevent other oral health problems, such as tooth decay and gum disease.
Regular check-ups with your dentist are more than just a routine appointment – they are essential in maintaining your oral health and preventing periodontal disease.
Closure
In conclusion, identifying periodontal disease early on is crucial in preventing its progression and saving your teeth. Regular dental check-ups, good oral hygiene, and a healthy lifestyle can all contribute to maintaining healthy gums and a beautiful smile. Don’t wait until it’s too late, take care of your teeth today!
FAQ Compilation
Q: What is the difference between gingivitis and periodontitis?
Gingivitis is a mild form of gum disease that can be reversed with good oral hygiene and regular dental check-ups. Periodontitis, on the other hand, is a moreadvanced form of gum disease that can lead to bone loss and tooth loss if left untreated.
Q: Can periodontal disease be treated with antibiotics?
Yes, in some cases, periodontal disease can be treated with antibiotics. However, this is usually only done in conjunction with other treatments such as scaling and root planing, and regular dental check-ups.
Q: Is periodontal disease contagious?
No, periodontal disease is not contagious. It is a bacterial infection that can be spread through poor oral hygiene and lack of regular dental check-ups.
Q: Can periodontal disease affect my overall health?
Yes, research has shown that there is a link between periodontal disease and several other health conditions such as heart disease, diabetes, and respiratory disease.
Q: How often should I visit my dentist for a check-up?
The frequency of dental check-ups depends on your individual oral health needs. However, it is generally recommended to visit your dentist for a check-up every 6 months to prevent and detect any oral health issues early on.